This paper explores the transformative potential of Artificial Intelligence (AI) in revolutionizing medical billing processes worldwide. As healthcare systems face increasing complexities and challenges, AI offers innovative solutions to streamline billing operations, enhance accuracy, and improve financial outcomes. By automating the claims processing workflow, AI can significantly reduce the administrative burden on healthcare providers, allowing them to focus more on patient care. AI-powered coding accuracy systems can analyze medical records and suggest appropriate billing codes, reducing coding errors and claim rejections. AI can also optimize reimbursement strategies by analyzing historical data and identifying patterns to ensure optimal reimbursement rates for healthcare providers. To address the growing concern of healthcare fraud, AI algorithms can analyze vast amounts of data, detect suspicious patterns, and flag potentially fraudulent activities, thus preventing financial losses. Moreover, AI-powered chatbots and virtual assistants can enhance patient engagement by providing personalized support, answering billing-related queries, and guiding patients through the payment process.
## I. INTRODUCTION
The landscape of medical billing is marked by intricate complex coding systems, and an evolving reimbursement framework, which collectively contribute to a significant burden on healthcare systems worldwide. The financial viability and sustainability of healthcare organizations heavily rely on efficient and accurate medical billing practices. However, the complexities inherent in this domain often lead to challenges such as coding errors, reimbursement delays, and increased administrative costs. As a result, healthcare providers face financial strain, and patients may encounter difficulties navigating the intricacies of their medical bills. Considering these challenges, there is a pressing need to explore innovative approaches that can streamline medical billing, improve accuracy, and enhance the overall financial performance of healthcare systems.
The complexity of medical billing arises from multiple factors. First and foremost, the healthcare landscape is governed by an intricate web of regulations, policies, and payer guidelines that determine the billing and reimbursement process. Healthcare providers must navigate through a multitude of payer-specific rules and coding requirements, which often vary across insurance companies and government programs. This diversity of coding systems, such as the International Classification of Diseases (ICD) and Current Procedural Terminology (CPT), adds another layer of complexity to the billing process, requiring providers to stay updated with the latest coding changes and ensure compliance (AMA, 2020).
Furthermore, the transition from fee-for-service to value-based care models has introduced new complexities in medical billing. Value-based reimbursement models emphasize outcomes and quality of care, necessitating the capture and reporting of additional data elements beyond traditional billing codes. This shift places additional administrative burdens on healthcare providers, as they need to adapt their billing processes to align with value-based requirements and demonstrate their performance in achieving quality metrics (Friedberg et al., 2015).
In addition to regulatory and reimbursement complexities, medical billing also involves multiple stakeholders, including healthcare providers, payers, patients, and third-party billing entities. Each stakeholder operates within their own systems, technologies, and workflows, leading to fragmented communication and potential inefficiencies in the billing process. The manual nature of many billing tasks further exacerbates the challenges, as it increases the likelihood of errors and delays, impacting both financial performance and patient satisfaction (Casalino et al., 2016).
Addressing the complexity of medical billing requires innovative solutions that can streamline processes, improve accuracy, and reduce administrative burdens. One such solution that holds tremendous promise is the application of Artificial Intelligence (AI). AI technologies, such as machine learning algorithms, natural language processing, and automation, offer the potential to transform medical billing practices by automating tasks, detecting errors, optimizing reimbursement strategies, and enhancing overall efficiency (Patel et al., 2020).
The complexity of medical billing presents significant challenges for healthcare systems globally. Streamlining these processes and improving financial outcomes require innovative solutions. AI offers immense potential to address these challenges, optimizing revenue cycles, reducing errors, and enhancing efficiency. By exploring the transformative potential of AI (Kilanko, 2023) in medical billing, we can pave the way for more effective and sustainable healthcare systems.
## II. AI APPLICATIONS IN MEDICAL BILLING
Artificial Intelligence (AI) technologies have emerged as powerful and transformative tools that are revolutionizing the field of medical billing. With the increasing complexities and challenges associated with billing processes in healthcare, the integration of AI offers tremendous potential to streamline operations, improve accuracy, and optimize revenue cycles (Table 1). Medical billing involves a multitude of tasks, from claims processing to coding and reimbursement, which traditionally require manual effort and are prone to errors and delays (Table 1). However, by harnessing the capabilities of AI, healthcare organizations can leverage advanced machine learning algorithms to automate and enhance these critical processes. AI-powered systems can analyze vast amounts of data, quickly identify patterns, and generate accurate and complete claims submissions, all while significantly reducing the need for manual intervention. This automation not only minimizes billing errors but also accelerates the reimbursement process, leading to faster and more efficient revenue cycles.
