Sudipta Chakrabarti Principal&Associate Professor in Biological Sciences
Midnapore City College
Kuturiya, Bhadutala, Paschim Medinipur-721129, West Bengal, India
Presently a day’s obesity is one of the significant public issues worldwide among kids, teenagers, just as in grown-ups and older people. From the distinctive animal models and clinical trials, it was accounted that natural adequacy related to weight is connected with more regrettable memory function. Evidence recognizes obesity as a significant danger factor for the beginning and progression of a few neurological problems associated with metabolic dysfunction and inflammation, which are related to obesity are owing to consequences for the primarily cognitive impairment. Numerous studies suggest that obesity results in neurological diseases such as Parkinson’s disease and Alzheimer’s disease, which could be initiated by various metabolic alterations, related to CNS damage as well as cognitive loss or cognitive dysfunction. This review examined whether obesity is associated with cognitive function or cognitive decline and whether obesity confounds the relationship between obesity and cognitive decline. This review approach was employed, using PubMed, and the Google Scholar database. Worse memory function may directly be related to obesity with underlying mechanisms discussed here. However, it is uncertain whether adiposity, itself, is influencing cognitive changes and it drives the obesity-cognitive relationship.
## I. INTRODUCTION
Obesity is a roaring global concern with a sprouting predominance in children (Ogden, Carroll, Kit, & Flegal, 2014), adolescents, and older people on the earth, especially in a developing country. The number of obese people also has expanded day by day in an epidemic manner throughout the last decade. It was accounted that the prevalence rate of obesity and central obesity varies from $11.8\%$ to $31.3\%$ and $16.9\% - 36.3\%$, respectively according to ICMR-INDIAB study 2015, (Ahirwar & Mondal, 2019). Obesity is characterized by the exorbitant gathering of fat, especially adipose tissues, which can adversely influence well-being by expanding the expression of pro-inflammatory markers (Huang, Zhang, & Chen, 2016). Due to the accumulation of excessive adipocytes, various health consequences such as increased heart disease, hypertension, diabetes, inactivity, inflammation, genetic alteration, stroke, and cancer (Aronne, 2001) occur. Some of these medical comorbidities are associated with adverse cognitive effects (Biessels, Deary, & Ryan, 2008). There is a strong correlation between obesity and neurodegenerative diseases, suggesting that obesity might affect the central nervous system, causing neurodegeneration and cognitive decline, as well as causing brain damage (Ashrafian, Harling, Darzi, & Athanasiou, 2013). Neurodegenerative disease (ND) is a significant reason for inability, morbidity, and diminished personal satisfaction, establishing the basis for $12\%$ of human death internationally (Erkkinen, Kim, & Geschwind, 2018). Investigations have shown that individuals who experience the ill effects of midlife obesity (estimated by BMI) have an expanded danger to building Alzheimer's Disease (AD) and Parkinson's Disease (PD) (Profenno, Porsteinsson, & Faraone, 2010). The role of obesity in memory and cognitive decline has been reviewed in this article.
## II. EFFECT OF OBESITY ON BRAIN STRUCTURE AND COGNITIVE CAPACITY
### a) Brain Structure
Structure alteration in neural architecture due to obesity has been recently reported. For instance, raised BMI is connected to diminished cerebrum volume (Ward, Carlsson, Trivedi, Sager, & Johnson, 2005), the autonomy of age, and morbidity (Gunstad et al., 2008). Expanded BMI is connected with gray matter decay in some specific parts of the brain (Shefer, Marcus, & Stern, 2013), and decreased uprightness of white matter of the brain (Verstynen et al., 2012). Middle-age must be the most critical period for brain aging and at that time, vulnerability to obesity is particularly acute compared with later life (Ronan et al., 2016), and the starting of middle-age, there has been identified white matter atrophy (Fotenos, Snyder, Girton, Morris, & Buckner, 2005) in the brain. Recently, Thompson et al. (2020) conducted a meta-analysis where the connection between obesity $(\mathrm{BMI} > 30\mathrm{kg} / \mathrm{m}^2)$ and brain structure of 6420 members was studied. Obesity has been shown to be associated with brain structure abnormalities, including a lowered temporal-frontal thickness. Cortical thinning of the brain might be related