Religion, governance, and politics-as well as related topics such as human rights, justice, and so on-have historically caused many of the world’s most significant conflicts, and they continue to do so because these issues are often the most fundamental in the structure of a society. To gain a military advantage, parties to armed conflicts have polluted water, burned crops, cut down forests, poisoned soils, and killed animals over the years. A variety of context factors, particularly socioeconomic conditions, governance, and political factors, interact and play a key role in translating climate change into conflict risks. The present unrest all over the world risks putting more than half of the countries into a crisis of health, economy, and social safety, which is the biggest threat to human civilization. The security and safety of healthcare facilities, workers, and supply lines remain paramount concerns along with access to health services, technology, and innovation.
## I. INTRODUCTION
Global health has grown in popularity as a concept and academic discipline in recent years. The COVID-19 conference emphasized the world's interconnectedness and how public health threats are no longer the sole concern of single nation-states, regions, or discrete sectors. War and conflict among pandemic and climate change, have resulted in a humanitarian crisis affecting millions of people worldwide. A joint study by WHO and World Bank says that, healthcare cost pushed more than 500 million people to extreme poverty just before Covid-19 outbreak and the pandemic made the situation even worse (Figure 2)[1]. Already $25\%$ of the world population lack access to essential medicines [2] and $50\%$ of them deprived of essential health services, according to WHO (Figure 2)[3]. The planet earth is probably seeing its worst days after civilization has started as climate [4] and economic crisis [5], along with global conflicts [6]are reaching their top. When viewed from the perspective of humanity, wars and invasions are always disastrous for both combatants and war victims—specially women, the injured, children of all ages, the
elderly, the functionally disabled, and the refugees. The present study aims to bring and correlate effects of pandemic, conflict and climate issues over world economy and interconnect them with victims and future public health (Figure 1).
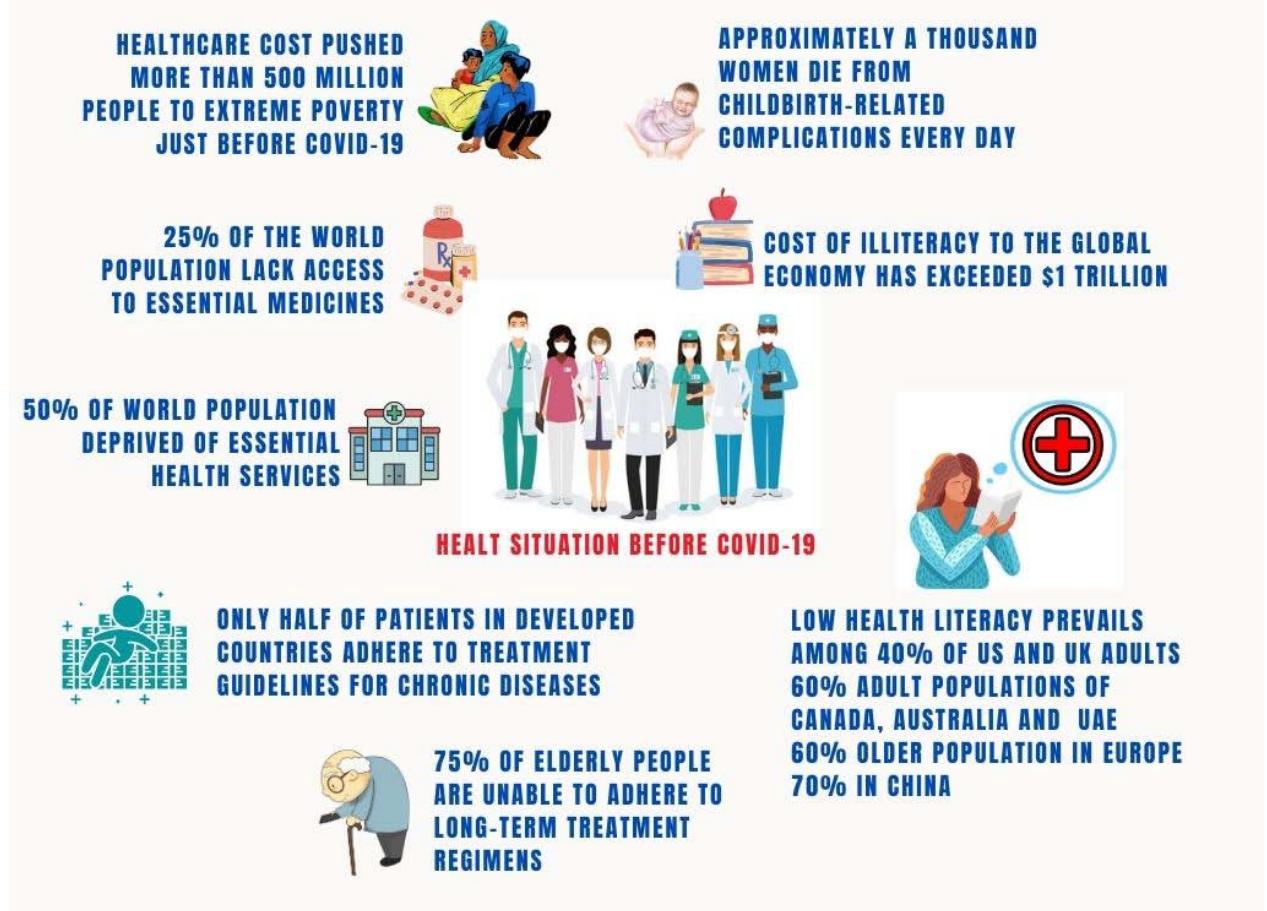 Figure 2: Even before the pandemic, the global health and economy were not in good shape.
## II. OBJECTIVE OF THE STUDY AND SOCIAL IMPLICATION
Several platforms have discussed the global health impacts of climate change, economic crisis, pandemics, and humanitarian crises, but they have been found to be inadequate because they rarely brought out the overall global situation. The current study's goal is to cover them all and bring them together on a single platform through a descriptive review. Students, journalists, healthcare providers, and even the mediocre can boost their knowledge, and of course, economists and policymakers may get a direction for future projections and strategic tools to get rid of this unique condition.
## III. METHODOLOGY
Relevant papers were extensively reviewed, mostly from online resources focusing on climate, conflict, and pandemic issues over public health. Many articles, press releases, and media broadcasts have covered the present global conflicts among pandemics and climate changes. Since journal publications lag behind many updates, popular online news platforms such as Financial Times, Washington Post, The Wall Street Journal, The Guardian, The Daily Star, BBC, CNN, CBC, New York Times, Business Standard, Bloomberg, Washington Post, Forbes and Reuters were carefully added to the keywords "global warming and public health," "war and conflicts among climate crises," and "war and conflicts among pandemics" during online search. War, conflicts, the world economy, war-weary economies with their concurrent health issues, pandemic and climate related economic losses, and changes in health system access during war and pandemic were studied. Therefore, news from online portals was carefully judged, and statistical data were correlated with journal articles, where possible. Daily reports of aggression and violence were omitted, along with complex mathematical analysis and data projections, to keep this review more understandable to common readers. Media propaganda is common
among conflict situations. Strenuous efforts have been made to correlate pandemic, climate, economic, and conflict issues with public health. PubMed, ALTAVISTA, Embase, Scopus, Web of Science, and the Cochrane Central Registers were prioritized to collect public health issues. Journals from Elsevier, Springer, Willey Online Library, and Wolters Kluwer were extensively searched.
## IV. A BRIEF REVIEW OF PRESENT GLOBAL SITUATION
### a) Climate Issues over Public Health
About 7.6 billion people—or $96\%$ of humanity have experienced a global warming effect on temperature in the past 12 months. The World Bank says, more than 1 billion people could be displaced globally by 2050 due to climate change and natural disasters (Figure 3)[7]. And more than five million extra deaths a year can be attributed to the disease burden associated with climate change, which is at least 30 times higher compared to 20 years ago (Figure 3)[8]. In those years, the lion's share (more than $96\%$ ) of disaster-related deaths had taken place mainly in developing countries[9], which has greatly shifted across 19 countries in North America, Europe, and the Asia-Pacific region that label global climate change as a major threat[10]. Global warming is influencing weather patterns, causing heat waves, heavy rainfall, droughts, cyclones, and wildfires [11]. According to the Centre for
Research on the Epidemiology of Disasters, Brussels (CRED), floods, storms, and draughts caused losses to the global economy of more than $224 billion in 2021 and could cost$ 5.6 trillion by 2050 (Figure 3) [12]. Less than $3\%$ of the earth's water is fresh water that can be used for daily necessities or agricultural use, and less than half of it can be used for drinking [13, 14]. Disastrous shrinking of rivers has been reported in the US, Europe, Asia, and the Middle East[15-18], while nearly a quarter of the world's population is at risk of flooding—10 times more rain in Sindh province [19] and 10 times faster melting of Himalayan glaciers are reported by the European Space Agency and Scientific Reports journal respectively [20]. Temperature extremes can deteriorate chronic illnesses like malnutrition [21], auto-immune diseaseslike arthritis [22] and diabetes [23], cardio-respiratory symptoms[24], certain cancer types[25, 26], as well as spread contagious diseases like mosquito-borne illnesses, COVID-19 [27], and fungal or bacterial infections[28, 29]. For instance, a 1-degree Celsius increase in global temperature may result in more than 100,000 new cases of diabetes each year in the USA alone [30] and six times more premature deaths among respiratory patients compared to the general population (Figure 3) [31]. Also, occupational heat-related mortality is 35 times higher among agricultural workers compared to workers from other industries (Figure 3) [32].
 Figure 3: The present climate issues are of great concern.
# b) The Global Economy and Public Health are Being Impacted by a Pandemic
The US government issued a new alert in May 2022 stating that the upcoming fall and winter could potentially see 100 million Covid-19 infections in the US
[33]. According to Worldometer data, during the course of the manuscript's writing, globally more than 655 million people were already affected, and 66 million had already died, as of December 14, 2022(Figure 2). As the world becomes more interconnected, the economic
The COVID-19 pandemic has been a major source of political and economic instability in many countries, with the most serious impacts of the COVID-19 pandemic become more serious. Because of its negative economic implications, the pandemic may also spark and intensify armed conflict [34-36], or at least worsen already precarious situations by escalating grievances, increasing mistrust, discrimination, and perceptions of injustice among vulnerable population in war or conflict zones [37-42]. However, fuel crisis induced by Russian aggression in Ukraine, supply chain disruptions, climate disaster, and the continued economic fallout of the COVID-19 pandemic are pushing approximately 345 million people around the globe into food insecurity [43]. "Hunger leads to one death every four seconds"—more than 200 NGOs from 75 countries were calling on global statesmen gathering at the 77th UN General Assembly to take decisive action [44]. According to the UN, a record $51.5 billion is required in 2023 to assist 230 million of the world's most vulnerable people in nearly 70 countries (Figure 4) [45]. Already, the cost of
illiteracy to the global economy has exceeded $1 trillion, and UNESCO estimates that close to 900 million learners have been affected by the closure of educational institutions, and 100 million children would fall below the minimum reading proficiency level (Figure 4) [46]. Globally, 3.3 billion people, which constitutes 81% of the world's workforce, were affected by the lockdown, and the world incurred a loss of 9% of global working hours, followed by 4.4% of the global GDP in lost labor incomes [47]. Economically and socially disadvantaged populations were twice as likely to present with COVID-19 symptoms to the emergency department and were more likely to require re-hospitalization within 30 days of discharge [48]. During the pandemic, child marriage, gender-based or domestic violence increased; routine health services were jeopardized; and routine vaccinations were halted for 80 million children in 70 countries (Figure 4) [49].
 Figure 4: The pandemic pushed the world into a deep mess.
### c) Man-Made Catastrophes
Major oil companies don't disclose the huge amount of greenhouse gases their oil fields emit--BP, Eni, ExxonMobil, Chevron, and Shell emit millions of tons of gas from their oil fields [50]. According to the World Wildlife Fund (WWF), as a result of deforestation and ocean pollution, the world's wildlife populations have decreased by more than two-thirds since 1970 [51]. Man-made catastrophes like mountain destruction, deforestation, and pollution not only hamper food, fuel, and habitat but also cause the spread of acute infections [52, 53], chronic conditions [54] and communicable diseases [55]. For example, cardiovascular disease accounts for more than $60\%$ of pollution-related disease and death [56]; each kilometer square of Brazilian Amazon deforestation results in 27 new malaria cases [57]. This is particularly important as, from California to Germany and China, droughts have shrunk the rivers that drive huge hydroelectric plants [58]. As global energy supplies tightened last year, India [59], China [60], Australia [61], and many European Union countries [62] increased their reliance on coal-fired power—along with the Russia-Ukraine conflict (Figure 4). The world's consumption of coal is taking it back to the record level it reached nearly a decade ago, says an International Energy Agency press release [63]. In its recent publication, Nature Food journal is saying "We estimate more than 2 billion people could die from nuclear war between India and Pakistan, and more than 5 billion could die from a war between the United States and Russia—underlining the importance of global cooperation in preventing nuclear war" [6].
### d) Present Global Economic Crisis: Fact is Stranger Than Fiction
Three largest economies in the world—namely, the US, Eurozone, and China—are facing impediments due to higher than expected inflation or lockdown [64]. For example, the UK economy is being battered by rising energy costs, rising interest rates, tax increases, and Brexit [65]. Global central banks continued raising interest rates following Federal Bank of America to prevent inflation, at the fastest pace in decades but failed, so far [64-69]. Inflation hits 40 years high in the US, UK [70-72], Japan [73], Germany [74]; 37 years high in France [75] and Italy [76]; 20 years high in Russia [77] and Turkey [78], mostly due to fuel crunch, food crisis, currency devaluation and business confidence nosedive over panic. China's factory inflation hits $25\%$ in 2021 [79], economy is slowing down due to adoption of "Zero-Covid strategy" [80, 81], amid a risk of 1 million deaths in "winter wave" [82]. Eurozone inflation averaged $2.12\%$ from 1991 until 2022, climbed closed to $11\%$ in October, 2022 [83, 84]. Nearly half of the countries of the EU, $40\%$ of the countries of Africa, and $30\%$ of the countries of Asia declared bankruptcy during the previous two centuries [85, 86]. However, according to a UN official at the November 2022 climate change conference, COP27, held in Egypt, 54 countries with the poorest development are currently in danger of bankruptcy (Figure 5) [87]. Lebanon, Sri Lanka, Russia, Suriname and Zambia are already in a debt default [88]. In addition to increased employer's healthcare insurance cost [89], currency devaluation [90], a reduced labor force or lack of skilled labor [91], fuel-power crisis [92], and the transportation freight cost [93-95] has hit the supply and demand chain massively and caused trouble for manufacturers, who have undergone layoffs or delayed their economic activities to prevent more loss.
### e) Global Conflicts over Health Economics: Adding Insult to Grave Injury
Conflict was responsible for more than 10 million deaths of children under the age of five between 1995 and 2015 worldwide [96]. From 2021 to 2022, more than 100 million people will have been driven from their homes by war, violence, persecution, and human rights abuse, according to the UN refugee agency (UNHCR) [97]. Ukraine, Afghanistan, the Democratic Republic of the Congo, Ethiopia, Sudan, the Syrian Arab Republic, and Yemen are the countries with the highest numbers of internally displaced persons [96, 98]. Since 2017, more than one in every six children lived in a conflict zone around the world (were living less than 50 km from where the actual fighting took place [99, 100]); highest number of women and children living in conflict zone has been twice since 2000 [96]. Armed conflict, in its various forms and manifestations, is prevalent throughout the world and often results in forced migration, an energy crisis, capital flight, and the destruction of societies' infrastructure, which includes a lack of access to food, health care, housing, employment, clean water, and sanitation, as well as a loss of community and homes. And the resulting stress or unrest has been shown to drive violent extremism, fostering recurring cycles of conflict. Global expenditure on military weapons exceeded $500 billion in 2020 and military spending surpassed $2 trillion by now (Figure 4) [101]. After seeing 50-100 million deaths in 1918-1919 Flu pandemic and more than 34 million deaths in World War II, the incorrigible world is thirsty for another great war in the midst of Covid-19 pandemic [102-106]. Whoever wins the war, humanity loses.
#### [1] Russian Aggression against Ukraine
The present cold winter distress in Europe and the power-fuel crisis, price volatility, inflationary pressure, and recession around the globe are a consequence of this war. The GDP of Ukraine could decrease by up to 35 to $40\%$ if the war lasts longer [107]. As of August 4, 2022, more than 7 million people remain, and around 10 million refugee movements have been recorded out of Ukraine (Figure 5), making this the fastest-growing refugee crisis since World War II [108]. Over $90\%$ of the fleeing population were women and children, including unaccompanied minors. Children account for $40\%$ of the refugee population (Figure 5). Hundreds of thousands of people are still trapped and faced with a shortage of food, water, and medicines [109]. Depression, social withdrawal, and anxiety are just a few of the long-term psychological and physical health repercussions that will afflict subsequent civilizations [110]. In Ukraine, close to 3 million people with disabilities are registered, facing a greater risk of abandonment, violence, and death, while their access to safety and recovery support is limited (Figure 5) [111, 112]. The correlation between low vaccination and
Russian aggression is still a question, as Ukraine was the second lowest (15%) vaccinated country after Armenia in Europe until the end of October, 2021 [113]. With a population of 42 million people, Ukraine has reported more than 10% cases of COVID-19 and over 0.1 million deaths from March 2020 through February 2022 [114]. Among deaths from COVID-19, close to 60% were teenagers aged 10–19 years, and more than 40% were children aged 0–9 years [115]. However, the number of vaccinated people in Ukraine will not surpass 40% until June 2022. It has one of the lowest rates of vaccination among middle-income countries [116, 117]. Ukraine has among the highest global burdens of noncommunicable diseases and chronic infectious diseases, such as drug resistant tuberculosis, measles, HIV/AIDS, and hepatitis B, and C [118]. The age-adjusted death rate in Ukraine from ischemic heart disease is more than six times greater than that in European Union countries, and it has among the highest suicide rates in the world [119]. Linguistic problems during hospitalization, including lack of continuity of medical care and lack of retained medical records, have been reported among refugees in Poland, Romania,