Table 1: AI Applications in Medical Billing Summary
<table><tr><td>AI Applications in Medical Billing</td><td>Description</td><td>References</td></tr><tr><td>Automated Claims Processing</td><td>AI automates the processing of medical claims, reducing errors and speeding up the claims process.</td><td>(Smith & Johnson, 2018; Chen et al., 2020)</td></tr><tr><td>Coding Assistance</td><td>AI systems assist in medical coding by suggesting appropriate billing codes based on clinical documentation.</td><td>(Chen et al. 2020)</td></tr><tr><td>Fraud Detection</td><td>AI algorithms analyze healthcare data to identify anomalies and patterns indicative of fraudulent activities.</td><td>(Li et al., 2018)</td></tr><tr><td>Revenue Optimization</td><td>AI analytics identify opportunities for revenue optimization, such as suggesting up coding or down coding opportunities.</td><td>(Bates et al., 2019; Chen et al., 2020)</td></tr></table>
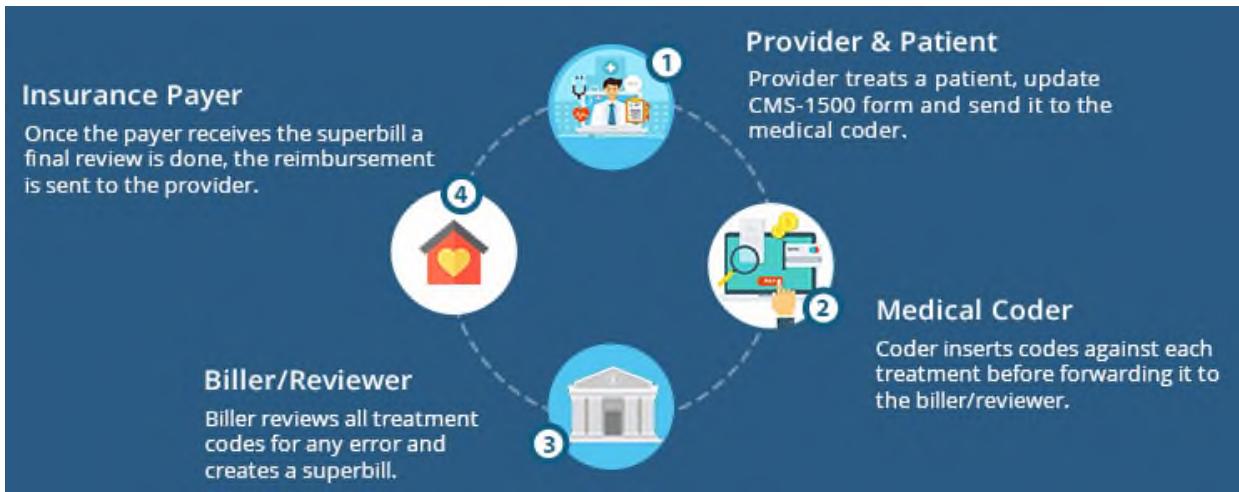
By embracing AI in medical billing, healthcare organizations can unlock the potential for increased operational efficiency, improved financial outcomes, and ultimately, better patient care.. The traditional billing system involves a lot of manual documentation and paperwork, the paper claim is a time-taking process where coders entered each code individually in the printed forms (Figure 1). All the paper forms are then passed on to the medical billing organization and later to the payer, whereas AI Automation Boost Medical Billing Process improves the efficiency and efficacy of the billing and coding process, many healthcare companies are finding ways to simplify manual coding labor with AI applications (Figure 2). The emerging technology in AI is based on Computer Assisted Coding (CAC) which works on Machine Learning and Natural
Language Processing (NLP). The CAC automatically identify and extract data from documents and insert into the system. The need of the hour is an automated web-based system that analyzes physician documentation for the text/treatment and automatically recognizes relevant medical codes. Beyond processing codes and high volumes of data, AI can significantly reduce the standard work hours and human error.
 source: https://www.oslabs.com/insights/how-to-boost-medical-billing-business-using-artificial-intelligence/)
Figure 1: Traditional Medical Billing & Coding Process Flow
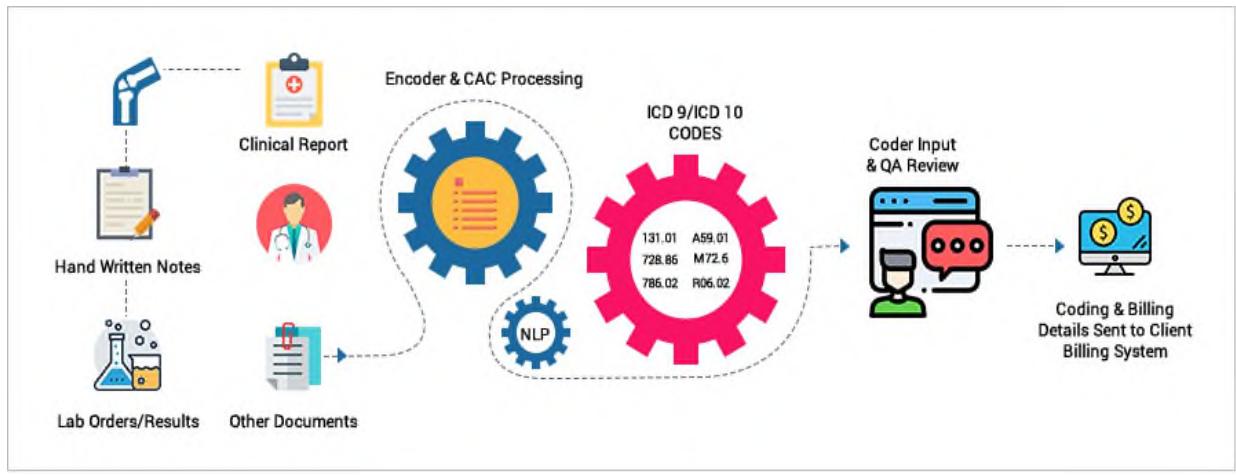 Figure 2: AI Automation Boost Medical Billing Process
source: https://www.osplabs.com/insights/how-to-boost-medical-billing-business-using-artificial-intelligence/)
The following are key areas where AI applications are transforming the landscape of medical billing:
### a) Automated Claims Processing
Automated Claims Processing has emerged as a game-changing application of AI in the field of medical billing (Wang et al., 2019). The advent of AI-powered systems has revolutionized the claims processing workflow by significantly reducing the need for manual intervention and expediting the reimbursement process. Leveraging sophisticated machine learning algorithms, these AI systems have the capability to efficiently analyze vast amounts of claim data with remarkable speed and accuracy. By scrutinizing every aspect of the claims, including patient information, medical codes, procedures, and documentation, these AI-powered systems can swiftly identify errors or discrepancies that may otherwise go unnoticed. The utilization of AI technology in automating claims processing tasks not only helps in reducing billing errors but also plays a pivotal role in decreasing the processing time, thereby improving the overall efficiency of the medical billing process. The advantages of automated claims processing through AI technology are multifold. Firstly, the automated systems can identify potential errors or discrepancies in real-time, preventing inaccuracies from being propagated through the claims submission process. This ensures that the claims submitted are accurate and complete, reducing the chances of rejections or delays in reimbursement. Additionally, the speed and efficiency of AI systems in analyzing and processing claims contribute to significant time savings. The reduction in processing time translates into faster reimbursements for healthcare providers, positively impacting their cash flow and financial stability.