to decreased microstructural integrity in white matter tracts in obese teenagers (Yau et al., 2014). Further, obesity decreases practical movement in cortical regions that are associated with episodic memory (hippocampus, dorsolateral prefrontal cortex, and angular gyrus) (Cheke, Bonnici, Clayton, & Simons, 2017). Obesity also causes an increase in the amount of glycerol, hormones, cytokines, and pro-inflammatory substances involved in developing insulin resistance (Al-Goblan, Al-Alfi, & Khan, 2014). The hippocampus might be especially helpless against the adverse consequences of abnormal glucose tolerance and insulin resistance comparative with other cerebrum districts, a suggestion supported by neurological, structural research associating type 2 diabetes and impaired glucose tolerance (IGT) with hippocampal atrophy (Bruehl et al., 2009; Gold & Shadlen, 2007; Korf, White, Scheltens, & Launer, 2006). Expanded development of harmful glycation end product results in hyperglycemia and type 2 diabetes (Roriz-Filho et al., 2009), this could result in hippocampal volume loss, especially given that the hippocampus is profoundly defenseless against other metabolic affronts (McEwen, 1997; Stranahan et al., 2008). Hippocampus has a high co-restriction of insulin and cortisol receptors (Jacobson & Sapolsky, 1991). It has been guessed that persistently raised corticosteroids related to type 2 diabetes could modify synaptic plasticity and explicit neurogenesis in the hippocampus (Magariños & McEwen, 2000). The conceivable clarification could be that peripheral insulin resistance results in expanded hepatic lipid production, especially in ceramides, a product from unsaturated fats and sphingosine and is known to have lipid solvent properties(Tong & de la Monte, 2009). A few studies have shown that ceramide promotes brain insulin resistance through an impaired brain insulin pathway (Arboleda, Morales, Benitez, & Arboleda, 2009), and results in neurodegeneration as a consequence (Arboleda et al., 2009; Sartorius et al., 2014; Tong & de la Monte, 2009). Even though there was no proof that ceramide straightforwardly results in blood-brain barrier disturbance, it is conceivable that a lot of ceramides under obese conditions might be one of the dangerous elements to cause the interruption of the blood-brain barrier. In this way, the blood-brain barrier can be crossed (Fig. 1).
### b) Cognitive and memory impairment
After different longitudinal and cross-sectional investigations, researchers considered that obesity in early adulthood or middle age could extend one's risk of later-life cognitive inability. People who had higher BMI in midlife displayed shortages in an assortment of mental spaces, including long-and short memory, psychomotor speed, verbal capacity, and spatial capacity, this led to more fast destruction of cognition (Hassing, Dahl, Pedersen, & Johansson, 2010). An increased BMI, as well as increased energy metabolites (Roriz-Filho et al., 2009), result in worse memory performance by causing hypertonicity and neuroinflammation (Gonzales et al., 2012). Numerous studies have shown that the "Western diet", which is high in saturated fats and simple sugars, impairs learning and memory in people who are obese (Beilharz,
Maniam, & Morris, 2015; Loprinzi, Frith, Edwards, Sng, & Ashpole, 2018). It is associated with decreased neurogenesis and increased inflammatory responses. As it is also shown, diet plays a vital role in such memory impairments, as opposed to being caused by adipose changes, and the brain's working memory and negative outcome learning capacity are hampered due to adaptations in the dopamine system due to obesity-induced overeating. (Coppin, Nolan-Poupart, Jones-Gotman, & Small, 2014).
BBB is mainly made up of endothelial cells. However, obesity is a cause of endothelial brokenness, adding to BBB deterioration through some mechanisms (Wardlaw et al., 2013). This results obesity-related cognitive impairments, initiates neuroinflammation and neurodegeneration. Disturbance in the tight junction of endothelium breakdown the BBB (Zlokovic, 2008) proposes that obesity might trigger tight junction interruption prompting BBB breakdown. The disruption of BBB by lipid-like substances results in microglial activation, decreased endothelial tight junction and protein articulation (Shigemoto-Mogami, Hoshikawa, & Sato, 2018; Sumi et al., 2010), ultimately leading to persistence neuroinflammation (Dalvi et al., 2017; Thaler et al., 2012) and cognitive dysfunction (Kahn & Flier, 2000). In like manner, (Bocarsly et al., 2015) announced that obesity prompted