Moldova, and Slovakia [120, 121]. Thousands of tons of sulfur dioxide and smoke poisoned the air, driving up respiratory illnesses, damaging crops, and causing four times more deaths per capita than the five cleanest countries altogether [122]. Moreover, most of the energy used for agricultural production, including fuels, electricity, fertilizers, pesticides, and lubricants, is reallocated for military use [123]. The occupiers have so far attacked more than 800 health care facilities; at least hundreds of them were completely damaged (Figure 7) [124]. At least three major oxygen plants in Ukraine have been damaged, making treatment uncertain for approximately 2,000 people requiring high oxygen flow (Figure 7) [125]. Until the 1st week of December 2022, a quarter of its population was facing power shortages and blackouts amid strong winds, rain, and sub-zero temperatures, along with half of its capital Kyiv, for days [126-128]. Europe is facing a new challenge that could lead to a new wave of COVID-19 and an increase in the number of cases of TB, polio, parasitic stomach disorders, and HIV from the Ukrainian refugees; the EU is already home to $12.5\%$ of HIV patients, according to the WHO [129, 130].
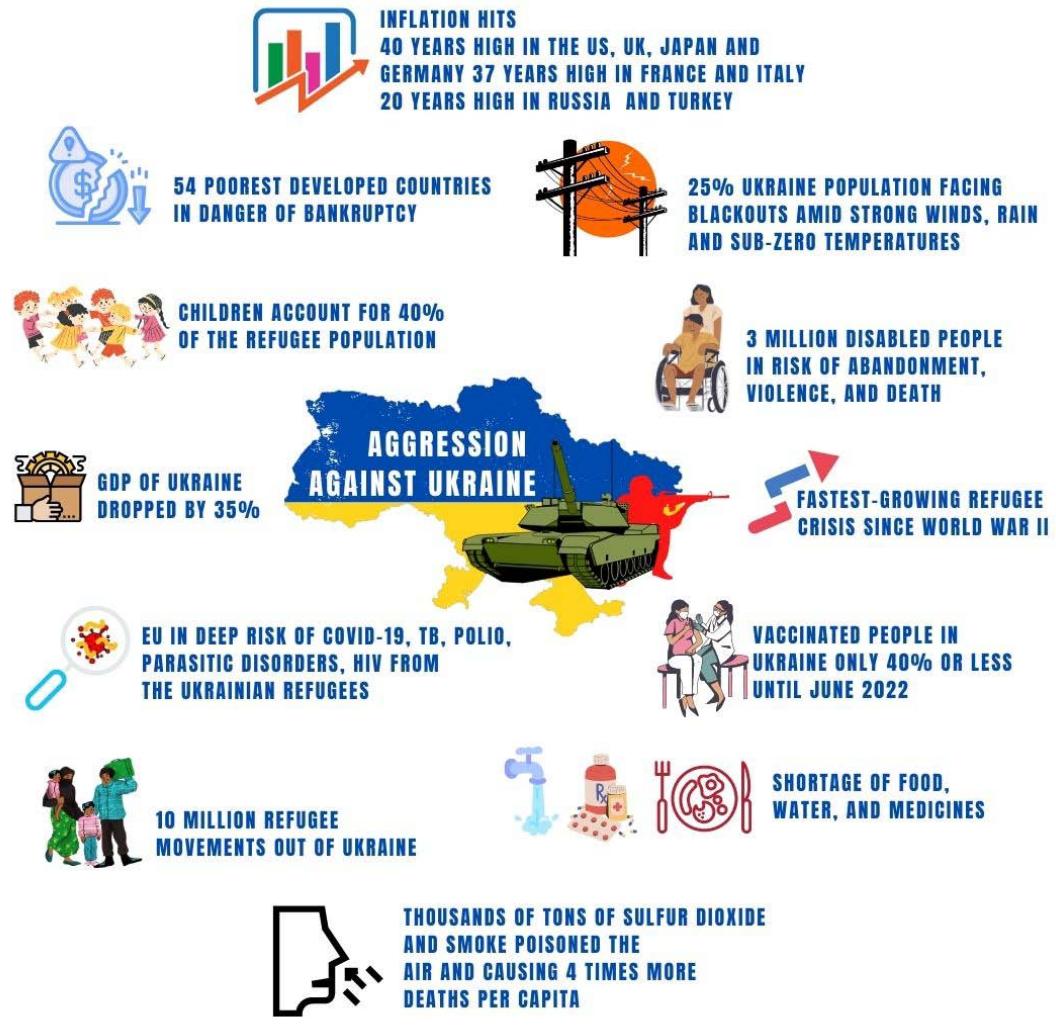 Figure 5: The Ukraine's aggression is making an impact elsewhere, too.
[2] China's Multiple Disputes including Trade War
China's growing control over one-third of the world's shipping lanes in the South China Sea poses an imminent threat to the US and Europe [131]. In the past, China has frequently been involved in border disputes with its neighbors. Southeast Asian countries such as China, Vietnam, the Philippines, Brunei, Malaysia, and Taiwan have disagreements about the disputed South China Sea [132].
U.S. goods and services trade with China will total an estimated $615.2 billion in 2020[133]. Amid an economic slowdown, China's four-year 'trade war' with the US has resulted in a total loss of USD 550 billion in import tariffs, the majority of which are aimed at Beijing [134]. China's vaccine diplomacy is believed to be based on the country's holistic approach to national security, as well as the importance China places on the "Belt and Road" Initiative [135]. China is a major manufacturer of medical products, including many vaccines, drugs, medical devices, and diagnostics. India and China are the two most important players in the global pharmaceutical raw materials and excipients market. And China accounted for \(28\%$ of the \)236.7 billion global API market in 2018 [136]. Close to $40\%$ of antibiotic APIs used in the US are sourced from China, where they are typically $35\% - 40\%$ less expensive than competitors [137].
In present years, China has increased economic, military, and political competition with the US, as depicted in numerous official documents and statements [138]. The trade war and escalating tariffs could raise manufacturing costs for generics and biosimilars in the US [139]. However, the trade war has opened up India's opportunity to export APIs. Currently, more than half of the 342 manufacturing facilities worldwide with more than ten active US-approved API products are located in India [140]. And very recently, a bill "H.R.7121(IH)-Protecting our Pharmaceutical Supply Chain from China Act of 2022" is introduced in the U.S [141].
The 2,100-mile long India-China border has long been a source of contention between New Delhi and Beijing [142]. Border tensions and the pandemic have jeopardized the supply of drugs and food between these two countries [143-145]. However, to reduce Chinese API dependency, India launched a government-backed Production Linked Incentive (PLI), as India's $42 billion pharmaceutical sector is heavily dependent on China for API [146].
A military confrontation between China and Japan has come into being for the first time since the end of World War II. After the Diaoyu Islands crises of 2010 and 2012, Japan began to regard China as a main security threat [147]. They have economic relations and cultural exchange but Japan was a pioneer in creating the concept of both the QUAD and the Indo-Pacific area [148]. The volume of trade between Japan and China
shrank in 2019 due to China-US trade frictions [149]. Japan, the largest pharmaceutical importer in the world, obtains the majority of its supplies from India, the United Kingdom, and Italy. In light of growing concerns about dependence on China around the world, the Japanese government plans to increase domestic pharmaceutical production [150].
Taiwan, missiles, and spying remain China's top priorities in the new Xi administration, as spread in many US news media [151]. Despite this, President Xi has stated that China is looking for ways to "get along" with America, even as tensions rise [152]. However, Taiwan tensions, have raised concerns about the safety of undersea cables around the world [153], as well as the semiconductor industry. In the midst of the US tech war, TSMC (the largest chip foundry with some big clients like Apple, Intel, Qualcomm, AMD, and Nvidia, based in Hsinchu Science Park, Taiwan) is under increasing threat from China [154]. Furthermore, Taiwan is home to more than $90\%$ of the world's advanced semiconductor manufacturing capacity [155]. Semiconductors are widely used in high-performance computer chips, medical equipment, drug delivery systems (implants) and in-vitro diagnostic devices, among other things [156]. Therefore, China has blocked imports of citrus, fish and other foods from Taiwan but avoided disrupting important technology and manufacturing relationships [157].
- [3] Civil unrest in Asian or Eurasian countries
- (a) The Nagorno-Karabakh conflict (Between Armenia and Azerbaijan)
Heat wave, drought, and war left Nagorno-Karabakh losing over $80\%$ of its access to water during the war last year [158]. The conflict became even more relevant for Azerbaijan in terms of its drinking water, irrigation, and hydropower. Between 20,000 and 30,000 people were killed in military operations during the Armenia-Azerbaijan clashes [159]. Ballistic missiles, drones, and other heavy artillery have been used, including the use of internationally banned cluster bombs [160]. Among the series of clashes, 50,000 people were injured or disabled, 700 medical institutions were destroyed, and the damage to the healthcare system was estimated to be $1.2 billion (Figure 7) [161]. Only $15\%$ of the Armenian population was found to be doubly vaccinated until October, 2021. They were found to have the lowest vaccination rates in the Caucasus region as the pandemic has been politicized [162]. Vaccine skepticism and being seriously hit by the COVID-19 pandemic have also been reported. Both Azerbaijan and Armenia faced a GDP shrinkage of nearly $5\%$ due to the pandemic outbreak [163, 164]. Azerbaijan's Caspian Sea, the world's largest landlocked body of water, is already rising, threatening the country's major urban centers and industrial resources along the coast [165]. With an increase in the frequency of extreme weather events, worsening desertification, and worsening land degradation, climate change is making Armenia more vulnerable. Agriculture, human health, water resources, forestry, transportation and energy infrastructure, and human health are the most at risk [166].
#### (b) Kyrgyzstan-Tajikistan border Conflicts
Kyrgyzstan-Tajikistan border tensions erupted into a brief open conflict in September 2022, and there have been more than 230 border clashes over the last 20 years between the two countries [167]. The two landlocked countries share an approximately 1,000-km long border, a third of which is disputed [168]. As a result of the COVID-19 pandemic, both of these countries have seen a precipitous drop in migrant laborer remittances from Russia [169]. Both of these countries' progress in Western-style public health education and science has been found to be slow [170].
#### (c) Sanctions and Anti-regime protests in Iran
The current anti-regime protest in Iran is a perpetuation of the previous one, sparked by the government's subsidy cut decision that caused price hikes by as much as $300\%$ for a variety of staples [171]. Almost half of Iran's 82 million population is now below the poverty line [172]. The annual rainfall is less than one-third of the global average [173], and climate changes have severe consequences for food and health [174]. Iran's economic woes have sparked several waves of protests in recent years. The UN human-rights chief has urged Iranian authorities to stop the "disproportionate use of violence" that has reportedly killed over 50 children and injured many more during Iran's public unrest [175]. Many Iranians injured by security forces during the protests are afraid to seek medical attention because some protesters seeking medical assistance have been detained. Iran has long been subject to severe international economic sanctions, which have limited their access to healthcare and are thought to be a contributing factor to their suffering [176]. Iran's ability to import drugs and medical equipment has been constrained by the majority of pharmaceutical companies being wary of getting into trouble due to US sanctions [177]. Patients with thalassemia, hemophilia, cancer, epilepsy, and multiple sclerosis who need medical care have been severely hampered by sanctions [178]. According to the 2018 statistics, among those who inject drugs in the Middle East and North Africa (MENA) region, more than $45\%$ of them were from Iran [179].
#### (d) The War-weary Afghanistan
The US Armed Forces completed their withdrawal from Afghanistan on December 31, 2021, ending 20 years of war and leaving 13 million children facing malnutrition [180] and one-third of the people food unsecured [181]. The IMF says, long-run war in Afghanistan lowered yearly national income by roughly
50% in 2016 [182]. Inflation began to rise in early 2021 as strengthening oil prices increased food transportation costs by as much as $50\%$ in some areas [181]. Since the USA's withdrawal, the World Bank, one of the project's main funders, has stopped funding the country's largest health project, which constituted nearly $80\%$ of the country's total health expenditure [183]. This has created ripple effects for the healthcare system, as hospitals operate with minimum resources [184]. The country has gone through four waves of the COVID-19, and trading economics data shows that the vaccination rate has just touched $30\%$ as of December 3, 2022 [185]. According to the WHO, deaths due to environmental risks and pollution constitute $26\%$ of overall mortality in Afghanistan. More than $30\%$ children under 5 are underweight and malnutrition reported among $60\%$ children [186]. Drug abuse prevalence is close to $13\%$ among those who are 15 years and older, and the country is known as the world's largest producer of opium, with an estimated $85\%$ share of the total global supply in 2020 [187].
#### [4] Arab and Middle East Unrest
Several Arab countries are in a humanitarian crisis as a result of armed conflict. Syria, Iraq, Lebanon, Sudan, Yemen, Libya, and the occupied Palestinian territory are among these countries [188]. Between 1970 and 2019, there were 41,837 attacks in the Middle East, making up almost $25\%$ of all terrorist attacks worldwide [189](Figure 6). Since the beginning of 2022, thousands of children have been killed in conflict or violence in several Middle Eastern and North African countries [190]. Nearly 6.5 million COVID-19 cases and over 100,000 fatalities had been documented in the MENA region as of July 1, 2020. The highest number of cases have been reported in Iraq, Jordan, and the United Arab Emirates, while the highest number of fatalities have been reported in Egypt, Tunisia, Jordan, and Morocco (Figure 6) [191].
(a) The Syrian Arab Republic has remained a civil warzone for over a decade. Killing, sexual offenses, multiple healthcare crises followed by daily life struggles, a cholera outbreak among refugees, and damage to $42\%$ of hospitals are the consequences of this war [192]. Physicians for Human Rights' (PHR) June 2022 report shows that violence caused the deaths of more than $90\%$ of medical personnel in the Assad regime, and a severe fear of healthcare worker shortage occurred when $70\%$ of them fled [193, 194]. Syrian refugees have affected Jordan's economy, labor market and society through different aspects. According to Ministry of Planning and International Cooperation (MOPIC), the direct and indirect cost of hosting Syrian refugees reached approximately $8 billion [195](Figure 6)and each refugee cost the Jordan government almost $3,750 [196].
- (b) Yemen has been dealing with the worst humanitarian crisis for seven years, where more than $80\%$ of the population requires aid [197]. According to the UN report July 2022, more than four million Yemenis have been internally displaced since the crisis began, making up nearly six million people who have been forced from their homes [198]. A World Bank, UNICEF, and WHO partnership study reveals that almost $40\%$ of the population living more than two hours from comprehensive emergency obstetric and surgical care [199]. More than $50\%$ of Yemen's population had to face hunger in 2021 [200]. Around $90\%$ foods are imported and Norwegian Refugee Council reported that more than $90\%$ families have cursed COVID-19 for food and other necessity inflation [201]. Nearly $70\%$ of additional deaths between 2015 and 2019 were related to violence in armed conflict (Figure 6) [202]. Nearly 2,50,000 people have died as a direct or indirect result of the conflict during this time, including over 12,000 civilians who were killed in targeted attacks. Additionally, $60\%$ of the deceased are children under the age of five [203]. Early in 2020, the WHO reported that less than $50\%$ of Yemen's medical facilities were fully operational due to the country's ongoing civil war, which was accompanied by seasonal outbreaks of cholera, dengue fever, malaria, chikungunya, and diphtheria [204]. Around $65\%$ of diphtheria patients were under the age of 15, and nearly $50\%$ of those cases had never received the diphtheria vaccine [205].
- (c) Lebanon has been without a president for over a month [206]) and banks are remained closed for clients[207]. After decades of war, Lebanon and Israel/Occupy Palestinian Territory agreed to resolve conflicts over maritime boundary [208]. With a population estimated at around 6 million, Lebanon is home to the largest number of refugees per capita in the world. Around $30\%$ of its population is made up of Syrian refugees (Figure 6). Being hit by a long-running economic and financial crisis, a pandemic, and a Beirut food grain store blast in 2020, more than $50\%$ of the population in the country lives below the poverty line [209, 210]. According to the World Bank's recent data, Lebanon was one of the top four countries with the highest food inflation in 2012 [211]. In real terms, it had experienced $122\%$ food inflation YOY (Figure 6) [212]. As the outbreak in Syria has grown, cholera has spread to neighboring Lebanon [213].
- (d) Afro-Arab Sudan faces 'generational catastrophe'-- floods, militia raids and hunger mean a third of children are not in school at all [214]. Among the most internally displaced people on the African continent, Sudanis home to over 1.1 million
refugees, the majority of whom are fleeing South Sudan (Figure 6) [215]. The country has been in the midst of a political crisis ever since long-time leader Omar al-Bashir was overthrown there in April [216]. In addition, Sudan has endured a number of humanitarian and economic crises, including a 22-year civil war and the Darfur genocide in 2003, which caused over two million deaths, four million displacements, food shortages, and famine, and for which an estimated 7 million people urgently require life-saving assistance [217, 218]. Additionally, the COVID-19 pandemic, severe health risks, malnutrition, poor transport infrastructure and a severe lack of funding for essential services all plague South Sudan [219]. In addition, the country has less than $30\%$ healthcare access and less than $50\%$ vaccination coverage [220]. The climate crisis and displacements, malaria cases in Sudan nearly doubled between 2015 and 2019 [221]. More than $70\%$ of people use mobile phones, but the country's telemedicine coverage is still facing challenges [222].
(e) Libya has experienced decades of armed conflict and political instability. During the Gaddafi regime, oil-rich Libya enjoyed free education, electricity, and health facilities [223]. Libyan health-care infrastructure continues to deteriorate due to civil war, inadequate human and financial support, and inadequate health facilities. More than 37 attacks reported over health facilities and medical personnel after violence began in April, 2019 [224]. Libya's health system is on the verge of collapse, with three-quarters of primary health care facilities closed due to a lack of medical personnel, supplies, medication, and equipment [225]. Only $40\%$ of hospitals' inpatient beds are adequately functioning with an overall bed capacity of 15 per 10,000 [226]. According to data from Trading Economics, food inflation in Libya averaged $9.87\%$ from 2005 to 2022 and peaked at $52.64\%$ in December of 2017. Over $80\%$ of all deaths and $78\%$ of years with a disability-adjusted life expectancy in Libya are due to noncommunicable diseases, which are particularly susceptible to long-term breakdowns in health services and policymaking processes [227].