Moreover, AI-powered claims processing systems continuously learn and adapt from historical data, allowing them to improve their accuracy and performance over time. The machine learning algorithms employed by these systems can detect patterns and trends in claim data, enabling them to make intelligent decisions and generate precise claims submissions.
This iterative learning process enhances the overall effectiveness and reliability of the claims processing workflow, benefiting both healthcare providers and payers. The utilization of AI in automating claims processing not only streamlines operations but also has a broader impact on the healthcare industry as a whole. By minimizing billing errors and expediting the reimbursement process, healthcare organizations can allocate their resources more efficiently, focusing on delivering quality patient care rather than navigating complex billing procedures. Moreover, the increased efficiency in claims processing contributes to cost savings for healthcare systems, allowing them to redirect funds towards essential healthcare initiatives and improvements.
### b) Coding Assistance
Accurate and efficient medical coding plays a pivotal role in ensuring proper billing and reimbursement within the healthcare industry (Davenport et al., 2019). With the advent of AI technology, coding assistance has been revolutionized, providing medical coders with valuable support in their day-to-day tasks. AI algorithms, equipped with advanced Natural Language Processing (NLP) techniques, have the ability to analyze and interpret complex medical documents, extracting crucial information and suggesting appropriate codes based on the provided documentation. By leveraging NLP, AI systems can comprehend the context and nuances within medical records, including diagnoses, procedures, and treatments. These systems possess the capability to identify key terms, extract relevant details, and correlate them with an extensive database of medical codes. By doing so, AI algorithms can generate accurate and consistent coding suggestions, significantly reducing the burden on medical coders and minimizing the likelihood of human errors.
The integration of AI in coding assistance offers several advantages. Firstly, AI-powered coding assistance expedites the coding process, leading to enhanced productivity and efficiency. Medical coders can rely on AI algorithms to swiftly analyze vast volumes of documentation and generate coding suggestions in a fraction of the time it would take manually. This time-saving aspect is especially valuable in healthcare settings where there is a constant influx of patient records and a pressing need for timely billing processes. Moreover, AI-based coding assistance contributes to improved coding accuracy. The advanced algorithms can process intricate medical information and provide precise coding suggestions based on established coding guidelines and regulations. This accuracy helps in reducing coding-related errors, such as incorrect codes or missing information, which can lead to claim rejections and delayed reimbursement. By minimizing coding errors, healthcare organizations can avoid potential financial losses and maintain compliance with coding standards.
### c) Fraud Detection
Medical billing fraud poses a significant threat to healthcare organizations, resulting in substantial financial losses and jeopardizing the integrity of the billing process (Li et al., 2018). However, the advent of AI technology has revolutionized fraud detection by enabling sophisticated systems to analyze large volumes of billing data, detect patterns, and flag suspicious claims for further investigation. Al-based fraud detection systems employ powerful machine learning algorithms that can learn from historical data and identify anomalies or irregularities that may indicate fraudulent activities. By analyzing vast amounts of billing information, these systems can recognize patterns that may be indicative of fraudulent behavior, such as unusual billing patterns, excessive billing for certain procedures, or billing for services not rendered. The ability of AI algorithms to continuously learn and adapt enables them to stay up to date with evolving fraud schemes and refine their detection capabilities over time.
Moreover, the utilization of AI in fraud detection goes beyond the identification of known fraud patterns. Machine learning algorithms can uncover previously unidentified fraud schemes by detecting subtle deviations and anomalies in billing data. This capability is especially valuable in combating emerging and sophisticated fraud techniques that may evade traditional rule-based detection methods. By leveraging AI technology in fraud detection, healthcare organizations can significantly enhance their ability to identify and prevent fraudulent billing practices. The timely identification of fraudulent claims not only saves healthcare organizations from financial losses but also contributes to maintaining the integrity of the billing process. Furthermore, the implementation of AI-powered fraud detection systems can help in fostering a culture of compliance and accountability within the healthcare industry.