decreases in dendritic spines and led to cognitive decline. It has been shown from different findings that obesity is associated with systemic and central inflammation (Gregor & Hotamisligil, 2011; Miller & Spencer, 2014) and is always hindering memory and cognition by stimulating the production of pro-inflammatory cytokines and adipokines that lead to insulin resistance (Su et al., 2017). De Souza and partners found that high-fat diets or obesity raises the pro-inflammatory cytokines and the pro-inflammatory transcription factor NF $\beta$ B in the hypothalamus (De Souza et al., 2005). The hippocampus, a significant area in cognitive preparing, learning, and memory, might be especially defenseless against inflammation in obesity, with raised TNF- $\alpha$ and ionized calcium-binding connector particle 1 (Iba1; microglial marker) (Jeon et al., 2012). Hence, this concluded that systemic inflammation and obesity have been recognized as the leading cause of cerebral white matter injuries and cognitive brokenness (T Den Heijer et al., 2005; Viscogliosi, Donfrancesco, Palmieri, & Giampaoli, 2017). In addition, higher plasma levels of interleukin (IL)-12 and 6 are connected to diminished speed in handling data and a quicker pace of cognitive decay (Marioni et al., 2010; Schram et al., 2007; Trollor et al., 2012). Hypertension expands one's danger of being diagnosed to have mild cognitive impairment (MCI) (Reitz, Tang, Manly, Mayeux, & Luchsinger, 2007). It predicts the degree of weakness seen in these people (Goldstein, Levey, & Steenland, 2013). Obesity-induced hypertension in midlife is conversely identified with execution on an assortment of cognitive tests, for example, those verbal surveying memory and executive function during obesity (M. Elias, Elias, Sullivan, Wolf, & D'agostino, 2003; Launer, Masaki, Petrovitch, Foley, & Havlik, 1995). Past research has shown that mitochondria assume a crucial part in cerebrum synaptic transmission and age-related intellectual capacity (A. Cheng, Hou, & Mattson, 2010; Hara et al., 2014; Mattson, Gleichmann, & Cheng, 2008; Raefsky & Mattson, 2017). That study suggested that changes in the shape of mitochondria in presynaptic neurons affected synaptic transmission. Additionally, apoptosomes are formed that activate the caspase cascades and subsequently trigger cell death(Cain, Bratton, & Cohen, 2002). Research has shown increased level of pro-apoptotic proteins (Bax and Bad) in brain tissue from rodents with insulin resistance caused by mitochondrial impairment, along with reduced levels of anti-apoptotic proteins (Bcl-2) (Nuzzo et al., 2015; Sa-Nguanmoo et al., 2017; Sa-Nguanmoo et al., 2016). An increment in pro-apoptotic proteins can prompt cytochrome C release, bringing about cerebrum apoptosis (Gómez-Crisóstomo, López-Marure, Zapata, Zazueta, & Martínez-Abundis, 2013). Also, apoptotic-mediated neuronal passing has been known to be one fundamental component for intellectual weakness and other neurodegenerative infections and cognitive loss (Ghavami et al., 2014).
## III. OBESITY AND DEMENTIA
As populaces age, intellectual problems, including dementias, become more normal. The most common form of dementia is Alzheimer's disease (AD), representing somewhere in the range of half and $70\%$ of all dementias. Ongoing efficient reviews and metaexaminations uncover an unpredictable connection between obesity and the possibility of dementias (Anstey, Cherbuin, Budge, & Young, 2011; Beydoun et al., 2011; Gorospe & Dave, 2007). The conviction of dementia being a solitary memory-related confusion of Alzheimer's disease (AD) has tremendously congested. The present comprehension of dementia is a complete loss of memory with diminished mental and scholarly execution because of damaged synapses. The current existing research on BMI and AD is conflicting and consolidating the consequences of many investigations that exhibited a lot of conflicting data. A meta-examination done on 16 articles covering 15 planned investigations showed that underweight, overweight, and obesity in midlife is related to an expanded danger of dementia when contrasted with having normal weight or BMI. Having a raised BMI in midlife altogether expands the danger of dementia perhaps because of expanded inflammation, higher cytokine, and hormone created by fat tissues (Skoog & Gustafson, 2003). Having an expanded BMI can likewise be related to countless morbidities, for example, insulin opposition prompting diabetes, elevated cholesterol, hypertension, and cardiovascular infection (Naderali, Ratcliffe, & Dale, 2009). The vascular impacts may likewise play