A THOUSAND AIRSTRIKES IN SYRIA AND 5,500 BOMBS DROPPED IN ARAB COUNTRIES SINCE 2017 FROM OCCUPIED PALESTINE TERRITORY

LIBYA: $80\%$ OF ALL DEATHS ARE DUE TO LONG-TERM BREAKDOWNS IN HEALTH SERVICES
VACCINATION RATE WAS BELOW 10% IN PALESTINIANS UNTIL JUNE,2021


COVID-19: HIGHEST NUMBER OF FATALITIES HAVE BEEN REPORTED IN EGYPT, TUNISIA, JORDAN, AND MOROCCO
PALESTINE: $40\%$ OF ICU PATIENTS ADMITTED DURING WAR ESCALATION HAD COVID-19 COMPLICATIONS
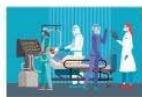

LEBANON:30% OF POPULATION IS MADE UP OF SYRIAN REFugeES

SUDAN IS HOME TO OVER 1.1 MILLION REFUGEES


JORDAN: COST OF HOSTING SYRIAN REFUGEES REACHED $8 BILLION

LEBANON EXPERIENCED $122\%$ FOOD INFLATION YOY
YEMEN: $70\%$ OF ADDITIONAL DEATHS BETWEEN 2015 AND 2019 WERE RELATEDTO VIOLENCE IN ARMED CONFLICT
NRC
NORWEGIAN REFUGEE COUNCIL: MORE THAN $90\%$ YEMENI FAMILIES HAVE CURSED COVID-19 FOR FOOD AND OTHER NECESSITY INFLATION
(f) The conflict between Palestine and its occupiers/Israel is a century-old issue. The occupiers have also experienced bereaved displacement as a result of persecution in Europe during World War II's Holocaust [228]. They have launched over a thousand airstrikes in Syria and dropped 5,500 bombs in Arab countries since 2017, facing new threats on various fronts (Figure 6) [229, 230]. It is a perfect example of “fostering recurring cycles of conflict” as depicted earlier. However, for a noble cause, two authorities signed an agreement to transfer vaccines for the COVID-19-afflicted people in June 2021, as the vaccination rate was below $10\%$ in Palestinians [231]. Afterwards, the donor withheld vaccines for the Palestinian population due to the escalation of conflicts and violence, which increased the risk of COVID-19 transmission and
damage to health facilities—including COVID-19 diagnostic testing facility. Close to $40\%$ of patients admitted in ICUs during the escalations had complications related to COVID-19 [232]. In the West Bank and Gaza Strip in 2018, there were an unprecedented 432 attacks on healthcare facilities (Figure 7) [233]. In just 13 days in May 2021 alone, the WHO reported 117 attacks on healthcare facilities in Gaza and the West Bank [234].
[5] War and Conflicts in African Countries
Deserts, grasslands, tropical forests, and semiarid lands are the four major climate zones in Africa [235]. The three most important security concerns in Africa to watch in 2022 are intra-state conflict, terrorism, and unconstitutional changes in government [236]. Droughts in Sub-Saharan Africa more than tripled between 1970 and 2009. According to the African
Development Bank, climate change is costing Africa up to $15\%$ of GDP growth [237]. Another recent study commissioned by Christian Aid claims that unless significant investments in climate adaptation are made, global warming will reduce Africa's economic growth by two-thirds by the end of the century [238]. In 2018, 2.2 million people were affected by devastating cyclones in Malawi, Mozambique, and Zimbabwe. Malaria, dengue fever, Lassa fever, Rift Valley fever, Lyme disease, Ebola virus, West Nile virus, and other infections have been linked to natural disasters [239]. Furthermore, due to the central role agriculture plays in African economies, malnutrition has increased by nearly $50\%$ since 2012 [240]. African nations, which have contributed the least to the global climate crisis, could see a $64\%$ decline in their GDP growth rate by the end of the century [241]. However, the UN and Red Cross blame the Ukraine crisis for contributing to nearly $25\%$ of Africans' food insecurity [242, 243]. Additionally, until December 2, 2022, only one-third of the population will have received at least one dose of a vaccine, making them the continent with the lowest vaccination rate [244]. The pandemic delayed the first dose of Diphtheria, Pertussis, Tetanus, Hepatitis B, and Hemophilus influenza B vaccines for 8 million African children in 2020 [245]. In addition, more than $95\%$ malaria is reported in African countries [246]. Since 1989, $75\%$ of non-state armed conflicts have been in Africa [247]. Many authors have argued climate crisis have strong association with conflicts in Africa [247-251]. Sub-Saharan Africa has the highest number of conflicts in the world, with at least a thousand people killed each year on average over the last two decades [252]. Half of the Hepatitis E outbreaks in sub-Saharan Africa have occurred among refugees and displaced persons living in humanitarian crisis settings [253].
#### (a) Ethiopia's Tigray conflict
Ethiopia, a landlocked country in the Horn of Africa, is a federal democratic republic. In Ethiopia, the pooled level of poor COVID-19 prevention practice was $51.60\%$. Inadequate COVID-19 knowledge, a negative attitude toward COVID-19 management, low educational attainment, living in a rural area, and being female were all significantly associated with poor COVID-19 prevention practices [254]. Armed conflict between the Ethiopian military and the Tigrayan Defense Force (TDF) in northern Ethiopia began on November 4, 2020 [255] and has displaced over 3 million people and killed about 500,000 in the last 2 years [256]. Armed militants destroyed crops, killed people, looted and vandalized hospitals, clinics, health posts, and ambulances, as well as ransacked and destroyed schools [257]. Rape, gang rape, sexual enslavement, torture, beatings and killings of friends and family, and derogatory ethnic slurs have all been reported [255]. According to the United Nations World Food Programme (WFP), nearly half of Tigray's six
million residents are classified as "heavily food in secure," with nearly $90\%$ lacking regular access to food. According to the UN, nearly one in every three children under the age of five is malnourished [258]. Among patients with severe illness, the Covid-19-related mortality rate went up to $40.3\%$ [259]. Fistula is raging in Tigray as a result of obstructed labor, limited or absent maternal care services, under-nutrition growth, birth difficulties, trauma, and sexually transmitted diseases (STDs) caused by conflict-related sexual violence [260]. According to Médecins Sans Frontières (MSF) assessment of 106 health facilities in the Tigray region between mid-December 2020 and early March 2021, "nearly $70\%$ had been robbed, and more than $30\%$ had been disrupted; only $13\%$ were operating normally" [261]. The ongoing conflict resulted in the destruction or damage of more than 1500 health facilities in Ethiopia in 2021, according to the country's health ministry (Figure 7) [262]. However, a surprise deal has been reached in the Ethiopian civil war with both sides agreeing to halt their two-year conflict [263].
#### (b) Democratic Republic of the Congo-Rwanda Conflict
On April 23, 2022, the Ministry of Health of the Democratic Republic of the Congo announced an Ebola virus outbreak (mortality rate $30 - 90\%$ ) which was declared ended by 2016 in West Africa, claimed more than eleven thousand death [264, 265]. It witnesses $45\%$ of deaths of children fewer than 5 years old due to malnutrition [266]. According to the United Nations, the most recent fighting with Rwanda, which started in October 2022, has forced nearly 300,000 people to flee their homes [267]. Multiple occasions have seen Rwandan forces fighting alongside Congolese rebels while crossing into the Congo. The same number of individuals were displaced by ethnic conflict in the Ituri province in 2019 during a second Ebola outbreak. Six years of conflict in the DR Congo resulted in a total death toll of six million people. The majority of deaths were caused by illness and malnutrition [268].
[6] Myanmar Military Vs Arakan Army
Clashes between the Arakan army and the military junta in 2019 displaced more than $20\%$ people across the Rakhaine state, one of Myanmar's poorest [269]. However, millions of Rohingya refugees fled from Myanmar in the last 50 years, and an estimated 1.4 million refugees are seeking asylum in Bangladesh, India, Indonesia, Nepal, Thailand, and Malaysia [270-272]. Pneumonia, liver diseases, breathing difficulties [273]; diphtheria, HIV, sexually transmitted diseases, Covid-19 [274]; Hepatitis B and C [275] have so far reported among refugees. The forced migration has created anxiety, depression, emotional distress, and PTSD among more than $60\%$ of them [276]. Approximately $80\%$ of humanitarian aid providers were denied entry into refugee camps during lockdowns [277]. Also, the host country was due to receive 12
million doses in early 2021 through the COVAX initiative, but by May 2021, the country had not received a single dose [278]. According to the UN, Rohingya aid represents only half of the funds raised this year [279]. In addition to limited access to voluntary contraception, $50\%$ of refugee settlement areas lack basic skills for general sexual, reproductive, and post-rape care (including emergency contraception and safe abortions), and more than $75\%$ of births are attended by unskilled personnel [280]. Also, discrimination, violence, lack of safe drinking water, poor sanitation and health education reported in other studies. Forging national identity cards or passports through bribery or fraud, traveling abroad illegally without a passport, illegal weapons, drug trafficking, smuggling, quarrels, fights, kidnap and murders are common with them [281-283].
## V. RESULTS AND DISCUSSION
Collectively, the pandemic, climate change, rising inflation, economic stagflation, and global conflicts pushed human civilization into a unique situation that the world has never experienced before. Following other issues are taken into considerations:
### a) Poor food handling and a lack of population control threaten public health and safety
Globally, close to one-third of agricultural produce is lost annually due to insect pests, diseases, weeds, and rodents [284, 285]. The US Centers for Disease Control and Prevention (CDC) confirmed more than 11,000 food-borne infections caused by only a few types of bacteria [286]. According to the WHO, 600 million cases of foodborne diseases are recorded each year, affecting nearly $10\%$ of the world's population [287], and food safety is associated with $7.5\%$ of deaths annually [288]. Furthermore, adulterated and contaminated foods cause $60\%$ of all foodborne illnesses [289]. Food adulteration affects almost all food commodities, and the main enticing factors are high population demand and the desire for fraudulent gain [290, 291]. Only 11 years after passing seven billion, the United Nations declared that the world population had surpassed eight billion [292]. Climate change is making the Egyptian government ask parents to have fewer children [293]. Uncontrolled population growth not only creates food insecurity but also threatens health safety. High population density appears to be associated with cancers, cardiovascular and respiratory diseases [294]; a higher risk of transmission of COVID-19, especially with the Delta variant [295, 296]; poor living conditions, such as insufficient access to healthy food, drinking water, poverty-related diseases with poor healthcare access. Also, food vulnerability and price volatility are an explosive combination for certain types of conflicts [297].
### b) Malnutrition is still a world health crisis
Global acute malnutrition increased dramatically and staggeringly from $10\%$ in 2019 to $28\%$ in 2019, and household food security significantly decreased from $59\%$ in 2019 to $15\%$ (Mulugeta & Gebregziabher, 2022). According to the World Innovation Summit for Health, 2018 $60\%$ of chronically food-insecure and malnourished people globally, including $75\%$ of all children with stunted growth, live in conflict-affected countries (Figure 7) [297].
### c) Poor health literacy still prevails in wealthy and dominant countries
Unfortunately, many European citizens lack health literacy, limiting their ability to make decisions about their own, their families', and their communities' health and well-being [298]. Even low health literacy (Figure 2) is reported in nearly $40\%$ of US [299] and UK adults [300]; $60\%$ of the older population in the EU [301]; $60\%$ of the adult populations in Canada [302]; Australia [303]; the UAE [304]; and more than $70\%$ in China [305]. Despite long-term improvements in health indicators like mortality and morbidity, there are still problems with the provision of healthcare in many low- and middle-income countries. Poor health literacy is a sign that health promotion techniques are not being used properly, and it is linked to the population's deteriorating health status and low compliance with disease prevention initiatives [306, 307].
### d) "Net-Zero Carbon" delayed by decades due to 'collaboration gap'
Approximately 80% of global carbon emissions are attributed to energy, according to the International Energy Agency (IEA) [308]. Current trends in global food systems would prevent the $1.5^{\circ}\mathrm{C}$ target from being met and put the $2^{\circ}\mathrm{C}$ target by the end of the century in jeopardy, even if fossil fuel emissions stopped now [309]. According to an Oxford study, decarbonizing the energy system by 2050 could result in enormous cost savings, but it will require a massive increase in private investment in renewable energy and sustainable infrastructure around the world. Estimated annual private investment in these sectors until 2050 ranges from US $4.4 trillion to$ 9.2 trillion [310, 311]. Not surprisingly, America and China, two major polluters (40% of total CO2 emissions), were hesitant and noncommittal on the issue at COP27 [312]. The IEA estimates that global nuclear capacity will need to double by 2050 to meet net-zero targets [313], but obstacles remain. In the aftermath of the Fukushima disaster in Japan, Germany, for example, was required to close nuclear power plants by 2022 [314-316].
### e) Pandemic hits on healthcare system
The pandemic's longest and most deadly surge has posed risks to quality of care and left medical professionals exhausted. Various studies on health professionals show work-related stress, sleep
disturbances and burnouts in $60\%$ [317-319]; and hospitalization within 6 months of the pandemic starting $15\%$ [261]. Also, WHO assumes that more than 1,15,000 health professionals may have died in the period between January 2020 and May 2021, and illnesses kept at least 500,000 health workers out of the US labor force alone [320, 321]. Nearly $20\%$ of 1000 American allied health workers (nurses, assistants, etc.) who responded to the survey stated that the pandemic was one of the main reasons they quit their jobs [322]. According to a cross-sectional study conducted by the US Bureau of Labor Statistics and the University of Minnesota Data Service, pandemic-induced physician turnover was four times that of allied professionals [323]. Lack of PPE, medical supplies, and adequate compensation have been reported in several studies.
### f) Humanitarian crisis over treatment guideline adherence and drug misuse
Migration and displacement are social determinants of health problems for refugees and other migrants [324]. Health care may be low on the list of priorities for children and adolescents who face severe pressures ranging from overcrowded camps or asylums to deep anxiety about their future [325]. Humanitarian crises are associated with increased short- and long-term cardiac morbidity and mortality, as well as elevated blood pressure [326]. Hypertensive patients with diabetes mellitus were twice as likely to exhibit poor BP control, as found in war-torn Palestine [327]. Also, a US-based survey of re-settled Rohingya refugees from Myanmar shows a higher trend of chronic diseases like diabetes, hypertension, and obesity [328]. A huge increase in benzodiazepine (sedative) dispensing is reported in Canada, and abuse of similar drugs doubled in Italy among people suffering from anxiety and stress caused by COVID-19, between the years 2020 and 2021 (Figure 7) [329]. An announcement from authorities on "simple possession of cannabis" to thousands of convicted citizens prior to the US midterm elections exploded recreational drug abuse in both the US and the EU [330, 331].
### g) War and terrorism hits on healthcare system
A terrorist attack on a hospital is not uncommon. In just 2017, there were at least 188 hospitals and clinics that were destroyed or damaged. More than 60 people were kidnapped and 64 healthcare workers were killed; 203 patients died and 141 were injured. Health facilities have been forced to close in Afghanistan, Burkina Faso, the Central African Republic, Egypt, and Turkey [332]. Research finds 454 terrorist attacks against hospitals were identified in 61 different countries over a 50-year period by the Global Terrorism Database (GTD), where more than $50\%$ of the attacks took place in the Middle East, Northern Africa, and South Asia (Figure 7). And in more than $50\%$ of cases, attacks targeted medical personnel [333]. Two other
similar studies show that close to $70\%$ of those attacks involved in bomb explosion [334] and close to $60\%$ attacks taken place after 2001 [335]. Attacks on hospitals may have long-term consequences: hospital units may be unavailable for an extended period of time, and replacing staff may take several months, further complicating hospital operations. In addition, hospitals are houses of resources (drugs, toxins, radioactive elements, and biological cultures) and information that could be used for nefarious purposes, making them a tempting target for terrorist groups. A full-fledged war and siege can have devastating consequences for patients who require constant care and well-functioning health infrastructural facilities, especially in resource-limited settings where providing optimal care is already difficult [336].
### h) Global transition or a massive work-force redistribution
The pandemic has accelerated job redistribution across sectors, with an estimated $25\%$ of workers worldwide choosing or being forced to change occupations by 2030 [337]. Interestingly, the SMEs seeking to recover are now confronted with skilled labor shortages [338-340], whereas big tech giants (Apple, Alphabet, Microsoft, Netflix, Meta, Twitter, HP, Stripe) [341, 342], media giants (The Guardian, BBC, CNN, Bloomberg) [343, 344], finance giants (JPMorgan Chase, Goldman Sachs, Morgan Stanley, Citigroup, Barclays, HSBC) [345-347], retail giants (Amazon, Tesco, Walmart) [348, 349] and fashion chain giants (Gucci, Nike, H&M) [350, 351] have seen mass layoffs in recent years, mostly in 2022.
### i) Healthcare workforce shortage and transition
The redistribution of the workforce and the shortage of workers could lead to a unique situation in healthcare systems around the world. The Eurozone is dealing with severe healthcare shortages (Figure 7). There are fewer doctors in France today than there were in 2012. In Germany, there were 35,000 unfilled positions in the care industry last year, a $40\%$ increase from ten years prior. More than 700,000 people in Spain were awaiting surgery. By 2030, Finland will require 200,000 additional workers. At least $40\%$ of doctors in one-third of the Eurozone's nations were close to retirement age [352-357]. Because of the physician shortage in general practice (GP), clinical pharmacists are working in general practice across England [358, 359]. According to a recent Lancet study, the Middle East and North Africa are lacking 636,000 doctors, with South Asia having the biggest gaps [360]. Also, turnover intentions have been reported in close to $50\%$ of physicians in emergency department, resident physicians and village doctors in China [361-363]; more than $50\%$ health professionals in Ethiopia [364]; more than $55\%$ doctors in Iraq and $30\%$ doctors in South Korea [365]. Burnout among healthcare workers and
deteriorating care quality are the immediate effects [366]. Also, globally, more than $20\%$ of health professionals are located in areas where there are many care gaps and it is a major determinant of job dissatisfaction [367]. Some $30 - 60\%$ nurses leave their first job in less than a year due to work related stress, job satisfaction and better opportunities elsewhere [368, 369]. And it is estimated that the cost is four to five times higher as productivity decreases with new hires [370]. Altogether, the motivation of health workers towards their professions has declined at a time when it is already projected that the world will face an 18 million healthcare workforce shortage by 2030. And the WHO says, more than $40\%$ of them, or 7.6 million, will be nursing shortages [368]. Moreover, there is a 6.5-fold difference between high-income and low-income countries [371, 372].
### j) Fears of nuclear war or biological weapons are not entirely false
Invaders of Ukraine launched projectiles at Chernobyl nuclear facility and the active Zaporizhzhia complex, causing international concern and raising fears
of a nuclear disaster in Eastern Europe [373]. The pandemic, hunger, discrimination or racism, climate change, rising inflation or economic crisis, imperialism, political turmoil and nuclear war share a common thing—conflict. In the last 100 years, human civilization has experienced multiple acts of bioterrorism, chemical warfare, and nuclear explosions that have targeted civilians [374]; all of them were borne out of conflicts. Although, the Geneva Protocol, which was first signed in 1925 and is still in effect today, forbids the development, manufacture, and use of biological weapons in armed conflict [375]. However, already Switzerland, Sweden, Finland, Germany, US, Russia, Italy, Belgium, UK, Japan and Israel/Occupied Palestinian Territory have spent billions for nuclear shelters (Figure 7) [376-380]. And, no nuclear-armed state is currently disarming, nor engaged in nuclear disarmament negotiations [381]. Also, SARS-CoV-2 has already demonstrated its ability to start a pandemic and, in spite of efforts made around the world, it still poses a serious threat to use as a bioweapon (Figure 7) [382].