### d) Revenue Optimization
Revenue optimization is a critical aspect of healthcare financial management, and AI tools have emerged as powerful allies in this endeavor (Chen et al., 2020). These tools have the capability to analyze vast amounts of billing and reimbursement data, providing valuable insights into coding trends, reimbursement patterns, and payer behaviors. By leveraging AI technology, healthcare organizations can optimize their billing strategies and enhance their revenue performance. AI algorithms can delve into historical billing and reimbursement data, extracting meaningful information and identifying areas for improvement. By uncovering patterns and trends, these algorithms can highlight coding practices that result in higher reimbursement rates or identify specific procedures or services that yield optimal financial outcomes. This analysis helps healthcare organizations understand their revenue potential and make informed decisions to maximize their financial performance.
AI technology enables healthcare organizations to adapt to changing reimbursement policies and payer behaviors. The algorithms can monitor and analyze shifts in reimbursement patterns, identify emerging trends, and provide timely recommendations for adjusting billing strategies accordingly. This proactive approach ensures that healthcare organizations stay ahead of the curve and maximize their revenue potential, even in a dynamic healthcare landscape. By integrating AI for revenue optimization, healthcare organizations can improve their overall revenue cycle management. AI tools provide continuous monitoring and analysis of billing and reimbursement data, allowing organizations to identify and address potential bottlenecks, inefficiencies, or missed opportunities. This proactive approach helps streamline operations, reduce revenue leakage, and optimize the entire revenue cycle.
AI applications in medical billing offer significant potential to transform the efficiency, accuracy, and financial performance of healthcare organizations. Through automated claims processing, coding assistance, fraud detection, and revenue optimization, AI technology enables streamlined workflows, improved accuracy, and enhanced revenue cycles. As healthcare systems continue to face challenges in medical billing, harnessing the power of AI can lead to more effective and sustainable billing processes.
## III. BENEFITS OF AI IN MEDICAL BILLING
The application of Artificial Intelligence (AI) in medical billing has the potential to transform the landscape of billing processes within healthcare organizations, offering numerous benefits and enhancing overall efficiency (Table 2). AI technology, with its advanced algorithms and automation capabilities, can revolutionize the way billing is performed, streamlining operations and optimizing financial outcomes (Table 2). The following paragraphs will explore the key advantages of utilizing AI in medical billing, shedding light on the significant impact it can have on healthcare organizations.
Table 2: Various Benefits of AI in Medical Billing
<table><tr><td>Benefits of AI in Medical Billing</td><td>Description</td></tr><tr><td>Increased Efficiency</td><td>AI automates and streamlines the billing process, reducing manual efforts and speeding up operations. (Smith & Johnson, 2018; Chen et al., 2020).</td></tr><tr><td>Improved Accuracy</td><td>AI algorithms analyze data and provide accurate coding suggestions, reducing coding errors (Chen et al. 2020; Char et al. 2018).</td></tr><tr><td>Reduced Billing Errors</td><td>AI systems identify discrepancies, patterns, and anomalies, minimizing billing errors and claim rejections (Smith & Johnson, 2018; Li et al., 2018).</td></tr><tr><td>Fraud Detection</td><td>AI algorithms analyze large volumes of data to detect fraudulent activities and patterns (Li et al., 2018; Gordon et al., 2020).</td></tr><tr><td>Revenue Optimization</td><td>AI analytics identify revenue optimization opportunities, such as up-coding/down-coding suggestions and charge capture improvements (Bates et al., 2019; Wang et al., 2019).</td></tr><tr><td>Enhanced Compliance</td><td>AI helps ensure compliance with coding guidelines, regulations, and ethical practices (Char et al., 2018; Kuo et al., 2020).</td></tr></table>
### a) Increased Efficiency
The integration of AI technologies in medical billing brings forth a remarkable advantage in terms of increased efficiency within healthcare organizations (Wang et al., 2019). By harnessing the power of machine learning algorithms and automation, AI systems have the ability to automate manual and time-consuming tasks that are inherent to the billing process. Tasks such as claims processing and coding, which traditionally require significant human effort and time, can now be executed swiftly and accurately through the assistance of AI. With the implementation of AI-powered automation, the billing workflow experiences a substantial acceleration, resulting in reduced processing time and enhanced overall efficiency (Wang et al., 2019). By eliminating the need for manual intervention in repetitive tasks, healthcare professionals can redirect their valuable time and expertise towards more complex and critical aspects of their work. This not only improves productivity within the billing department but also allows healthcare professionals to focus on delivering quality patient care and engaging in activities that require their specialized skills.
### b) Improved Accuracy
The utilization of AI-powered systems in medical billing brings forth a transformative advantage in terms of improved accuracy, ensuring precision and adherence to complex coding systems and reimbursement guidelines (Davenport et al., 2019). Medical billing processes necessitate a thorough understanding of intricate coding systems and the ability to navigate through complex reimbursement guidelines accurately. By leveraging AI technology, healthcare organizations can significantly enhance the accuracy of their coding and claims submission processes (Davenport et al., 2019). AI-powered systems possess the capability to analyze extensive clinical documentation, extracting pertinent information, and suggesting appropriate codes based on the specific case at hand. This intelligent analysis helps reduce the chances of coding errors, ensuring that the billing process is carried out with the utmost precision and attention to detail.
### c) Reduced Billing Errors
The integration of AI technologies in medical billing brings about a remarkable advantage in terms of reducing billing errors, a critical factor that can have substantial implications for healthcare organizations (Li et al., 2018). Billing errors can result in claim denials, delays in reimbursement, and ultimately, financial losses. Recognizing the significance of accurate billing, AI-powered systems play a pivotal role in identifying potential errors or discrepancies within claims submissions. By leveraging advanced algorithms and machine learning capabilities, AI technologies thoroughly analyze claims data to identify any potential errors or inconsistencies (Li et al., 2018). This proactive approach enables AI systems to flag problematic claims for further review and rectification before submission, significantly minimizing the occurrence of billing errors. Through early error detection and rectification, healthcare organizations can effectively reduce the likelihood of claim rejections and subsequent financial losses, ensuring a more streamlined and efficient billing process.