a part in advancing a quickly developing disease of late-life, Alzheimer's pathology. Additionally, the variables mentioned above and the higher BMI is link with the changes in cerebrum structure, white matter changes, blood-brain obstruction aggravations, and the age-related administrative changes in protein, carbohydrate, and lipid digestion that might trigger dementia pathology. The persistent overconsumption of food sources wealthy in carbohydrates and lipids in obesity can influence insulin emission and fundamentally affects cerebral glucose digestion. The normal intracellular components in type 2 Diabetes Mellitus and AD incorporate variant redox guidelines, oxidative pressure, and dynamic incendiary cycles bringing about disabled insulin emission and signaling pathways(Verdile et al., 2015). Studies have shown that central insulin organization may be powerful in helping people with Alzheimer's to perform cognitively (Claxton et al., 2015; Freiherr et al., 2013; Haj-Ali, Mohaddes, & Babri, 2009).Further evidence suggests insulin may influence AD-related proteins (e.g., APP and tau) and contribute to the progression of AD pathology and cognitive impairment (Ferreira, Clarke, Bomfim, & De Felice, 2014; Steculorum, Solas, & Brüning, 2014; Umegaki, 2014). The T2DM has a particularly damaging effect on the hippocampus - a part of the brain crucial for memory and learning functions (Bruehl et al., 2009; Tom den Heijer et al., 2003; Gold & Shadlen, 2007; Korf et al., 2006). Though diabetes is not just a danger factor for mild cognitive impairment (MCI) and Alzheimer's disorder yet in addition to some other kinds of dementia (G. Cheng, Huang, Deng, & Wang, 2012). Obesity can likewise initiate endothelial brokenness and cause cerebral hypoperfusion and improve the creation of $\beta$ -amyloid that will general, diminish endothelial capacity further, making an endless loop prompting pathogenic changes of AD. This endothelial brokenness is because of a diminished combination and activities of nitric oxide (NO) from the endothelium and expanding the development of oxidative pressure. Increasing levels of deviated dimethylarginine inhibit NO synthase activity, resulting in cerebral hypoperfusion and mental and neurodegenerative changes in AD (Toda, Ayajiki, & Okamura, 2014). In addition to the $\mathsf{A}\beta$ and Tau proteins causing AD, many factors are also a contributing factor to this disease (Alves, Correia, Miguel, Alegria, & Bugalho, 2012) including mitochondrial impairments, ROS generation, oxidative damage, proinflammatory responses, energy utilization impairments, and failure in various neurotransmission systems(Cai, Zhao, & Ratka, 2011; Ferrer et al., 2012). The gut-brain axis, also known as the gut-microbiota interaction, has also been suggested to be important in the utilization of high fat diets and other imbalanced eating plans that hinder perception (Solas, Milagro, Ramírez, & Martínez, 2017). Notably, cognitive execution and markers of cerebrum decay like whole brain and hippocampal volumes are amazing indicators of intellectual decrease and dementia in everyone (Amiya et al., 2005; M. F. Elias et al., 2000; Jack et al., 2005). In this manner, obesity-related degradation might intensify the danger for dementia and a cognitive decrease by synergistically associating with the maturing system. Predictable with this idea, higher BMI is associated with cerebrum degradation in patients determined to have AD (Abilés et al., 2010). Besides, there is proof that midlife obesity is related to an expanded pace of aggregate and hippocampal brain degradation and cognitive decrease ten years after the fact (Debette et al., 2011) and finally, cases of neurodegenerative disease. AD and PD are two main neurodegenerative diseases characterized by
the accumulation of abnormal protein in the brain, results in a neuronal loss (Gaeta & Hider, 2005) and causes cognitive impairment.
## IV. SUMMARY AND CONCLUSION
As a result of the systematic frame introduced in this review, we can now understand how obesity leads to brain changes that can result in cognitive impairment. As In addition to inflammation, hyperinsulinemia/insulin resistance, interruption of oxidative stress, and neurodegenerative diseases, obesity has been associated with cognitive impairment. It can therefore be concluded that obesity-induced structural changes in the brain, impaired mitochondrial function, insulin resistance and blood-brain barrier are major contributors to memory impairment.
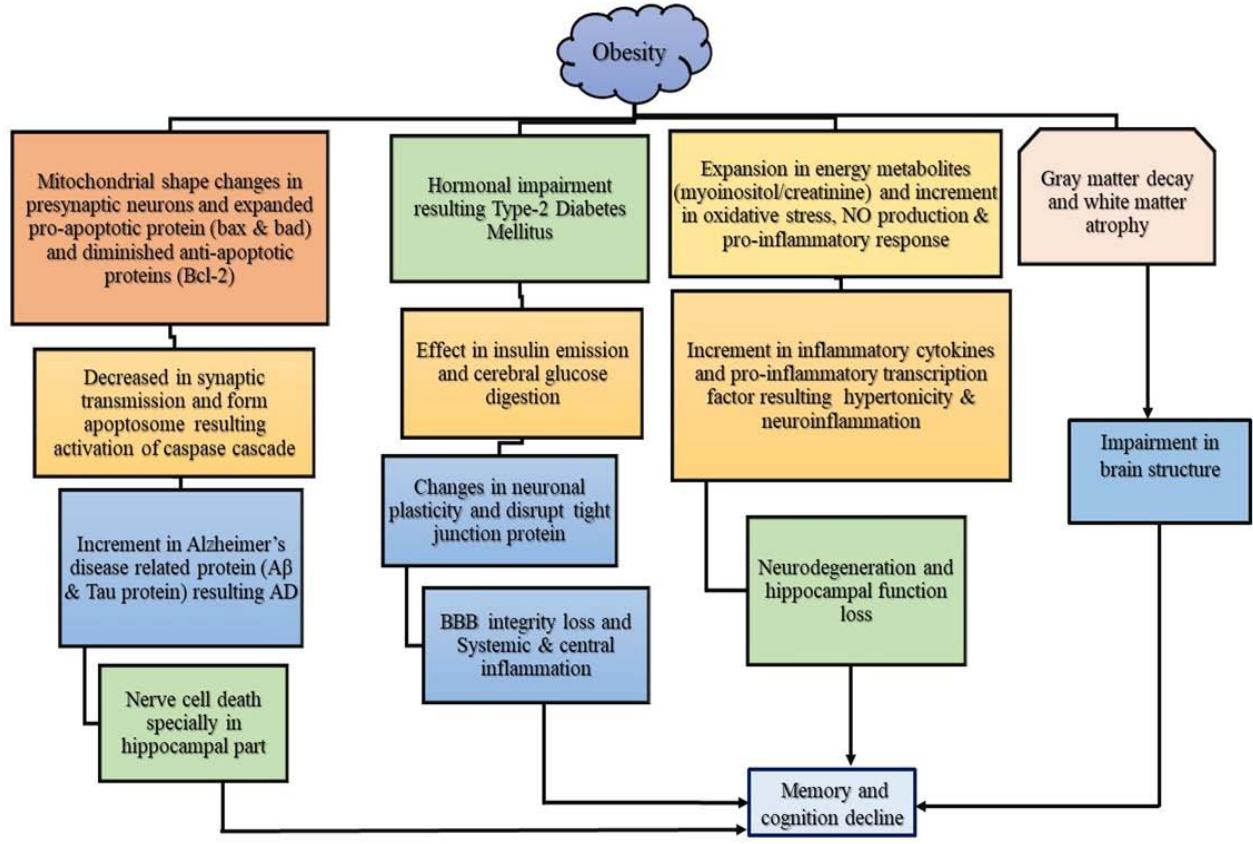 Fig.1: Systemic diagram of obesity-induced cognitive decline.