CHINA-US TRADE WAR: US IMPOSED RESTRICTION ON CHINESE DRUGS CHINA LOST HUGE PHARMA EXPORT IN JAPAN HUGE IMPACT ON SEMICONDUCTOR SUPPLY

LIBYA: $75\%$ PRIMARY HEALTH FACILITIES CLOSED DUE TO A LACK OF MEDICAL PERSONNEL, MEDICINE AND EQUIPMENT

SWITZERLAND, SWEDEN, FINLAND, GERMANY, US, RUSSIA, ITALY, BELGIUM, UK, JAPAN, ISRAEL SPENT BILLIONS FOR NUCLEAR SHELTERS

75% OF ALL CHILDREN WITH STUNTED GROWTH, LIVE IN CONFLICT-AFFECTED COUNTRIES
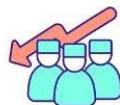
20% ARMS PURCHASE INCREASE IN EUROZONE, DESPITE HUGE HEALTHCARE SHORTAGES

UKRAINE: 3 MAJOR OXYGEN PLANT DAMAGED, TREATMENT UNCERTAIN FOR 2,000 PEOPLE
NAGORNO-KARABAKH CONFLICT: 700 MEDICAL FACILITIES WERE DESTROYED DAMAGE TO THE HEALTHCARE SYSTEM COSTS $1.2 BILLION

DESTRUCTION OR DAMAGE OF MORE THAN 1500 HEALTH FACILITIES IN ETHIOPIA IN 2021
SARS-COV-2 POSES SERIOUS THREAT TO USE AS BIOWEAPON