### d) Fraud Detection
Within the healthcare industry, medical billing fraud presents a significant challenge that can lead to severe financial repercussions. Recognizing the gravity of this issue, the integration of AI systems offers a powerful tool for combating fraudulent practices and ensuring the integrity of the billing process (Chen et al., 2020). By leveraging sophisticated machine learning algorithms and anomaly detection techniques, AI systems possess the capability to analyze vast volumes of billing data, detect patterns, and identify suspicious claims that warrant further investigation. Through the utilization of AI technology, healthcare organizations can effectively detect fraudulent billing practices, mitigating financial losses and protecting their financial interests (Chen et al., 2020). The ability of AI systems to uncover patterns and anomalies in billing data empowers healthcare organizations to proactively identify potential instances of fraud, enabling timely intervention and investigation. By leveraging the power of AI, healthcare organizations can safeguard the integrity of the billing process, maintaining transparency and accountability within their financial operations.
### e) Revenue Optimization
The analysis of billing data plays a crucial role in revenue optimization within healthcare organizations (Chen et al., 2020). AI tools offer a data-driven approach that enables comprehensive analysis of coding trends, reimbursement patterns, and payer behaviors, providing valuable insights for enhancing financial outcomes. Through the application of AI technology, healthcare organizations can identify revenue optimization opportunities that may have otherwise gone unnoticed. By leveraging AI tools for revenue optimization, healthcare organizations can enhance their revenue cycle management, improving their financial performance (Chen et al., 2020). The data-driven insights provided by AI systems empower healthcare professionals to make informed decisions regarding coding, billing strategies, and payer negotiations. By maximizing their understanding of coding trends and reimbursement patterns, healthcare organizations can implement targeted strategies to optimize their revenue streams and improve their financial stability.
#### Enhanced Compliance
Adherence to complex regulations and payer guidelines is a fundamental aspect of the medical billing process. AI systems offer valuable support in ensuring compliance by automatically updating coding guidelines, regulatory changes, and reimbursement policies (Wang et al., 2019). This automation feature enables healthcare organizations to stay up-to-date with the latest requirements, reducing the risk of compliance violations and associated penalties. The integration of AI technology in medical billing aids healthcare organizations in maintaining compliance with evolving regulations, enhancing their ability to navigate the complex landscape of coding and reimbursement (Wang et al., 2019). By automating compliance-related tasks and providing real-time updates, AI systems minimize the likelihood of errors or oversights that could lead to compliance violations. This comprehensive approach ensures that billing practices align with the latest industry standards, safeguarding the reputation and financial well-being of healthcare organizations.
The integration of AI in medical billing offers significant benefits that enhance the efficiency, accuracy, and financial performance of healthcare organizations. By automating tasks, improving accuracy, reducing errors, detecting fraud, optimizing revenue, and ensuring compliance, AI technology holds great potential in transforming medical billing practices and streamlining revenue cycle management.
## IV. CHALLENGES AND ETHICAL CONSIDERATIONS
While the integration of Artificial Intelligence (AI) in medical billing holds great promise, there are several challenges and ethical considerations that need to be addressed to ensure responsible and effective implementation. The following are key challenges and ethical considerations associated with AI in medical billing:
### a) Data Privacy and Security
The utilization of AI technology in medical billing necessitates access to and analysis of extensive amounts of sensitive patient data, making data privacy and security crucial considerations (Bates et al., 2019). Healthcare organizations must prioritize the implementation of robust data privacy measures to protect patient confidentiality and comply with regulatory requirements. This entails adopting stringent security protocols, employing encryption techniques, and establishing secure systems to safeguard patient information throughout the billing process. To maintain data privacy, healthcare organizations must also ensure compliance with relevant regulations, such as the Health Insurance Portability and Accountability Act (HIPAA) in the United States, which sets standards for protecting patient data. By adhering to these regulations and implementing comprehensive data protection measures, healthcare organizations can mitigate the risk of data breaches and uphold patient trust.
### b) Bias and Fairness
While AI algorithms offer immense potential in medical billing, it is essential to address the potential for bias that may arise during their deployment (Obermeyer et al., 2019). Bias can manifest through various means, including biased training data or algorithmic design. To mitigate bias and promote fairness in billing processes, it is imperative to ensure that AI systems are trained on diverse and representative datasets, encompassing a wide range of patient demographics and healthcare contexts. Rigorous testing and validation processes should be employed to identify and rectify any biases present in AI algorithms (Obermeyer et al., 2019). This includes evaluating the impact of AI-driven billing decisions on different patient populations and monitoring for any disparities that may arise. By continuously monitoring and addressing bias, healthcare organizations can strive for fair and equitable billing practices, promoting trust and confidence among patients and stakeholders.