Abbreviations: AD (Alzheimer's Disease), PD (Parkinson's Disease), ND (neurodegenerative disease), BMI (basal metabolic rate), BBB (blood-brain barrier), T2DM (Type 2 diabetes mellitus), MCI (mild cognitive impairment), NF $\beta$ (nuclear factor $\beta$ ), TNF- $\alpha$ (Tumour Necrosis Factor- $\alpha$ ), IL-12 (interleukin-12), $\mathsf{A}\beta$ (amyloid $\beta$ ).
Generating HTML Viewer...
References
91 Cites in Article
V Abilés,S Rodríguez-Ruiz,J Abilés,C Mellado,A García,A Pérez De La Cruz,M Fernández-Santaella (2010). Psychological Characteristics of Morbidly Obese Candidates for Bariatric Surgery.
Rajeev Ahirwar,Prakash Mondal (2019). Prevalence of obesity in India: A systematic review.
Abdullah Algoblan,Mohammed Alalfi,Muhammad Khan (2014). Mechanism linking diabetes mellitus and obesity.
Noriko Amiya,Masafumi Amano,Akiyoshi Takahashi,Takeshi Yamanome,Hiroshi Kawauchi,Kunio Yamamori (2005). Effects of tank color on melanin-concentrating hormone levels in the brain, pituitary gland, and plasma of the barfin flounder as revealed by a newly developed time-resolved fluoroimmunoassay.
K Anstey,N Cherbuin,M Budge,J Young (2011). Body mass index in and late-life as a risk factor for dementia: a meta-analysis of prospective studies.
L Aronne (2001). Epidemiology, morbidity, and treatment of overweight and obesity.
H Ashrafian,L Harling,A Darzi,T Athanasiou (2013). Neurodegenerative disease and obesity: what is the role of weight loss and bariatric interventions?.
Jessica Beilharz,Jayanthi Maniam,Margaret Morris (2015). Diet-Induced Cognitive Deficits: The Role of Fat and Sugar, Potential Mechanisms and Nutritional Interventions.
May Beydoun,Lori Beason-Held,Melissa Kitner-Triolo,Hind Beydoun,Luigi Ferrucci,Susan Resnick,Alan Zonderman (2011). Statins and serum cholesterol's associations with incident dementia and mild cognitive impairment.
Geert Biessels,Ian Deary,Christopher Ryan (2008). Cognition and diabetes: a lifespan perspective.
Hannah Bruehl,Oliver Wolf,Victoria Sweat,Aziz Tirsi,Stephen Richardson,Antonio Convit (2009). Modifiers of cognitive function and brain structure in middle-aged and elderly individuals with type 2 diabetes mellitus.
Zhiyou Cai,Bin Zhao,Anna Ratka (2011). Oxidative Stress and β-Amyloid Protein in Alzheimer’s Disease.
K Cain,S Bratton,G Cohen (2002). The Apaf-1 apoptosome: a large caspase-activating complex.
Lucy Cheke,Heidi Bonnici,Nicola Clayton,Jon Simons (2017). Obesity and insulin resistance are associated with reduced activity in core memory regions of the brain.
A Cheng,Y Hou,M Mattson (2010). Mitochondria and neuroplasticity.
G Cheng,C Huang,H Deng,H Wang (2012). Diabetes as a risk factor for dementia and mild cognitive impairment: a meta‐analysis of longitudinal studies.
Amy Claxton,Laura Baker,Angela Hanson,Emily Trittschuh,Brenna Cholerton,Amy Morgan,Maureen Callaghan,Matthew Arbuckle,Colin Behl,Suzanne Craft (2015). Long-Acting Intranasal Insulin Detemir Improves Cognition for Adults with Mild Cognitive Impairment or Early-Stage Alzheimer's Disease Dementia.
Géraldine Coppin,Sarah Nolan-Poupart,Marilyn Jones-Gotman,Dana Small (2014). Working memory and reward association learning impairments in obesity.