HIGH SEEDATIVE DISPENSING IN CANADA, DOUBLED ABUSE IN ITALY

TERRORIST ATTACKS ON HEALTHCARE FACILITIES:
AROUND 450 ATTACKS ACROSS THE WORLD IN 5 DECADES SINCE 2017
432 ATTACKS IN GAZA AND THE WEST BANK IN 2018
MORE THAN 800 ATTACKS IN UKRANE IN 2022 ALONE Figure 7: Humanitarian crisis over global health.
Present health system sustainability challenges in conflict zones and in rest of the world
1. Food crisis, malnutrition, lack of health facility access, attacks on health facility structures or medicinal personnel, harder hit by pandemics, violent extremism, violence against women and children, displacements, discriminations and many other nefarious things are common among war or conflict zone [383-386].
2. Climate-related challenges have escalated 30 times compared to 20 years ago, which will cost the global economy $224 billion in 2021 alone, accompanied by a precipitation of both chronic and contagious disease burdens. The non-cooperation of two major polluters at COP-27 may be associated with trade war-related privations, an economic crisis due to the pandemic, and fuel and power crisis. Rather, the pandemic and the fuel crisis forced major polluters to return to fossil fuel energy production.
3. Climate disasters are not under human control but are not completely beyond human reach. Much less of the money spent on war could have been spent on innovation, food, and the health system [387]. The world's medical system is still lacking [388, 389], facing newer types of diseases and challenges and will face more in coming days [390-392]. Many cancer types, HIV, autoimmune diseases, genetic disorders, antibiotic resistance—solutions of many vexing problems remain to be found.
4. Russia's invasion of Ukraine threatens to exacerbate the global inflationary surge, unbalancing oil demand and investment. The triple whammy of pandemic, fuel price shock, and currency depreciation causes economic and financial turmoil in low- and middle-income countries. Medical care and health spending generally increase faster than general inflation [393]. Also, rising inflation is associated with infant mortality rise [394]; child and maternal health compromise [395]; hospital labor expenses per patient [396]; depression, anxiety, frustration and stress [397]; cost burdens of chronic illnesses [398]; less access to assisted-living and independent-living facilities for the elderly population [399]; low-income households to compromise food quality [400]; decline insurance coverage [401]; worsening clinical labor shortage, lack of potential educators and high turnover [402]; lack of clinically necessary pharmaceuticals and supplies, as well as the accessibility of insecticides necessary to control vector-borne disease [403], are just a few examples of such problems.
5. Both conflict and climate crises cause displacements, which bring not only food and health crises but also unhealthy competition and newer
conflicts. Pandemics, climate crisis, and economic downturns pose major hit during and/or after a major conflict. Environmental pollution would not cause $26\%$ of mortality in Afghanistan if it had not been a war zone for the last 20 years. The Vietnam War lasted some 30 years and killed three million people or more [404]. Following the war, Vietnam was completely dedicated to an economic revolution and did not engage in any significant conflict. Violence was much lower after the Taliban took over, but it is now increasing as the Taliban fights two insurgencies. Azerbaijan and Armenia could resist more against a pandemic induced $5\%$ GDP drop and $1.2 billion in healthcare damage. A noticeable fact is that 700 medical institutions were destroyed at the cost of the Nagorno-Karabakh conflict, and the water crisis in Azerbaijan was a key factor, driven by the climate crisis [405,406]. Medical advances in Iran have boosted the country both domestically and internationally; the country was once known for producing $80\%$ of the world's medicinal herbs [407]. Conspicuous sanctions and spiraling unrests worsen their health situation, make life-saving drugs unavailable, and make it home to nearly half of the MENA region's injecting drug addicts.
6. $80\%$ of all humanitarian needs are also influenced by conflicts. Up to two-thirds of the world's extreme poor will reside in unstable and conflict-affected areas by 2030 [408, 409]. If the food crisis, inflation, economic stagflation prevails, healthcare will be less focused. And above all, people below the poverty line, facing any sort of discriminations or crisis can easily be engaged in crime, conflict, and chaos by shrewd opportunists. It will further decline the public health facilities. The European race to conquer Africa was fueled by commercial greed, territorial ambition, and political rivalry [228]. They encouraged Africans to fight each other in order to gain power [410, 411]. Gutierrez-Romero, 2022, stated that a $10\%$ increase in the local price index is associated with a 0.7 percentage point increase in violence against civilians in Africa. The Ukraine crisis contributes $25\%$ of their food insecurity, according to the UN and Red Cross [297]. Furthermore, Christian Aid claims severe economic stagflation will multiply conflicts in the future [238]. Their health system is also a terrible mess. They may never get rid of this position unless there is a solution to their conflict.
7. Approximately 450 terrorist attacks on healthcare facilities, mostly by bomb explosion, have been registered in more than 60 countries over the last five decades. It also raises the question of the credibility of these data, given that over 430 attacks on healthcare facilities in Palestine [233] and more
than 800 attacks on medical facilities in Ukraine have already been reported[124], [412-414]. Also, it is of great concern that victims of oppression are not even safe in hospitals, as are the caregivers and health providers.
8. For whatever reason, the total number of displaced persons exceeded 100 million, and there were 32.5 million refugees worldwide as of mid-2022, according to the UNHCR's refugee data finder. They are posing healthcare and economic burden to the already stressed host countries. Like Sub-Saharan Africa, which is facing multiple viral disease outbreaks due to the climate crisis, an intolerable food crisis partially due to the Ukraine war and triple drought, and vaccine discontinuation due to the COVID-19 outbreak, it is now hosting refugees who have become half of its Hepatitis E population. Furthermore, the EU is home to one in every eight HIV patients in the world—more than $25\%$ of Ukraine's population has been displaced and taken refuge in EU countries, where they are already among the highest rankers of HIV, drug-resistant tuberculosis, measles, and hepatitis B and C. Although close to $50\%$ of the Ukrainian war refugees had returned by June 2022 (12.6 million vs. 6 million), their vulnerabilities remained high [415, 416].
9. Transition in healthcare is not unusual; the same is happening in other sectors as well. Without sustainable economic growth, skilled workforce development is a myth. A peaceful, independent nation can take this challenge easier than a community under conflict [417-419]. In response to an expected Russian attack, the Eurozone increased its arms purchases by nearly $20\%$, despite the fact that spending on healthcare would be more necessary given the region's severe healthcare shortages, which may cause the region's health system to collapse in the near future (Figure 7) [420]. This was the case despite the fact that the global trade in major arms fell by $4.6\%$ [421].
10. It is impossible to shelter the population from biological weapons, but possible antidotes or vaccines may have been developed in secret. However, they will not be given away for free, and there will be an option to purchase them at a bargain price. Opportunistic gain is at the heart of all types of mischiefs. If that is the case, the potential for a nuclear attack becomes almost non-existent, because there will be no opportunity for dirty instincts to be satisfied if civilization does not exist. But risk arises when terrorists capture a nuclear weapon through hijacking or, in some cases, misconceptions [374], [422].
## VI. LIMITATION OF THE STUDY
Media control and propaganda always put strain over information broadcast, especially when it is related to war and conflict. Therefore, data collection from media source become a limitation for any researcher. However, the present analysis mostly uses statements from ADB, CDC (US), CRED, IMF, IEA, MOPIC, MSF, OECD, UNESCO, UNHCR, WFP, WWF, WHO, UNICEF, and World Bank, collected from their website or from the media.
## VII. CONCLUSION
War, conflicts, climate change, and pandemics are all contributing to the crisis's escalation, both directly and indirectly. The coexistence of all of these issues may endanger civilization by causing the loss of many basic healthcare facilities such as health system access, vaccination, poison control, coverage health insurance or co-payment policies, health vigilances and surveillances, monitoring of adverse drug reactions, telemedicine support, patient education or awareness programs, newer drug inventions, and allied technological advances and innovations. In a stable socio-political environment and sound economy, any of these facilities in countries or localities would take longer to develop and necessitate government and other allied authority support, IT innovation and protocol advancements, and public adherence to the health system.
### ACKNOWLEDGEMENT
I'm thankful to Dr. Mark L Graber, Professor Emeritus, Stony Brook University, and Chief Medical Officer, Founder and President Emeritus, SIDM for his valuable time to audit my paper and for his thoughtful suggestions. I'm also grateful to seminar library of Faculty of Pharmacy, University of Dhaka and BANSDOC Library, Bangladesh for providing me books, journal and newsletters.
COVAX: COVID-19 Vaccines Global Access
CNN: Cable News Network
COP27: 27th Conference of the Parties to the United Nations Framework Convention on Climate Change
CRED: Centre for Research on the Epidemiology of Disasters, Brussels
- CNBC: Consumer News and Business Channel
- EU: The European Union
- GDP: Gross Domestic Product
- GP: General Practitioner
- GTD: Global Terrorism Database
- HIV: Human Immunodeficiency Virus
- HP: Hewlett-Packard
- H&M: Hennes & Maurititz AB
- HSBC: Hongkong and Shanghai Banking Corporation
- ICU: Intensive Care Units
- IEA: International Energy Agency
- IMF: International Monetary Fund
- JPMorgan Chase: JPMorgan Chase & Co.
- MENA: Middle East and North Africa
- MSF: Médecins Sans Frontières
- MOPIC: Ministry of Planning and International Cooperation
- OECD: The Organization for Economic Co-operation and Development
- MOPIC: Physicians for Human Rights
- PLI: Production Linked Incentive
- PPE: Personal Protective Equipment
- PTSD: Post-Traumatic Stress Disorder
- QUAD: Quadrilateral Security Dialogue
- SMEs: Small and Medium-sized Enterprises
- STDs: Sexually Transmitted Diseases
- TBS: The Business Standard
- TDF: Tigrayan Defense Force
- TSMC: Taiwan Semiconductor Manufacturing Company Limited
- UAE: United Arab Emirates
- UNESCO: United Nations Educational, Scientific and Cultural Organization
- UNHCR: United Nations High Commissioner for Refugees
- UNICEF: United Nations Children's Fund
- WFP: World Food Programme
- WHO: World Health Organization
- WWF: World Wildlife Fund
- YOY: Year-over-year
- Financial Disclosure or Funding: N/A
- Conflict of Interest: The author declares that he has no competing interests.
- Declaration: The present study was conducted solely for the purpose of examining global sustainability challenges and future health system projections.
Generating HTML Viewer...
References
265 Cites in Article
R Sabet-Parry,J Guo (2021). More than half a billion people pushed or pushed further into extreme poverty due to health care costs.
Sachiko Ozawa,Raja Shankar,Christine Leopold,Samuel Orubu (2019). Access to medicines through health systems in low- and middle-income countries.
D Carrington (2022). Past five years were the hottest ever, says climate report.
K Georgieva (2022). Facing crisis upon crisis: How the world can respond.
L Xia,A Robock,K Scherrer (2022). Global food insecurity and famine from reduced crop, marine fishery and livestock production due to climate disruption from nuclear war soot injection.
J Henley (2020). Climate crisis could displace 1.2bn people by 2050.
Q Zhao,Y Guo,T Ye (2021). Global, regional, and national burden of mortality associated with nonoptimal ambient temperatures from 2000 to 2019: a three-stage modelling study.
Joses Kirigia,Luis Sambo,William Aldis,Germano Mwabu (2004). Impact of disaster-related mortality on gross domestic product in the WHO African Region.
T Smart (2022). Climate change, the environment and the cost of living top the #SetTheAgenda poll.
M Zamir (2021). Climate Change: Are we heading towards extinction? The Financial Express.
G Dickie (2022). The Summit that Snoozed? Climate-related disasters over five years have cost almost half a trillion dollars.
J Albert,G Destouni,Duke Sylvester,S (2021). Scientists' warning to humanity on the freshwater biodiversity crisis.
Joann Demaria (2022). Review: <i>A National Geographic Action Book</i>, by The National Geographic Society.
B Sullivan (2022). Hidden Waterways: Bassett Creek.
