## I. INTRODUCTION
Preterm labor refers to the onset of labor after fetal viability but before 37 completed weeks of gestation. The diagnostic criteria are onset of increasingly frequent and painful uterine contractions (atleast 4 contractions per 20 minutes) with progressive effacement and dilatation of the cervix i.e., $80\%$ cervical effacement and atleast 2cm dilatation (or cervical length $< 1\mathrm{cm}$ ).
It is a major challenge in perinatal health care. Preterm birth occurs in $5\%$ to $18\%$ of all deliveries worldwide. It is estimated that 15 million preterm births occur each year with 1.1 million infants dying from preterm birth complications. $^{1}$ Prediction of preterm labor enables taking early action for preterm birth as in- utero transfer to tertiary care centres, reasonable administration of corticosteroids while avoiding un-necessary use, magnesium sulphate treatment for neuroprotective effect and antibiotic treatment in case of infection.2
Current screening tests for the prediction of preterm labor can be divided into three general categories:-
1) Risk factor assessment
2) Cervical measurement
3) Bio-chemical markers
One of the early changes that precede preterm birth is cervical shortening, which may be detected even several weeks prior to the onset of active labor. But due to limitations in ultrasound availability and operator expertise, cervical length alone cannot be reliably utilised to predict preterm labor or used as routine screening tool. $^3$
Cervico-vaginal fluid, a complex mixture of secretions from vagina, endocervix, endometrial decidua and amniochorion serves as an important diagnostic tool for preterm labor prediction. Two most commonly used biochemical markers used for prediction of preterm labor are -fetal fibronectin and phosphorylated Insulin like growth factor binding protein-1(ph-IGFBP-1).
Fetal fibronectin is a glycoprotein produced by amniocytes and cytotrophoblasts. It is normally found in cervico-vaginal fluid before 22 weeks of gestation but its presence between 24 to 34 weeks of gestation indicates a risk of preterm birth. But this test has several disadvantages or limitations including high cost, limited availability, sexual intercourse or vaginal examination interferes with the test and reduces its accuracy
Phosphorylated Insulin like growth factor binding protein -1 (ph-IGFBP-1) was requested as a marker for predicting preterm birth for being positive at significantly higher rates in cervical fluids of patients with preterm birth. An immune chromatographic test (one step dipstick test) detects ph-IGFBP-1 in cervix, can be used from 22 weeks onwards with fast results. Test results are not affected by urine, intercourse semen, vaginal medications, lubricants or infections.It has $98\%$
(high) negative predictive value that helps to avoid unnecessary treatment and reduces cost. $^4$
## II. AIM AND OBJECTIVES
To predict preterm deliveries in symptomatic patients.
To assess sensitivity, specificity, positive predictive value and negative predictive value of the phosphorylated Insulin like Growth Factor Binding Protein-1 test for prediction of preterm labour in symptomatic patients.
## III. MATERIALS AND METHODS
The study was conducted in the Department of Obstetrics and Gynaecology, SMS Medical College, Jaipur. Women with singleton pregnancy 28 to 37 weeks of gestation with intact fetal membranes, who presented with threatened preterm labour were included in the study after taking written informed consent. Pregnant women with Preterm premature rupture of membranes (PPROM), advanced preterm labour, those women who require iatrogenic preterm induction of labor were excluded.
The study sample was 78 cases and they were subjected to detailed history if any were noted. Abdominal examination was done for presentation of fetus and frequency of uterine contractions. Amniotic fluid leak was confirmed on per speculum examination and the test for detection of phosphorylated Insulin like Growth Factor Binding Protein-1 was done. The test was positive if two blue lines appeared and negative if only one blue line was seen.
## IV. STATISTICAL ANALYSIS
The data collected was entered in MS excel sheet. Continuous variables were summarized as mean and were analyzed by using unpaired t test. Nominal/categorical variables were summarized as proportions and were analyzed by using chi-square/Fischer exact test. Pvalue $< 0.05$ was taken as significant. Diagnostic accuracy was assessed using following terms: Sensitivity, Specificity, PPV and NPV. Medcalc 16.4 version software was used for all statistical calculations.