P Dalvi,J Chalmers,V Luo,D.-Y Han,L Wellhauser,Y Liu,. Wheeler,M (2017). High fat induces acute and chronic inflammation in the hypothalamus: effect of high-fat diet, palmitate and TNF-α on appetite-regulating NPY neurons.
Cláudio De Souza,Eliana Araujo,Silvana Bordin,Rika Ashimine,Ricardo Zollner,Antonio Boschero,Mário Saad,Lício Velloso (2005). Consumption of a Fat-Rich Diet Activates a Proinflammatory Response and Induces Insulin Resistance in the Hypothalamus.
Den Heijer,T Launer,L Prins,N Van Dijk,E Vermeer,S Hofman,A,. Breteler,M (2005). Association between blood pressure, white matter lesions, and atrophy of the medial temporal lobe.
T Den Heijer,S Vermeer,E Van Dijk,N Prins,P Koudstaal,A Hofman,M Breteler (2003). Type 2 diabetes and atrophy of medial temporal lobe structures on brain MRI.
M Elias,P Elias,L Sullivan,P Wolf,R D'agostino (2003). Lower cognitive function in the presence of obesity and hypertension: the Framingham heart study.
M Elias,A Beiser,P Wolf,R Au,R White,R Agostino (2000). The preclinical phase of Alzheimer disease: a 22-year prospective study of the Framingham Cohort.
Michael Erkkinen,Mee-Ohk Kim,Michael Geschwind (2018). Clinical Neurology and Epidemiology of the Major Neurodegenerative Diseases.
Sergio Ferreira,Julia Clarke,Theresa Bomfim,Fernanda De Felice (2014). Inflammation, defective insulin signaling, and neuronal dysfunction in Alzheimer's disease.
I Ferrer,I López-Gonzalez,M Carmona,E Dalfó,A Pujol,A Martínez (2012). Neurochemistry and the non-motor aspects of PD.
A Fotenos,A Snyder,L Girton,J Morris,R Buckner (2005). Normative estimates of cross-sectional and longitudinal brain volume decline in aging and AD.
J Freiherr,M Hallschmid,W Frey,Y Brünner,C Chapman,C Hölscher,. Benedict,C (2013). Intranasal insulin as a treatment for Alzheimer's disease: a review of basic research and clinical evidence.
A Gaeta,R Hider (2005). The crucial role of metal ions in neurodegeneration: the basis for a promising therapeutic strategy.
Joshua Gold,Michael Shadlen (2007). The Neural Basis of Decision Making.
Felicia Goldstein,Allan Levey,N Steenland (2013). High Blood Pressure and Cognitive Decline in Mild Cognitive Impairment.
Nancy Gómez-Crisóstomo,Rebeca López-Marure,Estrella Zapata,Cecilia Zazueta,Eduardo Martínez-Abundis (2013). Bax induces cytochrome c release by multiple mechanisms in mitochondria from MCF7 cells.
Mitzi Gonzales,Takashi Tarumi,Danielle Eagan,Hirofumi Tanaka,Miral Vaghasia,Andreana Haley (2012). Indirect Effects of Elevated Body Mass Index on Memory Performance Through Altered Cerebral Metabolite Concentrations.
E Gorospe,J Dave (2007). The risk of dementia with increased body mass index.
Margaret Gregor,Gökhan Hotamisligil (2011). Inflammatory Mechanisms in Obesity.
John Gunstad,Robert Paul,Ronald Cohen,David Tate,Mary Spitznagel,Stuart Grieve,Evian Gordon (2008). Relationship Between Body Mass Index and Brain Volume in Healthy Adults.
V Haj-Ali,G Mohaddes,S Babri (2009). Intracerebroventricular insulin improves spatial learning and memory in male Wistar rats..
Yuko Hara,Frank Yuk,Rishi Puri,William Janssen,Peter Rapp,John Morrison (2014). Presynaptic mitochondrial morphology in monkey prefrontal cortex correlates with working memory and is improved with estrogen treatment.
Linda Hassing,Anna Dahl,Nancy Pedersen,Boo Johansson (2010). Overweight in Midlife Is Related to Lower Cognitive Function 30 Years Later: A Prospective Study with Longitudinal Assessments.
Wen-Juan Huang,Xia Zhang,Wei-Wei Chen (2016). Role of oxidative stress in Alzheimer's disease.
C Jack,N Arbour,J Manusow,V Montgrain,M Blain,E Mccrea,. Antel,J (2005). TLR signaling tailors innate immune responses in human microglia and astrocytes.
Lauren Jacobson,Robert Sapolsky (1991). The Role of the Hippocampus in Feedback Regulation of the Hypothalamic-Pituitary-Adrenocortical Axis*.
B Jeon,E Jeong,H Shin,Y Lee,D Lee,H Kim,. Roh,G (2012). Resveratrol attenuates obesity-associated peripheral and central inflammation and improves memory deficit in mice fed a high-fat diet.
Barbara Kahn,Jeffrey Flier (2000). Obesity and insulin resistance.