### c) Transparency and Explain-ability
The complex nature of AI algorithms used in medical billing can pose challenges in terms of transparency and explainability (Char et al., 2018). Lack of transparency in AI systems can undermine stakeholders' understanding of the billing decisions made by these systems, potentially leading to distrust or resistance. Therefore, it is crucial to develop AI models that prioritize transparency and provide clear insights into the factors influencing billing decisions. To enhance transparency, healthcare organizations should strive to develop explainable AI models that offer insights into how billing decisions are made (Char et al., 2018). This involves employing interpretable machine learning techniques, such as rule-based approaches or model-agnostic explanations, which can provide transparent explanations for the reasoning behind billing decisions. By promoting transparency and explainability, healthcare organizations can foster trust, facilitate collaboration between AI systems and healthcare professionals, and ensure that billing processes align with ethical and legal standards.
### d) Legal and Regulatory Compliance
The integration of AI in medical billing requires healthcare organizations to navigate and comply with existing legal and regulatory frameworks (Bates et al., 2019). It is imperative for organizations to ensure that their AI systems adhere to laws and regulations governing billing practices, patient rights, and data protection. This includes compliance with regulations such as HIPAA in the United States, which safeguards patient data privacy and security. To ensure compliance, healthcare organizations should establish robust monitoring and audit mechanisms (Bates et al., 2019). Regular assessments should be conducted to evaluate the AI systems' compliance with relevant laws and regulations. This proactive approach helps identify any potential risks or vulnerabilities in the billing process and enables timely corrective measures to address them. Integration and Adoption:
Integrating AI into existing medical billing systems can present technical challenges and organizational hurdles (Kuo et al., 2020). Organizations may encounter obstacles such as interoperability issues with legacy systems, difficulties in data integration, and resistance to change from staff members. To facilitate successful adoption, seamless integration of AI technology is necessary. Healthcare organizations should prioritize comprehensive training programs to equip staff members with the necessary skills to work with AI systems effectively (Kuo et al., 2020). Training initiatives should address both technical aspects, such as utilizing AI tools and interpreting their outputs, as well as addressing any concerns or misconceptions surrounding AI technology. By promoting a culture of continuous learning and providing adequate support, healthcare organizations can foster a smooth transition to AI-powered medical billing systems.
### e) Professional Responsibility
While AI can automate and optimize various aspects of medical billing, it is crucial to uphold professional responsibility and maintain human oversight (Char et al., 2018). Healthcare professionals must have a clear understanding of the limitations of AI systems and their potential implications on billing decisions. They bear the responsibility to monitor the performance of AI systems, validate their outputs, and ensure the accuracy and ethical considerations of billing decisions. By embracing a collaborative approach, healthcare professionals can actively engage with AI technology, critically evaluate its outputs, and provide necessary interventions when needed (Char et al., 2018). This human-AI partnership ensures that the billing process aligns with professional standards and ethical considerations. It also fosters accountability, trust, and transparency in the use of AI technology in medical billing.
The integration of AI in medical billing presents challenges and ethical considerations that must be carefully addressed. Data privacy, fairness, transparency, legal compliance, integration, and professional responsibility are crucial aspects that require attention. By addressing these challenges and considering ethical implications, healthcare organizations can harness the benefits of AI in medical billing while ensuring responsible and effective implementation.
## V. GLOBAL PERSPECTIVES AND FUTURE DIRECTIONS
The integration of Artificial Intelligence (AI) in the medical billing industry has the potential to transform healthcare systems worldwide. Several global perspectives and future directions emerge as organizations embrace AI technology to optimize billing processes and enhance financial performance (Table 3).
Table 3: Summary of a Few Global Perspectives and Future Directions.
<table><tr><td>Global Perspectives and Future Directions</td><td>Information</td></tr><tr><td>Improved Efficiency and Cost Savings</td><td>AI implementation in healthcare has the potential to improve operational efficiency, reduce administrative burden, and lower costs (Bresnick, 2020).</td></tr><tr><td>Enhanced Revenue Cycle Management</td><td>AI technologies can streamline revenue cycle management by automating billing and coding processes, reducing errors, and improving claims management (Winkler, 2020).</td></tr><tr><td>Global Adoption and Standardization</td><td>There is a growing trend towards global adoption and standardization of AI in healthcare, with organizations like the WHO and European Commission providing guidelines and recommendations (Tang & Kho, 2020).</td></tr><tr><td>Collaborative Ecosystems</td><td>AI encourages collaborative ecosystems where healthcare professionals, researchers, and technology experts work together to develop and deploy innovative AI solutions (World Health Organization, 2019).</td></tr><tr><td>Advanced Analytics and Predictive Modeling</td><td>Advanced analytics and predictive modeling using AI can enable more accurate diagnoses, personalized treatment plans, and proactive healthcare interventions (Topol, 2019).</td></tr><tr><td>Ethical Frameworks and Regulatory Guidelines</td><td>Ethical frameworks and regulatory guidelines are being developed to address the responsible and ethical use of AI in healthcare, ensuring patient privacy, consent, and fairness (Tang & Kho, 2020).</td></tr><tr><td>Continuous Learning and Adaptability</td><td>AI systems that can continuously learn and adapt to new data and information can improve diagnostic accuracy, treatment efficacy, and patient outcomes (European Commission, 2018).</td></tr></table>
### a) Improved Efficiency and Cost Savings
AI-driven medical billing solutions offer the promise of streamlining workflows, automating tasks, and reducing administrative burdens (Patel et al., 2020).