## V. RESULTS
Table 1: Socio-demographic factors
<table><tr><td>Variable</td><td colspan="2">Preterm delivery</td><td>p-value</td></tr><tr><td></td><td>Yes</td><td>No</td><td></td></tr><tr><td>Age</td><td></td><td></td><td>< 0.143</td></tr><tr><td>18-25years</td><td>33(63.5%)</td><td>12(46.2%)</td><td></td></tr><tr><td>26-30years</td><td>17(32.7%)</td><td>10(38.5%)</td><td></td></tr><tr><td>>30years</td><td>2(8.8%)</td><td>4(15.4%)</td><td></td></tr><tr><td>Socio-economic status</td><td></td><td></td><td><0.223</td></tr><tr><td>Upper</td><td>6(11.5%)</td><td>2(7.7%)</td><td></td></tr><tr><td>Middle</td><td>43(82.7%)</td><td>19(73.1%)</td><td></td></tr><tr><td>Lower</td><td>3(5.8%)</td><td>5(19.2%)</td><td></td></tr><tr><td>Residence</td><td></td><td></td><td><0.150</td></tr><tr><td>Urban</td><td>29(55.8%)</td><td>10(38.5%)</td><td></td></tr><tr><td>Rural</td><td>23(44.2%)</td><td>16(61.5%)</td><td></td></tr><tr><td>BMI</td><td></td><td></td><td><0.709</td></tr><tr><td><18.5kg/m2</td><td>12(63.2%)</td><td>7(36.8%)</td><td></td></tr><tr><td>18.5-22.9kg/m2</td><td>40(67.8%)</td><td>19(32.2%)</td><td></td></tr><tr><td></td><td></td><td></td><td></td></tr></table>
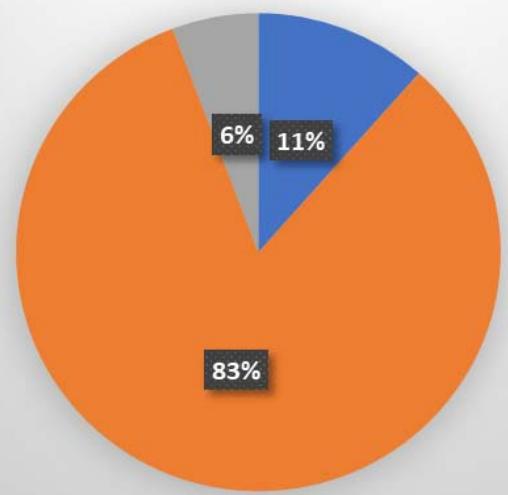
Association between Preterm delivery with socio-economic status
Upper Middle Lower
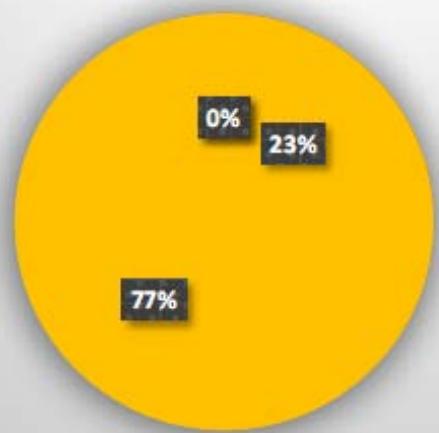
Association between preterm delivery with BMI
<18.5kg/m2 18.5-22.9kg/m2
Table 2: Risk factors for preterm delivery
<table><tr><td>Risk factor</td><td colspan="2">Preterm delivery</td></tr><tr><td></td><td>Yes</td><td>No</td></tr><tr><td>History of vaginosis (31)</td><td>24(77.4%)</td><td>7(22.6%)</td></tr><tr><td>History of threatened abortion (33)</td><td>24(72.7%)</td><td>9(27.3%)</td></tr></table>
Table 3: Complication in last delivery
<table><tr><td>Complication in last delivery</td><td colspan="2">Preterm delivery</td></tr><tr><td></td><td>Yes</td><td>No</td></tr><tr><td>Preterm delivery(58)</td><td>35(60.34%)</td><td>23(39.66%)</td></tr><tr><td>Vaginal infection (12)</td><td>9(75%)</td><td>3(25%)</td></tr><tr><td>UTI(5)</td><td>5 (100%)</td><td>0(0.00%)</td></tr></table>
Table 4: Association between preterm birth and ph-IGFBP-1 test
<table><tr><td>Preterm delivery</td><td colspan="2">PhIGFBP-1 test</td></tr><tr><td></td><td>Positive</td><td>Negative</td></tr><tr><td>Yes(52)</td><td>52 (100%)</td><td>0(0.00%)</td></tr><tr><td>No(26)</td><td>1(3.85%)</td><td>25(96.15%)</td></tr></table>
Table 5: Association between phlGF BP-1 test and test delivery interval
<table><tr><td>Test delivery interval</td><td colspan="2">PhIGFBP-1 test</td></tr><tr><td></td><td>Positive</td><td>Negative</td></tr><tr><td><=48hours(36)</td><td>36(100%)</td><td>0(0.00%)</td></tr><tr><td>48hours but within 7days (9)</td><td>9(100%)</td><td>0(0.00%)</td></tr><tr><td>>7 days (33)</td><td>8(24.24%)</td><td>25(75.76%)</td></tr></table>
## VI. RESULTS AND DISCUSSION
An accurate diagnosis of preterm labor is clinically difficult. In this study, we evaluated the value of the rapid phlGFBP-1 test in predicting preterm births in patients. In the study, majority of the participants (78) belonged to age group 18-25 years (45) and among this group, around $63.5\%$ (33) had preterm delivery. Naoko Kozuki et al(2013) $^{5}$ reported in their study that early and late maternal age is an important risk factor for preterm labor. In this study, participant distribution is equal $(50\%)$ among rural and urban areas. Various studies have given variable results on association of preterm delivery with ethnicity but data on distribution in areas are non-conclusive.