Esther Korf,Lon White,Ph Scheltens,Lenore Launer (2006). Brain Aging in Very Old Men With Type 2 Diabetes.
Lenore Launer,K Masaki,H Petrovitch,D Foley,R Havlik (1995). The Association Between Midlife Blood Pressure Levels and Late-Life Cognitive Function.
Paul Loprinzi,Emily Frith,Meghan Edwards,Eveleen Sng,Nicole Ashpole (2018). The Effects of Exercise on Memory Function Among Young to Middle-Aged Adults: Systematic Review and Recommendations for Future Research.
Ana Magariños,Bruce Mcewen (2000). Experimental diabetes in rats causes hippocampal dendritic and synaptic reorganization and increased glucocorticoid reactivity to stress.
Riccardo Marioni,Mark Strachan,Rebecca Reynolds,Gordon Lowe,Rory Mitchell,F Fowkes,Brian Frier,Amanda Lee,Isabella Butcher,Ann Rumley,Gordon Murray,Ian Deary,Jackie Price (2010). Association Between Raised Inflammatory Markers and Cognitive Decline in Elderly People With Type 2 Diabetes.
Mark Mattson,Marc Gleichmann,Aiwu Cheng (2008). Mitochondria in Neuroplasticity and Neurological Disorders.
B Mcewen (1997). Possible mechanisms for atrophy of the human hippocampus.
Alyson Miller,Sarah Spencer (2014). Obesity and neuroinflammation: A pathway to cognitive impairment.
Ebrahim Naderali,Stuart Ratcliffe,Mark Dale (2009). Review: Obesity and Alzheimer’s Disease: A Link Between Body Weight and Cognitive Function in Old Age.
D Nuzzo,P Picone,S Baldassano,L Caruana,E Messina,A Marino Gammazza,. Di Carlo,M (2015). Insulin resistance as common molecular denominator linking obesity to Alzheimer's disease.
Cynthia Ogden,Margaret Carroll,Brian Kit,Katherine Flegal (2014). Prevalence of Childhood and Adult Obesity in the United States, 2011-2012.
Louis Profenno,Anton Porsteinsson,Stephen Faraone (2010). Meta-Analysis of Alzheimer's Disease Risk with Obesity, Diabetes, and Related Disorders.
Sophia Raefsky,Mark Mattson (2017). Adaptive responses of neuronal mitochondria to bioenergetic challenges: Roles in neuroplasticity and disease resistance.
Christiane Reitz,Ming-Xin Tang,Jennifer Manly,Richard Mayeux,José Luchsinger (2007). Hypertension and the Risk of Mild Cognitive Impairment.
Lisa Ronan,Aaron Alexander-Bloch,Konrad Wagstyl,Sadaf Farooqi,Carol Brayne,Lorraine Tyler,Paul Fletcher (2016). Obesity associated with increased brain age from midlife.
Jarbas S. Roriz-Filho,Ticiana Sá-Roriz,Idiane Rosset,Ana Camozzato,Antonio Santos,Márcia Chaves,Júlio Moriguti,Matheus Roriz-Cruz (2009). (Pre)diabetes, brain aging, and cognition.
Piangkwan Sa-Nguanmoo,Pongpan Tanajak,Sasiwan Kerdphoo,Thidarat Jaiwongkam,Wasana Pratchayasakul,Nipon Chattipakorn,Siriporn Chattipakorn (2017). SGLT2-inhibitor and DPP-4 inhibitor improve brain function via attenuating mitochondrial dysfunction, insulin resistance, inflammation, and apoptosis in HFD-induced obese rats.
Piangkwan Sa-Nguanmoo,Pongpan Tanajak,Sasiwan Kerdphoo,Pattarapong Satjaritanun,Xiaojie Wang,Guang Liang,Xiaokun Li,Chao Jiang,Wasana Pratchayasakul,Nipon Chattipakorn,Siriporn Chattipakorn (2016). FGF21 improves cognition by restored synaptic plasticity, dendritic spine density, brain mitochondrial function and cell apoptosis in obese-insulin resistant male rats.
Tina Sartorius,Andreas Peter,Nadja Schulz,Andrea Drescher,Ina Bergheim,Jürgen Machann,Fritz Schick,Dorothea Siegel-Axel,Annette Schürmann,Cora Weigert,Hans-Ulrich Häring,Anita Hennige (2014). Cinnamon Extract Improves Insulin Sensitivity in the Brain and Lowers Liver Fat in Mouse Models of Obesity.
Miranda Schram,Sjoerd Euser,Anton De Craen,Jacqueline Witteman,Marijke Frölich,Albert Hofman,Jelle Jolles,Monique Breteler,Rudi Westendorp (2007). Systemic Markers of Inflammation and Cognitive Decline in Old Age.
Gabi Shefer,Yonit Marcus,Naftali Stern (2013). Is obesity a brain disease?.