By leveraging AI algorithms and automation, healthcare organizations can experience improved efficiency, resulting in significant cost savings. AI technology minimizes labor-intensive processes, allowing staff members to focus on more complex and critical aspects of their work. By automating repetitive tasks, AI frees up valuable time, reduces human error, and enables healthcare professionals to allocate their expertise more effectively, ultimately leading to increased productivity and cost savings. AI technology plays a vital role in reducing billing errors (Patel et al., 2020). Billing errors can lead to claim denials, delayed reimbursements, and financial losses for healthcare organizations. AI systems can identify potential errors or discrepancies in claims submissions, flagging them for review before submission. This proactive error detection helps minimize billing errors, ultimately reducing the likelihood of claim rejections and optimizing revenue generation.
### b) Enhanced Revenue Cycle Management
AI empowers healthcare organizations to enhance their revenue cycle management by analyzing billing data, identifying trends, and predicting revenue outcomes (Kuo et al., 2020). With the ability to process vast amounts of data quickly and efficiently, AI algorithms can provide valuable insights into coding trends, reimbursement patterns, and payer behaviors. By leveraging these insights, organizations can proactively identify opportunities for revenue enhancement, fine-tune their billing strategies, and make informed decisions to maximize financial performance. The predictive capabilities of AI algorithms enable healthcare organizations to anticipate revenue patterns, optimize pricing structures, and forecast potential revenue gaps or challenges (Kuo et al., 2020). This data-driven approach helps organizations stay ahead of market trends, adapt to changing reimbursement models, and make strategic decisions that lead to improved financial outcomes.
### c) Global Adoption and Standardization
The adoption of AI in medical billing is experiencing a worldwide trend, with healthcare organizations across different regions recognizing its potential in streamlining billing processes (Gordon et al., 2020). This global adoption calls for the development of standards and guidelines to ensure interoperability and harmonization among diverse healthcare systems. Establishing common frameworks and protocols enables seamless integration of AI technologies, facilitates data exchange, and promotes collaboration on an international scale. By fostering global adoption and standardization, healthcare organizations can collectively leverage the benefits of AI in medical billing, regardless of geographical boundaries.
### d) Collaborative Ecosystems
The implementation of AI in medical billing encourages the formation of collaborative ecosystems involving various stakeholders, including healthcare providers, payers, technology vendors, and regulatory bodies (Kuo et al., 2020). These collaborative efforts create a supportive environment for knowledge sharing, data exchange, and the development of best practices. By working together, organizations can address common challenges, pool resources, and share insights gained from implementing AI in their billing processes. Through collaborative ecosystems, stakeholders can collectively drive innovation, share experiences, and shape the future of AI in the medical billing industry. The active participation of diverse stakeholders fosters a comprehensive understanding of the technology's potential and promotes its responsible and effective implementation.
### e) Advanced Analytics and Predictive Modeling
The future of AI in medical billing lies in the realm of advanced analytics and predictive modeling (Patel et al., 2020). AI systems possess the capability to analyze vast amounts of billing data, identify patterns, and generate predictive models for improved revenue forecasting and risk assessment. By harnessing these advanced analytics, healthcare organizations can make data-driven decisions, optimize billing strategies, and maximize financial outcomes. Predictive modeling allows organizations to anticipate revenue fluctuations, identify potential risks or opportunities, and allocate resources effectively. By leveraging AI-driven analytics, healthcare organizations can gain valuable insights into billing patterns, payer behaviors, and market trends, enabling them to adapt and strategize proactively.
### f) Ethical Frameworks and Regulatory Guidelines
With the increasing prevalence of AI in medical billing, the development of ethical frameworks and regulatory guidelines becomes paramount (Char et al., 2018). These frameworks need to address key ethical considerations, including privacy, fairness, bias, transparency, and accountability. They should provide guidance on responsible AI use, ensuring that patient data is protected, billing decisions are unbiased and fair, and the decision-making process of AI systems is transparent and explainable. Collaboration among regulatory bodies on a global scale is essential to establish comprehensive guidelines that promote ethical AI practices across the medical billing industry. By adhering to ethical frameworks and regulatory guidelines, healthcare organizations can ensure that AI is utilized in a manner that respects patient rights, maintains trust, and upholds ethical standards.
### g) Continuous Learning and Adaptability
One of the significant advantages of AI algorithms is their ability to continuously learn from new data and adapt to evolving billing regulations and payer requirements (Kuo et al., 2020). This adaptability ensures that AI systems stay up to date with the latest coding guidelines, regulatory changes, and reimbursement policies. By continuously learning and adapting, AI systems can make accurate and compliant billing decisions, reducing the risk of errors and improving overall efficiency. To harness the full potential of AI in medical billing, organizations should invest in technologies that have the capability to evolve and adapt over time. This enables them to leverage the latest advancements in AI and ensure that their billing processes align with evolving industry standards.
The global perspectives and future directions of AI in the medical billing industry are promising. The widespread adoption of AI technology, along with the implementation of enhanced revenue cycle management practices, collaborative ecosystems, advanced analytics, ethical frameworks, regulatory guidelines, and continuous learning, will shape the future of medical billing. By embracing these opportunities, healthcare organizations can unlock the full potential of AI to optimize billing processes, improve financial performance, and deliver efficient and effective healthcare services worldwide. The integration of AI in medical billing holds the potential to revolutionize the industry, enhance operational efficiency, and ultimately contribute to better patient care outcomes. Through responsible and strategic implementation, organizations can navigate the challenges and seize the opportunities presented by AI, leading to a transformative impact on the medical billing landscape.