J Henley (2022). Europe's rivers run dry as scientists warn drought could be worst in 500 Years.
N Croker,R Rigdon,J Jones,C Dotto,A Dewan (2022). Seen from space: Extreme drought dries up rivers across the globe.
K Bradsher,J Dong (2022). China's record drought is drying rivers and feeding its coal habit.
Zafar Adeel (2022). Flooding in Pakistan shows that climate adaptation requires international support and regional co-operation.
Ethan Lee,Jonathan Carrivick,Duncan Quincey,Simon Cook,William James,Lee Brown (2021). Accelerated mass loss of Himalayan glaciers since the Little Ice Age.
William Dietz (2020). Climate change and malnutrition: we need to act now.
B Levine (2022). Autoimmune disease incidence increase linked to climate change.
Sarya Natur,Odeya Damri,Galila Agam (2022). The Effect of Global Warming on Complex Disorders (Mental Disorders, Primary Hypertension, and Type 2 Diabetes).
Jesse Bell,Claudia Brown,Kathryn Conlon,Stephanie Herring,Kenneth Kunkel,Jay Lawrimore,George Luber,Carl Schreck,Adam Smith,Christopher Uejio (2018). Changes in extreme events and the potential impacts on human health.
Leticia Nogueira,K Yabroff,Aaron Bernstein (2020). Climate change and cancer.
Leticia Nogueira,K Yabroff,Aaron Bernstein (2020). Climate change and cancer.
Danial Khojasteh,Ehsan Davani,Abbas Shamsipour,Milad Haghani,William Glamore (2022). Climate change and COVID-19: Interdisciplinary perspectives from two global crises.
Naomi Hauser,Kathryn Conlon,Angel Desai,Leda Kobziar (2021). Climate Change and Infections on the Move in North America.
Nnaemeka Nnadi,Dee Carter (2021). Climate change and the emergence of fungal pathogens.
Abdul Mohiuddin (2020). TRACK Implementation: a Bangladesh Scenario.
Gennaro D’amato,Carolina Vitale,Annamaria De Martino,Giovanni Viegi,Maurizia Lanza,Antonio Molino,Alessandro Sanduzzi,Alessandro Vatrella,Isabella Annesi-Maesano,Maria D’amato (2015). Effects on asthma and respiratory allergy of Climate change and air pollution.
Moussa El Khayat,Dana Halwani,Layal Hneiny,Ibrahim Alameddine,Mustapha Haidar,Rima Habib (2022). Impacts of Climate Change and Heat Stress on Farmworkers' Health: A Scoping Review.
Y Abutaleb,J Achenbach (2022). Coronavirus wave this fall could infect 100 million, Administration warns.
Marius Mehrl,Paul Thurner (2021). The Effect of the Covid-19 Pandemic on Global Armed Conflict: Early Evidence.
Emmanuel Ossai (2022). COVID-19 and Peace in Conflict-Affected Areas.
Tobias Ide (2021). COVID-19 and armed conflict.
Eyal Rubinson,Gadi Hitman (2022). The Effects of Covid-19 Emergency Aid on UN Reputation—Evidence From Syria, Yemen, and Sudan.
B Mckay,A Marcus,N Khan,J Page (2021). How this pandemic has left us less prepared for the next one.
D Crow (2020). Coronavirus fuels Black America's sense of injustice: Free to read.
Justin Chen,Emily Zhang,Cindy Liu (2020). Potential Impact of COVID-19–Related Racial Discrimination on the Health of Asian Americans.
Angela Gover,Shannon Harper,Lynn Langton (2020). Anti-Asian Hate Crime During the COVID-19 Pandemic: Exploring the Reproduction of Inequality.
Yehuda Blum (2020). 25 South Africa’s Withdrawal from the International Labour Organization (ILO).
K Georgieva,S Sosa,B Rother (2022). Global food crisis demands support for people, open trade, bigger local harvests.
Bimbisar Irom,Porismita Borah,Anastasia Vishnevskaya,Stephanie Gibbons (2022). News Framing of the Rohingya Crisis: Content Analysis of Newspaper Coverage from Four Countries.
Dan Wang,Steve Guo (2022). Making “Un-news”: News aggregation in Chinese press.
Maria Nicola,Zaid Alsafi,Catrin Sohrabi,Ahmed Kerwan,Ahmed Al-Jabir,Christos Iosifidis,Maliha Agha,Riaz Agha (2020). The socio-economic implications of the coronavirus pandemic (COVID-19): A review.
J Moyer,W Verhagen,B Mapes (2022). How many people is the COVID-19 pandemic pushing into poverty? A long-term forecast to 2050 with alternative scenarios.
Magdalena Tuczyńska,Rafał Staszewski,Maja Matthews-Kozanecka,Ewa Baum (2022). Impact of Socioeconomic Status on the Perception of Accessibility to and Quality of Healthcare Services during the COVID-19 Pandemic among Poles—Pilot Study.
Mandeep Dhaliwal,Roy Small,Douglas Webb,Lucie Cluver,Mona Ibrahim,Ludo Bok,Collin Nascimento,Cheng Wang,Aidan Garagic,Lars Jensen (2022). Covid-19 as a long multiwave event: implications for responses to safeguard younger generations.
E Stallard,O Pinnell,J Kelly (2022). Revealed: Huge gas flaring emissions never reported.
A Radchenko (2022). World Disruptive Innovations (based on Thomson Reuters Report, 2016).
Carly Reddington,Luke Conibear,Suzanne Robinson,Christoph Knote,Stephen Arnold,Dominick Spracklen (2021). Air Pollution From Forest and Vegetation Fires in Southeast Asia Disproportionately Impacts the Poor.
K Zimmer (2019). Unknown Title.
A Beyer (2022). Biden environmental push doesn't include Key Mountaintop Removal Study.
(2022). The disease of deforestation.
Thomas Münzel,Omar Hahad,Andreas Daiber,Philip Landrigan (2022). Soil and water pollution and human health: what should cardiologists worry about?.
Leonardo Chaves,Jan Conn,Rossana López,Maria Sallum (2018). Abundance of impacted forest patches less than 5 km2 is a key driver of the incidence of malaria in Amazonian Brazil.
David Campbell,Elizabeth Dale,Michael Moody (2022). Donations by top 50 US donors dropped sharply to $16 billion in 2022 – Bill Gates, Elon Musk, Mike Bloomberg and Warren Buffett lead the list of biggest givers.
S Varadhan (2022). Analysis: India Power Binges on coal, outpaces Asia. Reuters.
Y Chen (2022). Breaking views -Ukraine War helps China's coal addiction stack up.
M Mandavia (2022). Climate change could be doubleedged sword for Australian coal.
P Dvorak,A Hirtenstein (2022). 10. Gaining Green by Going Green.
(2022). OECD – Coal statistics (Edition 2021).
P-O Gourinchas (2022). IMF World Economic Outlook (WEO) Update, July 2013.
(2022). Take Steps to Identify Generational Businesses.
T Fairless (2022). Higher interest rates can take a long time to bring down inflation.
F Canepa,H Schneider (2022). Central Banks raise rates again as fed drives global inflation fight.
J Hole (2022). Central Banks will fail to tame inflation without better fiscal policy, study says.
J Smialek (2022). Articles of 2012.
A Hagstrom (2022). UK inflation matches us, soars to highest point in 40 years. Fox Business.
P Hannon (2022). inflation hits 41-year high as recession looms.
G Lopez (2022). Inflation's 40-year high.
Babagana Mala Musti (2022). The Impact of Data Frequency on the Level of Exchange Rate Pass-through to Consumer Prices in Nigeria.
M Arnold (2022). German inflation hits 40-year high as ECB president warns of 'supply shock.
M Alkhalifa (2022). Figure 1.33. Headline inflation, policy rate and real interest rate in selected Emerging Asian economies, July 2021 to January 2022.
(2022). existing-home-sales-reach-six-year-high.
L Pitel (2022). Argentine inflation hits 30-year high but may slow.
(2021). China's factory inflation hits 25-year high. The Daily Star.
S Tewari (2022). Unknown Title.
R Woo,E Zhang,L Gao (2022). China's economic wobbles worsen as factory, property woes Mount. Reuters.
E White,A Lin (2022). China risks 1mn Covid deaths in 'Winter wave', modelling shows.
M Arnold (2022). Argentine inflation hits 30-year high but may slow.
P Hannon (2022). Eurozone inflation rate rises to 10.7% as recession looms.
Megan Venzin (2022). Learn From What Went Wrong.
H Mohamed (2022). After Lebanese statement, what does state bankruptcy mean? Egypt Today.
F Harvey (2022). more than 50 poor countries in danger of bankruptcy' says UN official.
Susan Strange (2022). Debt and Default in the International Political Economy.
A Mathews (2019). Cost of employer-provided health coverage passes $20,000 a year.
D Lubin (2022). A stronger dollar might hit emerging economies harder this cycle.
C Pizzinelli,I Shibata (2022). Why jobs are plentiful while workers are scarce.
W Englund (2021). The energy crisis in the world today: analysis of the World Energy Outlook 2021.
Y Carrière-Swallow,Deb Furceri,D Jiménez,D Ostry,J (2022). How soaring shipping costs raise prices around the world.
V Golle (2021). Supply chain latest: How freight rates are adding to inflation.
R Miller,E Curran (2022). Job cuts in tech and banking don't mean mass layoffs in looming global recession.
Eran Bendavid,Ties Boerma,Nadia Akseer,Ana Langer,Espoir Malembaka,Emelda Okiro,Paul Wise,Sam Heft-Neal,Robert Black,Zulfiqar Bhutta,Zulfiqar Bhutta,Robert Black,Karl Blanchet,Ties Boerma,Michelle Gaffey,Ana Langer,Paul Spiegel,Ronald Waldman,Paul Wise (2021). The effects of armed conflict on the health of women and children.
(2022). More than 100 million now forcibly displaced: UNHCR report.
Elisabeth Mahase (2022). UN warns of “devastating” effect of covid-19, conflict, and climate change on women’s and children’s health.
N ; Rolander,S Jahan (2019). Unknown Title.
N Ferguson,S Mollman,G Rosenfeld (2022). Waheeduzzaman A. Don't let world leaders put us through World War III. The Daily Star.
V Astrov,M Ghodsi,R Grieveson (2022). Russia's invasion of Ukraine: Assessment of the humanitarian, economic, and financial impact in the short and medium term.
U Haque,A Naeem,S Wang (2022). The human toll and humanitarian crisis of the Russia-Ukraine war: the first 162 days.
B Kumar,R James,S Hargreaves (2022). Meeting the health needs of displaced people fleeing Ukraine: Drawing on existing technical guidance and evidence.
Manish Dhawan,Om Choudhary,Priyanka,Abdulrahman Saied (2022). Russo-Ukrainian war amid the COVID-19 pandemic: Global impact and containment strategy.
(2021). The Impact of the Armed Conflict and Occupation on Children’s Rights in Ukraine.
A Yakovleva,G Kovalenko,M Redlinger (2022). Tracking SARS-COV-2 variants using Nanopore sequencing in Ukraine in 2021.
I Seriakova,V Yevtushenko,S Kramarov,L Palatna,I Shpak,T Kaminska (2022). Clinical course of COVID-19 in hospitalized children of Ukraine in different pandemic periods.
O Uwishema,B Sujanamulk,M Abbass (2022). Russia-Ukraine conflict and COVID-19: a double burden for Ukraine's healthcare system and a concern for global citizens.
M Jankowski,M ; Gujski,C Greenaway,G Fabreau,K Pottie (2022). Editorial: The Public Health Implications for the Refugee Population, Particularly in Poland, Due to the War in Ukraine.
P Kardas,M Babicki,J Krawczyk,A Mastalerz-Migas (2022). War in Ukraine and the challenges it brings to the Polish healthcare system.
J Klas,A Grzywacz,K Kulszo (2022). Challenges in the Medical and Psychosocial Care of the Paediatric Refugee-A Systematic Review.
O Popov,A Iatsyshyn,V Kovach (2020). Risk Assessment for the Population of Kyiv, Ukraine as a Result of Atmospheric Air Pollution.
G Nchasi,C Mwasha,M Shaban (2022). Ukraine invasion: safe corridor for medical supplies is urgently needed, says WHO.
J Guy,Y Kesaieva,J Shelley,D Lapin,T ; Lister,S Patel,T Erickson (2022). The new humanitarian crisis in Ukraine: Coping with the public health impact of hybrid warfare, mass migration, and mental health trauma.
Lai To,L (2003). China, the USA and the South China Sea conflicts.
S Shukla (2020). What is nine-dash line? the basis of China's claim to sovereignty over South China Sea.
(2021). China's trade war with US resulted in loss of USD 550 billion: Report.
L Liu,Y Huang,Jin (2022). China's Vaccine Diplomacy and Its Implications for Global Health Governance.
C Kay,M Makol,Maz Sadek (2022). The Business Standard.
Maria Papageorgiou,Daniella De Melo (2022). China as a Responsible Power Amid the COVID-19 Crisis: Perceptions of Partners and Adversaries on Twitter.
D ; Zha,D Jimenez (2021). China and the global search for health security: history, vaccines, and governance.
V Sud,S ; Mccarthy,P Chatterjee (2020). Sharma DC. India-China border standoff raises concerns on drug supplies.
P Guerin,S Singh-Phulgenda,N Strub-Wourgaft (2020). The consequence of COVID-19 on the global supply of medical products: Why Indian generics matter for the world?.
R Buddhavarapu (2022). India wants to be the 'pharmacy of the world.
T Zhang (2021). Strengthening Crisis Management, the most urgent task in current China-US and Chinajapan security relations.
B Cannon,A ; Rossiter,Wang (2020). Locating the quad: Informality, institutional flexibility, and future alignment in the indo-pacific.
C Shepherd,P-L Wu,Taiwan (2022). Unknown Title.
D Tang (2022). Unknown Title.
P Heijmans,C Wang,S Ellis (2022). US-China confrontation over Taiwan risks escalation.
L Wintermeyer (2022). The Chip Company in Taiwan you've never heard of that powers the devices in your life -TSMC.
E Cheng,K Sutradhar,C Sumi,I Khurshudyan,E Cunningham,M Berger (2016). Implantable microchip: the futuristic controlled drug delivery system.
A Kazaryan,B Edwin,A Darzi (2021). War in the time of COVID-19: humanitarian catastrophe in Nagorno-Karabakh and Armenia.
S Shoib,N Arif,M Nahidi,K Rumiyya,S Swed,' Yusha,' Armiya (2020). Nagorno-Karabakh conflict: Mental health repercussions and challenges in Azerbaijan.
Yazdanpanah Dero,Q Yari,E Charrahy,Z (2020). Global warming, environmental security and its geoeconomic dimensions case study: Caspian Sea level changes on the balance of transit channels.
W Tompson,G Lecomte,A Pretet,L ; Mackle,G Gotsadze,N Mirzikashvili,D Kekelidze (2020). The State of Public Health Education and Science During and After the Fall of the Soviet Union: Achievements, Remaining Challenges, and Future Priorities.