In this study, $10.3\%$ (8) women were from upper economic class, $79.5\%$ (62) from middle economic class and $10.3\%$ (8) were from lower socio-economic class. Among them maximum preterm delivery around $82.7\%$ (43) were in middle socio-economic group. This finding was not in accordance with the study done by L. Ochoe (2021)[^6] where poor or lower socio-economic status with lower education and income levels had more chances of preterm delivery.
In this study, $75.6\%$ (59) women had BMI between 18.5 -22.9 kg/m2 and among them $67.8\%$ (40) had preterm delivery. The exact mechanisms explaining the link between BMI and preterm delivery are not well known, however one theory suggests that significant preterm delivery risk increasing continuously with rising BMI.
In our study, among participants (78) around $66.7\%$ (52) delivered preterm. Among preterm delivered $77.4\%$ (24) had a history of vaginosis and $72.7\%$ (24) had a history of threatened abortion in the present pregnancy. As per Kurki et al(1992)[^7], Bacterial vaginosis had 2-6 times increased risk for preterm labor.
As per the study by Salah Roshdy (2012) $^{8}$, women with threatened abortion had a significantly increased risk of preterm labor. In our present study, those who delivered preterm, $71.4\%$ (35) had a history of previous preterm delivery, $18.4\%$ (9) had a history of vaginal infection in previous delivery and $10.2\%$ (5) had a history of UTI in previous pregnancy. As per the study by Yang (2017), a prior preterm birth increases the risk for a subsequent preterm birth with higher odds.
In our study, out of 78 women, 53 $(67.9\%)$ tested positive for phlGFBP-1 test and 25 $(32.1\%)$ tested negative result. Those who tested positive 52 $(98.1\%)$ delivered preterm and only 1 $(1.9\%)$ delivered term. Those who tested negative were not delivered preterm.
As the test has a high negative predictive value, this may enable physicians to prevent overtreatment of patients with preterm labor. Therefore, many unwanted side effects and complications of potentially hazardous tocolytic therapy can be prevented.
In our study those who tested positive $67.9\%$ (36) for phlGFBP-1(53) were maximally delivered within 48 hours and $17\%$ (9) delivered between 48 hours to 7 days and $15\%$ (8) delivered after 7 days of the test. Those who tested negative (25) were all delivered after 7 days of the test. So the test was extremely sensitive in predicting preterm labor.
## VII. LIMITATION OF THE STUDY
The sample size of study may be small for the result to be significant enough to be applicable to the general population, but it is big enough to be significant for the study population.
## VIII. CONCLUSION
In this study, results show that there is a role of cervical phlIGFBP-1 test in the management of women presenting with suspected preterm labor, it may replace cervical ultrasonography and fetal fibronectin in the future or at least serve as a useful adjunct to these tests. Thus, it will allow more focused management of women who are more likely to deliver preterm and perhaps avoid unnecessary admissions and treatment, to curtail health care costs.
Conflicts of interest: No potential conflicts of interest were reported by the authors.
Informed consent statement: All subjects here were already informed and gave consent.
Provenance and peer review: Not commissioned, externally peer-reviewed.
Declaration of competing interest: None.
### ACKNOWLEDGEMENT
The authors would like to thank everyone who supported and assisted throughout all aspects of our study and for their help in writing the manuscript.
Generating HTML Viewer...
References
8 Cites in Article
S Pallavi,Anahita Vishwekar,Najuturakhia Chauhan (2017). Unknown Title.
B Koullali,M Oudijk,T Nijman,B Mol,E Pajkrt (2016). Risk assessment and management to prevent preterm birth.
(2016). Figure 1: Conceptual causal model of preterm birth among North Dakota women who had live singleton births and did not have a prior preterm birth, 2017–2021..
Eun Jung,Jeong Park,Aeli Ryu,Sung Lee,Soo‐hyun Cho,Kyo Park (2016). Prediction of impending preterm delivery based on sonographic cervical length and different cytokine levels in cervicovaginal fluid in preterm labor.
Naoko Kozuki,C Arme,Lee (2013). The Association of parity and maternal age with small for gestational age, preterm and neonatal and infant mortality.
L ochoa-Association of neighbourhood socioeconomic trajectories with preterm birth and smallfor-gestational-age in the Netherlands: a nationwide population based study.
Dr Iqbal (1992). Bacterial Vaginosis: A Risk Factor for Preterm Labour- A Case – Control Study.
Salah Ahmed,Mohamed Alsammani,Muneera Alsheeha,Abdou Aitallah,Farhat Khan (2023). Pregnancy Outcome in Women with Threatened Miscarriage: a Year Study.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
Sana Tak. 2026. \u201cA Cross -Sectional Study on Prediction of Preterm Delivery with Phosphorylated Insulin Like Growth Factor Binding Protein -1 Test\u201d. Global Journal of Medical Research - E: Gynecology & Obstetrics GJMR-E Volume 23 (GJMR Volume 23 Issue E1): .
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.