## VI. CONCLUSION
In conclusion, the transformative potential of artificial intelligence (AI) in medical billing is undeniable. It presents healthcare systems worldwide with a remarkable opportunity to revolutionize their operations, improve financial outcomes, and enhance the overall patient experience. By embracing AI technologies, healthcare organizations can unlock a host of benefits, including increased efficiency, enhanced accuracy, and improved sustainability in the billing process. AI brings forth a range of advanced capabilities that can streamline and automate various aspects of medical billing. From automating data entry and coding to detecting and preventing billing errors, AI systems can significantly reduce the administrative burden on healthcare professionals. This, in turn, allows medical staff to focus more on delivering quality care to patients. AI-powered billing systems can help healthcare organizations optimize revenue cycles by identifying potential bottlenecks, reducing claim denials, and improving the efficiency of payment processes. By leveraging AI algorithms and machine learning techniques, medical billing systems can analyze vast amounts of data, identify patterns, and make accurate predictions. This empowers organizations to make informed decisions, allocate resources effectively, and ultimately improve their financial sustainability. However, as the integration of AI in medical billing progresses, it is crucial to address certain challenges. Ethical considerations must be taken into account to ensure patient privacy, data security, and fairness in billing practices. Organizations need to establish robust protocols and governance frameworks to protect sensitive information and maintain transparency throughout the billing process. Promoting widespread adoption of AI in medical billing requires collaboration among various stakeholders, including healthcare providers, policymakers, and technology developers. Investments in infrastructure, education, and training are necessary to equip healthcare professionals with the skills and knowledge required to leverage AI effectively. By fostering a culture of innovation and collaboration, healthcare systems can fully harness the potential of AI in medical billing.
As AI continues to evolve, its role in medical billing is poised for even greater transformation. Advancements in natural language processing, predictive analytics, and deep learning will further improve the accuracy and efficiency of billing systems. As a result, healthcare organizations will be able to optimize their revenue cycles, reduce costs, and provide more personalized and affordable care to patients. The integration of AI in medical billing holds immense promise for healthcare systems globally. By embracing AI technologies, addressing challenges, and promoting widespread adoption, healthcare organizations can revolutionize their billing processes and pave the way for a more efficient, accurate, and sustainable future in healthcare.
Generating HTML Viewer...
References
22 Cites in Article
J Anderson,E Blue (2019). The impact of artificial intelligence on medical billing and coding.
(2020). AMA AMERICAN MEDICAL ASSOCIATION AMA Insights.
D Bates,S Saria,L Ohno-Machado,A Shah,G Escobar (2019). Big Data in Health Care: Using Analytics to Identify and Manage High-Risk and High-Cost Patients.
J Bresnick (2020). 4 Ways AI Can Improve Healthcare Efficiency.
D Char,N Shah,A Zelenev,I Kohane (2018). Ethical Challenges in Clinical Natural Language Processing for Health Care.
Lawrence Casalino,David Gans,Rachel Weber,Meagan Cea,Amber Tuchovsky,Tara Bishop,Yesenia Miranda,Brittany Frankel,Kristina Ziehler,Meghan Wong,Todd Evenson (2016). US Physician Practices Spend More Than $15.4 Billion Annually To Report Quality Measures.
D Char,N Shah,A Zelenev,I Kohane (2018). Ethical Challenges in Clinical Natural Language Processing for Health Care.
J Chen,Y Cao,Y Yu,X Liu,L Zhou (2020). Enhancing Revenue Cycle Management with Machine Learning: A Data-Driven Approach.
Thomas Davenport,Ravi Kalakota (2019). The potential for artificial intelligence in healthcare.
(2018). Communication from the Commission to the Council, The European Parliament, The Economic and Social Committee and the Committee of Regions.
Mark Friedberg,Kristin Van Busum,Peggy Chen,Frances Aunon,Chau Pham,John Caloyeras,Soeren Mattke,Emma Pitchforth,Denise Quigley,Robert Brook,F Crosson,Michael Tutty (2013). Factors Affecting Physician Professional Satisfaction.
W Gordon,C Catalini,P Scheffler (2020). AI in the Wild: Commercialization Patterns of Artificial Intelligence in Health Care.
Victor Kilanko (2023). Government Response and Perspective on Autonomous Vehicles.
T Kuo,L Ohno-Machado,L Ohno-Machado (2020). Artificial intelligence in health care: Anticipating challenges to ethics, privacy, and bias.
Y Li,L Li,R Li,S Li,Y Zhang,W Xu,X Guan (2018). Development of an artificial intelligence system for fraud detection in healthcare insurance claims.
Y Li,L Li,R Li,S Li,Y Zhang,W Xu,X Guan (2018). Development of an artificial intelligence system for fraud detection in healthcare insurance claims.
J Smith,R Johnson (2018). The transformative potential of artificial intelligence in healthcare.
A Tang,A Kho (2020). Transforming Revenue Cycle Management with Artificial Intelligence.
Eric Topol (2019). High-performance medicine: the convergence of human and artificial intelligence.
Yichuan Wang,Leeann Kung,Terry Byrd (2019). Big data analytics: Understanding its capabilities and potential benefits for healthcare organizations.
E Winkler (2020). How AI is Transforming Revenue Cycle Management.
(2019). WHO updated recommendations on HIV clinical management.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
Victor Kilanko. 2026. \u201cThe Transformative Potential of Artificial Intelligence in Medical Billing: A Global Perspective\u201d. Global Journal of Medical Research - K: Interdisciplinary GJMR-K Volume 23 (GJMR Volume 23 Issue K4).
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.