A Javadi,M Ghahremanzadeh,M Sassi,O Javanbakht,B Hayati (2022). Economic evaluation of the climate changes on food security in Iran: application of CGE model.
A Mousavi,A Ardalan,A Takian,A Ostadtaghizadeh,K Naddafi,A Bavani (2020). Climate change and health in Iran: a narrative review.
K Cooper,J English (2022). UNICEF calls for the protection of children against all forms of violence in Iran amid public unrest.
F Kokabisaghi (2018). Assessment of the Effects of Economic Sanctions on Iranians' Right to Health by Using Human Rights Impact Assessment Tool: A Systematic Review.
P Bastani,Z Dehghan,S Kashfi,H Dorosti,M Mohammadpour,G Mehralian (2022). Challenge of Politico-Economic Sanctions on Pharmaceutical Procurement in Iran: A Qualitative Study.
A Asadi-Pooya,M Nazari,N Damabi (2022). Effects of the international economic sanctions on access to medicine of the Iranian people: A systematic review.
Hossein Mirzaei,Zhaleh Abdi,Elham Ahmadnezhad,Mahshad Gohrimehr,Elham Abdalmaleki,Rezvaneh Alvandi,Iraj Harirchi (2020). Health Status in the Islamic Republic of Iran, Middle East and North Africa Countries: Implications for Global Health.
M Essar,H Ashworth,A Nemat (2022). Addressing the humanitarian crisis in Afghanistan through $10 billion Afghani assets: what are the challenges and opportunities at hand?.
Z Islam,D Kokash,M Babar (2021). Food Security, Conflict, and COVID-19: Perspective from Afghanistan.
M Hameed,M Rahman,R Khanam (2022). Assessing the asymmetric war-growth nexus: A case of Afghanistan.
S Hussaini,S Ali,Syyeda Rahmat,Z Islam,Z Tharwani,Z (2022). Mental health impacts of earthquake on Afghans amidst humanitarian crisis.
G Walraven,Y Yousofzai,S Mirzazada (2021). The World Bank's health funding in Afghanistan.
A Asady,M Sediqi,S Habibi (2022). The Fourth Wave of the COVID-19 in Afghanistan: The Way Forward.
W Masood,S Aquil,H (2016). Impact of climate change on health in Afghanistan amidst a humanitarian crisis.
D Tin,S Fares,Al Mulhim,M Ciottone,G (2022). Terrorist Attacks in the Middle East: A Counter-Terrorism Medicine Analysis.
S Ahmed,Aj ; Nashwan,Janos Mhdba (2021). Public health consequences after ten years of the Syrian crisis: a literature review.
M Butt,Z Tharwani,M Muzzamil,H Rafi,H Khawaldah,N ; Alzboun,T Ahdal,R Farahat (2022). Maternal mortality and its prominence in the Syrian Arab Republic: Challenges, efforts, and recommendations.
K Garber,C Fox,M Abdalla (2020). Estimating access to health care in Yemen, a complex humanitarian emergency setting: a descriptive applied geospatial analysis.
H Hashim,A Miranda,M Babar (2021). Yemen's triple emergency: Food crisis amid a civil war and COVID-19 pandemic.
Z Rahmat,Z Islam,P Mohanan (2022). Food Insecurity during COVID-19 in Yemen.
Guha Sapir,D Ogbu,J Scales,S (2021). Civil War and death in Yemen: Analysis of Smart Survey and Acled Data, 2012-2019.
E Saleh,R Haddadin,B Saleh,E Elayeh (2022). Changes in drug demand when a pandemic coincides with other outbreaks in a war zone country: a cross-sectional pilot study.
F Dureab,M Al-Sakkaf,O Ismail (2019). Diphtheria outbreak in Yemen: the impact of conflict on a fragile health system.
K Chehayeb,A Explainer,R Jalabi (2022). Lebanon's banks to close 'indefinitely' after heists by angry depositors.
J Dahham,I Kremer,M Hiligsmann (2022). Valuation of Costs in Health Economics During Financial and Economic Crises: A Case Study from Lebanon.
M Gebeily (2022). Cholera outbreak hits Syrian refugees sheltering in camps in Lebanon. Reuters.
Z Salih (2022). UNHCR warns of surging needs in Sudan amid skyrocketing prices and gaps in humanitarian funding.
S Sirgany,N Elbagir,Y Abdullah (2019). Sudan's president Bashir forced out in military coup.
S Shoib,Osman Elmahi,O Siddiqui,M,Abdalrheem Altamih,R Swed,S,Sharif Ahmed,Em ; Lutwama,G Sartison,L Yugi,J (2022). Health services supervision in a protracted crisis: a qualitative study into supportive supervision practices in South Sudan.
V Anib,M Achiek,F Ndenzako,O Olu (2022). South Sudan's road to universal health coverage: a slow but steady journey.
A Elagali,A Ahmed,N Makki (2022). Spatiotemporal mapping of malaria incidence in Sudan using routine surveillance data.
R Elahssan,F Shariff,M Ogrady,Ti ; Yousif,Gc,A Alsadig,M Isa (2008). Telehealth application in Sudan: requirements and potential benefits.
M Elhadi,A Msherghi (2020). COVID-19 and civil war in Libya: the current situation.
L Allen,M Aghilla,M Kak (2022). Conflict as a macrodeterminant of non-communicable diseases: the experience of Libya.
Y Dahdal,N Davidovitch,M Gilmont (2021). Lessons of the Israeli-Palestinian Conflict for Public Health: The Case of the COVID-19 Vaccination Gap.
M Alkhaldi,R Coghlan,S Miller,A Basuoni,O Tanous,Y Asi (2018). Global incidence and prevalence of selected curable sexually transmitted infections: 2008.
Y Asi,O Tanous,B Wispelwey,M Alkhaldi (2021). Corrigendum to: Are there 'two sides' to attacks on healthcare? evidence from Palestine.
C Williams,N Hanan,J Neff (2007). Africa and the global carbon cycle.
S Gruzd,I Bosman,A Benkenstein,C ; Van Staden,O Pearce,M ; Andrijevic,E Anugwom,L Erhabor,G Gbakima,A (2021). Reflections on climate change and public health in Africa in an ERA of global pandemic.
A Elagali,A Ahmed,N Makki (2018). Spatiotemporal mapping of malaria incidence in Sudan using routine surveillance data.
J O'loughlin,A Linke,Fd ; Witmer,Miguel Mb,S Satyanath,J Dykema,D Lobell (2009). Effects of temperature and precipitation variability on the risk of violence in sub-Saharan Africa, 1980-2012.
F Cappelli,C Conigliani,D Consoli,V Costantini,E Paglialunga (2022). Climate change and armed conflicts in Africa: Temporal persistence, non-linear climate impact and geographical spillovers.
C Chol,J Negin,A Garcia-Basteiro (2018). Health system reforms in five sub-Saharan African countries that experienced major armed conflicts (wars) during 1990-2015: a literature review.
A Ahmed,Y Ali,E Siddig (2022). Hepatitis E Virus Outbreak among Tigray War Refugees from Ethiopia, Sudan.
M Tegegne,M Melkam,T Adane,S Getawa (2022). COVID-19 preventive practice and associated factors in Ethiopia: A systematic review and metaanalysis.
E Berhe,B Tesfay,H Teka (2022). Vicarious trauma on the hemodialysis healthcare workers in the besieged Ethiopia's Tigray region: a call to action.
S Sharif,Analysis,L Wall (2022). Ethiopia's peace may depend on post-conflict plans for Tigray soldiers.
Temesgen Abebe,H,Mitiku Ashebir,M,Mohamedniguss Ebrahim,M (2022). Epidemiological and Clinical Characteristics of COVID-19 Patients in Northern Ethiopia: A Retrospective Cohort Study.
M Gholami,I Fawad,S Shadan (2021). COVID-19 and healthcare workers: A systematic review and meta-analysis.
C Macaulay,A Soy (2019). Unknown Title.
J Sun,O Uwishema,H Kassem (2017). Human Milk output among mothers previously treated for severe acute malnutrition in childhood in Democratic Republic of Congo.
M Rashid,F Iqbal (1942). 1.2M rohingyas entered BD since.
M Ismail,M Hussain,Abdullah Al Hasan,M Kamal,A Rahman,M Hasan,M Mohiuddin,A (2020). Health problems among Forcibly Displaced Myanmar Nationals (FDMNs) admitted to the Medicine ward of Cox's Bazar Medical College Hospital.
M Ali,M Rahman,H Njuguna (2022). High Prevalence of Hepatitis B and C Virus Infections Among Rohingya Refugees in Bangladesh: A Growing Concern for the Refugees and the Host Communities.
S Palit,H Yang,J Li,Mas Khan,M Hasan (2022). The impact of the COVID-19 pandemic on the mental health of Rohingya refugees with pre-existing health problems in Bangladesh.
S Chowdhury,T Mchale,L Green,R Mishori,C Pan,I ; Fredricks,J Stoken (2020). Health professionals' perspectives on the impact of COVID-19 on sexual and genderbased violence (SGBV) and SGBV services in Rohingya refugee communities in Bangladesh.
Z Chowdhury,A ; Lion,Ak ; Mohiuddin,Salter (2014). Mini-Review on domination of pollutant residues among food products: perspective of south-East Asian countries.
H Lee,Y ; Yoon,M Baker,A-Hm Kamal (2021). Exploring customers' perceptions of food adulteration at bazaars and supermarkets in Dhaka, Bangladesh & nbsp.
A Mohiuddin (2020). Health hazards with adulterated spices: Save the "Onion Tears.
S O'grady,Hf ; Mahfouz,E Carnegie,G Inglis,A Taylor,A Bak-Klimek,O Okoye (2022). Is Population Density Associated with Non-Communicable Disease in Western Developed Countries? A Systematic Review.
Y Jamal,M Gangwar,M Usmani (2022). Identification of Thresholds on Population Density for Understanding Transmission of COVID-19.
Md Iderus,N,Lakha Singh,S,Mohd Ghazali,S (2022). Correlation between Population Density and COVID-19 Cases during the Third Wave in Malaysia: Effect of the Delta Variant.
M Gutiérrez-Romero R ; Emerson,S Buckland,M Lawlor (2015). Conflicts increased in Africa shortly after COVID-19 lockdowns, but welfare assistance reduced fatalities.
J Shebehe,S Montgomery,A Hansson,A Hiyoshi (2022). Low health literacy and multiple medications in community-dwelling older adults: a populationbased cohort study.
R Kyabaggu,D Marshall,P Ebuwei,U Ikenyei (2022). Health Literacy, Equity, and Communication in the COVID-19 Era of Misinformation: Emergence of Health Information Professionals in Infodemic Management.
C Ellender,M Boyde,I Scott (2022). Health literacy assessment in the clinic: benefits, pitfalls and practicalities.
H Ibrahim,S Nair (2021). Comment on Health Literacy: The Common Denominator of Healthcare Progress.
Y Li,X Lv,J Liang,H Dong,C Chen (2022). The development and progress of health literacy in China.
S Meherali,N Punjani,A Mevawala (2020). Health Literacy Interventions to Improve Health Outcomes in Low-and Middle-Income Countries.
T Bhardwaj (2021). Orion announces ambition to achieve net-zero carbon emissions by 2050.
C Costa,E Wollenberg,M Benitez,R Newman,N Gardner,F Bellone (2022). Roadmap for achieving netzero emissions in global food systems by 2050.
R Way,M Ives,P Mealy,J Farmer (2022). Empirically grounded technology forecasts and the Energy Transition.
N Chestney (2011). Global Nuclear Power Capacity Needs to double by 2050 -IEA. Reuters.
Antonello Russo,Maria Blettner,Hiltrud Merzenich,Daniel Wollschlaeger,Friederike Erdmann,Emilio Gianicolo (2022). Incidence of childhood leukemia before and after shut down of nuclear power plants in Germany in 2011: A population‐based register study during 2004 to 2019.
A Koontalay,W Suksatan,K Prabsangob,J Sadang (2021). Healthcare Workers' Burdens During the COVID-19 Pandemic: A Qualitative Systematic Review.
T Al-Otaibi,A Abbas,Ashry Gheith,O (2023). Determinants, predictors and negative impacts of burnout among health care workers during COVID-19 pandemic.
J Biber,B Ranes,S Lawrence (2021). Mental health impact on healthcare workers due to the COVID-19 pandemic: a U.S. cross-sectional survey study.
Y Poon,Y Lin,P Griffiths,K Yong,B Seah,S Liaw (2022). A global overview of healthcare workers' turnover intention amid COVID-19 pandemic: a systematic review with future directions.
B Frogner,J Dill (2022). Tracking Turnover Among Health Care Workers During the COVID-19 Pandemic: A Cross-sectional Study.
S Ekblad (2020). To Increase Mental Health Literacy and Human Rights Among New-Coming, Low-Educated Mothers With Experience of War: A Culturally, Tailor-Made Group Health Promotion Intervention With Participatory Methodology Addressing Indirectly the Children.
J Keasley,O Oyebode,S Shantikumar (2020). A systematic review of the burden of hypertension, access to services and patient views of hypertension in humanitarian crisis settings.
I Alawneh,A Yasin,S Musmar (2022). The Prevalence of Uncontrolled Hypertension among Patients Taking Antihypertensive Medications and the Associated Risk Factors in North Palestine: A Cross-Sectional Study.
A Rahman,J Biswas,P Banik (2022). Non-communicable diseases risk factors among the forcefully displaced Rohingya population in Bangladesh.
A Sarangi,T Mcmahon,J Gude (2021). Benzodiazepine Misuse: An Epidemic Within a Pandemic.
J Kaiman,D Smith,A Anand (2014). The Lancet. Health care in conflict: war still has rules.
N Ulmer,D Barten,De Cauwer,H (2022). Terrorist Attacks against Hospitals: World-Wide Trends and Attack Types.
B Mcneilly,G Jasani,G Cavaliere,R Alfalasi,B Lawner (2022). The Rising Threat of Terrorist Attacks Against Hospitals.
G Cavaliere,R Alfalasi,G Jasani,G Ciottone,B Lawner (2021). Terrorist Attacks Against Healthcare Facilities: A Review.
M Sekkarie,L Murad,A Al-Makki,F Al-Saghir,O Rifai,M ; Isreb,S Peters,J Dennerlein,G Wagner,G Sorensen (2020). End-Stage Kidney Disease in Areas of Armed Conflicts: Challenges and Solutions.
C Giles,R Simon (2021). Carpenter J. 4 big questions for Big Tech after its worst day for layoffs in 2022.
S Krouse,J ; Flint,J Fontanella-Khan (2020). Cost cuts loom on wall street as balance of power with staff shifts.
L Nguyen,S Azhar,N Nishant (2022). Morgan Stanley making 'modest' job cuts; CEO 'wouldn't bet against' musk.
T Francis,Emily Glazer,; Mathers,M (2022). Layoffs hit white-collar workers as Amazon, Walmart, others cut jobs.
T Taylor (2020). Nike plans layoffs in pivot to sell directly to Consumers Online.