Yukari Shigemoto-Mogami,Kazue Hoshikawa,Kaoru Sato (2018). Activated Microglia Disrupt the Blood-Brain Barrier and Induce Chemokines and Cytokines in a Rat in vitro Model.
Ingmar Skoog,Deborah Gustafson (2003). Hypertension, hypertension-clustering factors and Alzheimer's disease.
Maite Solas,Fermin Milagro,María Ramírez,J Martínez (2017). Inflammation and gut-brain axis link obesity to cognitive dysfunction: plausible pharmacological interventions.
S Steculorum,M Solas,J Brüning (2014). The paradox of neuronal insulin action and resistance in the development of aging-associated diseases.
Fan Su,Hao Shu,Qing Ye,Zan Wang,Chunming Xie,Baoyu Yuan,Zhijun Zhang,Feng Bai (2017). Brain insulin resistance deteriorates cognition by altering the topological features of brain networks.
Noriko Sumi,Tsuyoshi Nishioku,Fuyuko Takata,Junichi Matsumoto,Takuya Watanabe,Hideki Shuto,Atsushi Yamauchi,Shinya Dohgu,Yasufumi Kataoka (2010). Lipopolysaccharide-Activated Microglia Induce Dysfunction of the Blood–Brain Barrier in Rat Microvascular Endothelial Cells Co-Cultured with Microglia.
Joshua Thaler,Chun-Xia Yi,Ellen Schur,Stephan Guyenet,Bang Hwang,Marcelo Dietrich,Xiaolin Zhao,David Sarruf,Vitaly Izgur,Kenneth Maravilla,Hong Nguyen,Jonathan Fischer,Miles Matsen,Brent Wisse,Gregory Morton,Tamas Horvath,Denis Baskin,Matthias Tschöp,Michael Schwartz (2012). Obesity is associated with hypothalamic injury in rodents and humans.
Paul Thompson,N Jahanshad,C Ching,L Salminen,S Thomopoulos,J Bright,. Bruin,W (2020). ENIGMA and Global Neuroscience: A Decade of Large-Scale Studies of the Brain in Health and Disease Across More Than 40 Countries.
Noboru Toda,Kazuhide Ayajiki,Tomio Okamura (2014). Obesity-Induced Cerebral Hypoperfusion Derived from Endothelial Dysfunction: One of the Risk Factors for Alzheimer’s Disease.
Ming Tong,Suzanne De La Monte (2009). Mechanisms of Ceramide-Mediated Neurodegeneration.
Julian Trollor,Evelyn Smith,Emmeline Agars,Stacey Kuan,Bernhard Baune,Lesley Campbell,Katherine Samaras,John Crawford,Ora Lux,Nicole Kochan,Henry Brodaty,Perminder Sachdev (2012). The association between systemic inflammation and cognitive performance in the elderly: the Sydney Memory and Ageing Study.
H Umegaki (1011). Type 2 diabetes as a risk factor for cognitive impairment: current insights.
G Verdile,K Keane,V Cruzat,S Medic,M Sabale,J Rowles,. Newsholme,P (2015). Inflammation and oxidative stress: the molecular connectivity between insulin resistance, obesity, and Alzheimer's disease.
Timothy Verstynen,Brighid Lynch,Destiny Miller,Michelle Voss,Ruchika Prakash,Laura Chaddock,Chandramallika Basak,Amanda Szabo,Erin Olson,Thomas Wojcicki,Jason Fanning,Neha Gothe,Edward Mcauley,Arthur Kramer,Kirk Erickson (2012). Caudate Nucleus Volume Mediates the Link between Cardiorespiratory Fitness and Cognitive Flexibility in Older Adults.
Giovanni Viscogliosi,Chiara Donfrancesco,Luigi Palmieri,Simona Giampaoli (2017). The metabolic syndrome and 10-year cognitive and functional decline in very old men. A population-based study.
Michael Ward,Cynthia Carlsson,Mehul Trivedi,Mark Sager,Sterling Johnson (2005). The effect of body mass index on global brain volume in middle-aged adults: a cross sectional study.
Joanna Wardlaw,Fergus Doubal,Maria Valdes-Hernandez,Xin Wang,Francesca Chappell,Kirsten Shuler,Paul Armitage,Trevor Carpenter,Martin Dennis (2013). Blood–Brain Barrier Permeability and Long-Term Clinical and Imaging Outcomes in Cerebral Small Vessel Disease.
Suk Yau,Ang Li,Ruby Hoo,Yick Ching,Brian Christie,Tatia Lee,Aimin Xu,Kwok-Fai So (2014). Physical exercise-induced hippocampal neurogenesis and antidepressant effects are mediated by the adipocyte hormone adiponectin.
Berislav Zlokovic (2008). The Blood-Brain Barrier in Health and Chronic Neurodegenerative Disorders.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
Sudipta Chakrabarti. 2026. \u201cEffect of Obesity in Memory and Cognition\u201d. Global Journal of Medical Research - L: Nutrition GJMR-L Volume 22 (GJMR Volume 22 Issue L1).
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.