Benjamin Ngulumbu,Fanice Waswa (2015). Abdul, G., A., & Sehar, S. (2015). Conflict management and organizational performance: A case study of Askari Bank Ltd. Research Journal of Finance and Accounting. 6(11), 201. Adhiambo, R., & Simatwa, M. (2011). Assessment of conflict management and resolution in public secondary schools in Kenya: A case study of Nyakach District. International Research Journal 2(4), 1074-1088. Adomi, E., & Anie, S. (2015). Conflict management in Nigerian University Libraries. Journal of Library Management, 27(8), 520-530. https://doi.org/10.1108/01435120610686098 Amadi, E., C., & Urho, P. (2016). Strike actions and its effect on educational management in universities in River State. Kuwait Chapter of Arabian Journal of Business and Management Review, 5(6), 41-46. https://doi.org/10.12816/0019033 Amah, E., & Ahiauzu, A. (2013). Employee involvement and organizational effectiveness. Journal of Management Development, 32(7), 661-674. https://doi.org/10.1108/JMD-09-2010-0064 Amegee, P. K. (2010). The causes and impact of labour unrest on some selected organizations in Accra. University of Ghana Awan, A., G., & Anjum K. (2015). Cost of High Employees turnover Rate in Oil industry of Pakistan, Information and Knowledge Management, 5 (2), 92- 102. Bernards, N. (2017). The International Labour Organization and African trade unions: tripartite fantasies and enduring struggles. Review of African Political Economy, 44(153), 399-414. https://doi.org/10.1080/03056244.2017.1318359 Blomgren Amsler, L., Avtgis, A. B., & Jackman, M. S. (2017). Dispute System Design and Bias in Dispute Resolution. SMUL Rev., 70, 913. Boheim, R., & Booth, A. (2004). Trade union presence and employer provided training in Great Britain industrial relations 43: pp 520-545. https://doi.org/10.1111/j.0019-8676.2004.00348.x Bryson, A., & Freeman, R. B. (2013). Employee perceptions of working conditions and the desire for worker representation in Britain and the US. Journal of Labor Res 34(1), 1–29. https://doi.org/10.1007/s12122-012-9152-y Buccella, D., & Fanti, L. (2020). Do labour union recognition and bargaining deter entry in a network industry? A sequential game model. Utilities Policy, 64, 101025. https://doi.org/10.1016/j.jup.2020.101025 Constitution, K. (2010). Government printer. Kenya: Nairobi. Cortés, P. (Ed.). (2016). The new regulatory framework for consumer dispute resolution. Oxford University Press. https://doi.org/10.1093/acprof:oso/9780198766353.001.0001 Creighton, B., Denvir, C., & McCrystal, S. (2017). Defining industrial action. Federal Law Review, 45(3), 383-414. Daud, Z., & Bakar, M. S. (2017). Improving employees' welfare. European Journal of Industrial Relations, 25(2), 147-162. Deery, S., J., Iverson, R., D., & Walsh, J. (2010). Coping strategies in call centers: Work Intensity and the Role of Co-workers and Supervisors. International Journal of employment relations, 48(1), 189-200. https://doi.org/10.1111/j.1467-8543.2009.00755.x Durrani, S. (2018). Trade Unions in Kenya's War of Independence (No. 2). Vita Books. https://doi.org/10.2307/j.ctvh8r4j2 Dwomoh, G., Owusu, E., E., & Addo, M. (2013). Impact of occupational health and safety policies on employees’ performance in the Ghana’s timber industry: Evidence from Lumber and Logs Limited. International Journal of Education and Research, 1 (12), 1-14. Edinyang, S., & Ubi, I. E. (2013). Studies secondary school students in Uyo Local government area of AkwaIbom State, Nigeria. Global Journal of Human Resource Management, 1(2), 1-8. Ewing, K., & Hendy, J. (2017). New perspectives on collective labour law: Trade union recognition and collective bargaining. Industrial Law Journal, 46(1), 23-51. https://doi.org/10.1093/indlaw/dwx001 Fitzgerald, I., Beadle, R., & Rowan, K. (2020). Trade Unions and the 2016 UK European Union Referendum. Economic and Industrial Democracy. https://doi.org/10.1177/0143831X19899483 Gall, G., & Fiorito, J. (2016). Union effectiveness: In search of the Holy Grail. Economic and Industrial Democracy, 37(1) 189211. https://doi.org/10.1177/0143831X14537358 Gathoronjo, S. N. (2018). The Ministry of labour on the causes of labour disputes in the public sector. University of Nairobi. Iravo, M. A. (2011). Effect of conflict management in performance of public secondary schools in Machakos County, Kenya. Kenyatta University. Jepkorir, B. M. (2014). The effect of trade unions on organizational productivity in the cement manufacturing industry in Nairobi. University of Nairobi. Kaaria, J. K. (2019). Trade Liberalization and Export Survival In Kenya. University of Nairobi. Kaburu, Z. (2010). The relationship between terms and conditions of service and motivation of domestic workers in Nairobi. University of Nairobi. Kambilinya, I. (2014). Assessment of performance of trade unions. Master’s Thesis Submitted to University of Malawi. Kamrul, H., Ashraful, I., & Arifuzzaman, M. (2015). A Study on the major causes of labour unrest and its effect on the RMG sector of Bangladesh. International Journal of Scientific & Engineering Research, 6 (11). Kazimoto, P. (2013). Analysis of conflict management and leadership for organizational change. International Journal of Research in Social Sciences, 3(1), 16-25. Khanka, I. (2015). Industrial relations in Tanzania. University of Dar-es-salaam. Kisaka, C. L. (2010). Challenges facing trade unions in Kenya. Master’s Thesis Submitted to University of Nairobi. Kituku, M. N. (2015). Influence of conflict resolution strategies on project implementation. A Case of Titanium Base Limited Kwale County Kenya. University of Nairobi. Kmietowicz, Z. (2016). Ballot on industrial action by GPs averted as government accepts BMA’s demands. https://doi.org/10.1136/bmj.i4619 KNHCR (2020). Key Business and Human Rights Concerns in Kenya. Retrieved from http://nap.knchr.org/NAP-Scope/Key-Business-and-Human-Rights-Concerns-in-Kenya. Magone, J. (2018). Iberian trade unionism: Democratization under the impact of the European Union. Routledge. https://doi.org/10.4324/9781351325684 Menkel-Meadow, C. J., Porter-Love, L., Kupfer-Schneider, A., & Moffitt, M. (2018). Dispute resolution: Beyond the adversarial model. Aspen Publishers. Mlungisi, E. T. (2016). The liability of trade unions for conduct of their members during industrial action. MoLSP (2020). Ministry of Labor and Social Protection, Registrar of Trade Unions. Retrieved from https://labour.go.ke/department-of-trade-unions/ Msila, X. (2018). Trade union density and its implications for collective bargaining in South Africa. University of Pretoria. Mulima, K. J. (2017). Trade Union Practices on Improvement of Teachers Welfare. University of Nairobi). Năstase, A., & Muurmans, C. (2020). Regulating lobbying practices in the European Union: A voluntary club perspective. Regulation & Governance, 14(2), 238-255. https://doi.org/10.1111/rego.12200 Otenyo, E. E. (2017). Trade unions and the age of information and communication technologies in Kenya. Lexington Books. Powell, J. (2018). Towards a Marxist theory of financialised capitalism. https://doi.org/10.1093/oxfordhb/9780190695545.013.37 Razaka, S. S., & Mahmodb, N. A. K. N. (2017). Trade Union Recognition in Malaysia: Transforming State Government’s Ideology. Proceeding of ICARBSS 2017 Langkawi, Malaysia, 2017(29th), 175..
S-T Bencharif (2022). Either Too Few or Too Many.
J Henley,K Connolly,S Jones,A ; Giuffrida,Robinson (2019). Measuring the availability of human resources for health and its relationship to universal health coverage for 204 countries and territories from 1990 to 2019: a systematic analysis for the Global Burden of Disease Study 2019.
J Feng,L Li,C Wang (2022). The prevalence of turnover intention and influencing factors among emergency physicians: A national observation.
X Sun,M Zhang,Z Lu (2022). Turnover intention and related factors among resident physicians in China under the standardised residency training programme: a cross-sectional survey.
Y Chen,Y You,Y Shen,Z Du,T Dai (2022). Village doctors' dilemma in China: A systematic evaluation of job burnout and turnover intention.
T Mekonnen,T Abera,A Tilahun,A Tadese,T Yadesa (2022). Self-reported turnover intention and associated factors among health professionals in Kafa Zone, Southwest Ethiopia.
H Hou,Y Pei,Y Yang (2021). Factors Associated with Turnover Intention Among Healthcare Workers During the Coronavirus Disease 2019 (COVID-19) Pandemic in China.
De Hert,S ; Mmm,Ajf Cassenote,M Scheffer (2020). Physician turnover in primary health care services in the East Zone of São Paulo City, Brazil: incidence and associated factors.
H Hu,C Wang,Y Lan,X Wu (2022). Machitidze M. Impact of the nurses education and shortage on the patients care outcomes-literature review.
E Smokrović,T Kizivat,A Bajan (2022). A Conceptual Model of Nurses' Turnover Intention.
M Boniol,T Kunjumen,T Nair,A Siyam,J Campbell,K Diallo (2022). The global health workforce stock and distribution in 2020 and 2030: a threat to equity and 'universal' health coverage?.
A Kamarulzaman,K Ramnarayan,A Mocumbi (2022). Plugging the medical brain drain.
A Tansu,K Culp (2022). Risk to Civilian Nuclear Power Plant Workers During the Ukrainian-Russian War.
M Williams,L Armstrong,D Sizemore (2022). Book Review: The Children's Treasure-Trove of Pearls.
B Rathish,R Pillay,A Wilson,V Pillay (2017). Comprehensive Review of Bioterrorism.
C Schaer (2019). The Bunkers That Came In From the Cold. US News.
R Noack,J Horowitz,T Ruff (2021). Ending nuclear weapons before they end us: current challenges and paths to avoiding a public health catastrophe.
C Farkas,G Dudás,G Babinszky,L Földi (2022). Analysis of the Virus SARS-CoV-2 as a Potential Bioweapon in Light of International Literature.
A-E Birn,Y Pillay,T Holtz (2017). The Impact of Armed Conflict on the Epidemiological Situation of COVID-19 in Libya, Syria and Yemen.
V Jm Quinn,T Dhabalia,L Roslycky (2022). COVID-19 at War: The Joint Forces Operation in Ukraine.
J Wells,F Scheibein (2022). Global pandemics, conflict and networks -the dynamics of international instability, infodemics and health care in the 21st century.
M Ikegami,Z Wang (2022). Does military expenditure crowd out health-care spending? Cross-country empirics.
J Kaiman,D Smith,A Anand (2014). How sick are the world's healthcare systems? The Guardian.
M Rahman,U Ghoshal,K Ragunath (2020). Biomedical research in developing countries: Opportunities, methods, and challenges.
Cazzolla Gatti,R Geddes,L (2021). Why We Will Continue to Lose Our Battle with Cancers If We Do Not Stop Their Triggers from Environmental Pollution.
J Goss (2022). Health Expenditure Data, Analysis and Policy Relevance in Australia, 1967 to 2020.
Azra Cader,Lakwimashi Perera (2011). Understanding the Impact of the Economic Crisis on Child and Maternal Health Among the Poor: Opportunities for South Asia.
W Bao,R Tao,A Afzal,H Dördüncü (2022). Real Estate Prices, Inflation, and Health Outcomes: Evidence From Developed Economies.
O Guerra,Vio Agyapong,N Nkire (2022). A Qualitative Scoping Review of the Impacts of Economic Recessions on Mental Health: Implications for Practice and Policy.
H Jung,Y Kwon,Jw ; Noh,S Jimenez Rincon,N Dou,Murray Kolb,L (1995). Financial burden of catastrophic health expenditure on households with chronic diseases: financial ratio analysis [published correction appears.
S O'lear,A ; Gray,A Samadikuchaksaraei,W Mousavizadeh K ; Selassie,Jacob (2006). HOLDING ON TO THE MAN ANGEL YHWH! Symbolize a Nation and People Holding on to Their Faith and Received a Blessing.
E Wong,U The (2022). wants to counter China's moves in Africa. but American officials try not to mention that.
V Bisset,K Nichols,A Chapman,J Bikales,P Villegas,Thebault (2022). Unknown Title.
V Yazdi Feyzabadi,A Haghdoost,M Mehrolhassani,Z Aminian (2015). The Association between Peace and Life Expectancy: An Empirical Study of the World Countries.
M Kruk,A Gage,C Arsenault (2018). High-quality health systems in the Sustainable Development Goals era: time for a revolution [published correction appears in.
A Takian,G Rajaeieh,R Salami (2020). A letter in the Lancet of June 2020¹ claimed the COVID-19 pandemic teaches lessons we must embrace to overcome two additional existential threats: nuclear war and global warming. What lessons can we learn from the global response to COVID-19 that could help the world address future threats such as climate change or the proliferation of nuclear weapons? ¹Muller and Nathan.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
Abdul Kader Mohiuddin. 2026. \u201cGlobal Health Issues with Conflict Escalation among Pandemic, Climate, and Economic Crises\u201d. Global Journal of Human-Social Science - H: Interdisciplinary GJHSS-H Volume 23 (GJHSS Volume 23 Issue H1): .
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Religion, governance, and politics-as well as related topics such as human rights, justice, and so on-have historically caused many of the world’s most significant conflicts, and they continue to do so because these issues are often the most fundamental in the structure of a society. To gain a military advantage, parties to armed conflicts have polluted water, burned crops, cut down forests, poisoned soils, and killed animals over the years. A variety of context factors, particularly socioeconomic conditions, governance, and political factors, interact and play a key role in translating climate change into conflict risks. The present unrest all over the world risks putting more than half of the countries into a crisis of health, economy, and social safety, which is the biggest threat to human civilization. The security and safety of healthcare facilities, workers, and supply lines remain paramount concerns along with access to health services, technology, and innovation.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.