Lipedema is defined as a genetic disorder that affects the mass of adipose tissue and its distribution, due to abnormal deposition of fat in the buttocks and legs, bilaterally. The characteristic symptoms are pain, tightness, and a tendency to hematomas. The onset of lipedema is typically triggered by hormonal changes (puberty, pregnancy, menopause, stress). This condition affects almost exclusively women, leading to considerable disability, impaired daily functioning, and psychosocial distress. A survey carried out in 2022 by the Department of Vascular Surgery of the Amato Institute revealed that the prevalence of lipedema in the population of Brazilian women is 12.3%. Research on this disease is still scarce, considering that it has a difficult diagnosis, heterogeneous picture, and lack of objective measurement instruments to characterize the conditions. The cause of this chronic progressive condition is still unexplained, but there are some hypotheses about its pathophysiology. As it usually manifests itself in periods of hormonal change and is characterized by a disproportionate distribution of body fat, this condition is believed to be mediated by estrogen. Thus, through this study, we seek to clarify the general aspects, pathogenesis, diagnosis, treatment, and complications of lipedema.
## I. INTRODUCTION
Lipedema is a chronic and progressive disease, characterized by its abnormal subcutaneous fat tissue distribution, resulting in its excess, especially in the lower extremities, bilaterally and symmetrically; it also presents frequent hematomas due to small trauma injuries. This disease affects almost exclusively women, being that the initial manifestations of this condition commonly appear in phases of hormonal changes, like in puberty, pregnancy, or menopause. $^{1,2}$ The major signs of this pathology are the presence of accumulation of body fat in the thighs, legs, and arms; in terms of symptoms, patients often report pain and swelling in the legs. Research made in 2022 by the Instituto Amato revealed that over $12.3\%$ of Brazilian women that participated in this study have lipedema and that the estimates of the prevalence of lipedema in the general population range from 0.006 to $10\%$. There is a large case of underdiagnosis of this condition due to the lack of instruments and reliable tests for this purpose, therefore, despite being a particular condition, it is often confused with more frequently diagnosed diseases, such as obesity and lymphedema[3].
Nowadays, the complexity and multifactorial character of this pathology have been increasingly highlighted. Besides affecting the body, this disorder also affects the patient's mental state, considering that the symptoms, by causing a visible disproportion between a standard upper body and thickened lower limbs, can negatively affect self-esteem regarding their appearance, in addition to the possibility of physically limiting daily activities. Therefore, the patient's quality of life is drastically reduced. The stigmatization, labeling, and minimization of suffering affect the mental states of patients with lipedema, which makes it difficult to implement effective therapy and increases the level of pain experienced by them.[1,2]
Regarding that, this work aims to discuss the data presented in the literature concerning lipedema, more specifically on its pathogenesis, diagnosis, complications and treatment. After all, there isn't much research on the subject, so this study intends to synthesize the information already produced on the subject.
The authors declare that there is no conflict of interest.
## II. METHODS
Seven articles from de last five years were selected from de the PubMed database using the keywords: lipedema, pathogenesis, diagnosis and treatment, in English. The filter "free full article" was also applied. Case reports and articles that were not related to the topic were excluded.
The results obtained in the research carried out in the PubMed database using the parameters described in the methodology of this article are listed below. The presentation of results is arranged in a table containing: the year; publication title; journal/source; publication type; author.
Table 1: Identification of the articles, according to year; publication title; journal/source; publication type; author
<table><tr><td>Publication Title</td><td>Author</td><td>Year</td><td>Journal/source</td><td>Publication type</td></tr><tr><td>Lipedema-Pathogenesis, Diagnosis, and Treatment Options</td><td>KRUPPA, P.; et al.</td><td>2020</td><td>Deutsches Ärzteblatt International</td><td>Article</td></tr><tr><td>Standard of care for lipedema in the United States</td><td>HERBST, K.; et al.</td><td>2021</td><td>Phlebology: The Journal of Venous Disease</td><td>Article</td></tr><tr><td>Lipoedema is not lymphoedema: A review of current literature</td><td>SHAVIT, E.; et al.</td><td>2018</td><td>International Wound Journal</td><td>Article</td></tr><tr><td>Update in the management of lipedema</td><td>CORDERO, I. F.; et al.</td><td>2021</td><td>International Angiology</td><td>Article</td></tr><tr><td>Lipedema: A Call to Action!</td><td>BUSO, G.; et al.</td><td>2019</td><td>Obesity (Silver Spring)</td><td>Article</td></tr><tr><td>Lipoedema as a Social Problem. A Scoping Review</td><td>CZERWINSKA, M.; et al.</td><td>2021</td><td>International Journal of Environmental Research and Public Health</td><td>Article</td></tr><tr><td>Translation, cultural adaptation, and validation of a lipedema symptoms questionnaire</td><td>AMATO, A. C. M.; et al.</td><td>2020</td><td>Jornal Vascular Brasileiro</td><td>Article</td></tr></table>
## III. DEVELOPMENT
### 1. Pathogenesis
The pathogenesis of lipedema is not completely clarified. To date, there is still no specific biomarker associated with the onset of the disease, so the diagnosis is made based on the patient's clinic and the exclusion of differential diagnoses. However, some studies have shown that positive family history is present in approximately $60\%$ of patients. Furthermore, changes in the process of adipogenesis, hormonal, microvascular and lymphatic disorders may be related to the abnormal deposition of subcutaneous adipose tissue that characterizes lipedema.
Concerning adipogenesis, previous research has found that in the analysis of the vascular stromal fraction obtained in liposuction of 52 patients with lipedema, there was an increase in the amount of adipose stem cells. Regarding angiogenesis, it was found that patients undergoing shockwave therapy for lipedema had elevated serum levels of endothelial vascular growth factor, suggesting the role of pathological angiogenesis in the development of the disease. Moreover, in non-obese lipedema patients, increased numbers of macrophages, blood vessels and capillary dilation were also verified, which reinforces the hypothesis that changes in microcirculation contribute to the manifestation of the disease. $^{1}$
Another point of investigation is the possible role of genes that suffer the influence of estrogen in the development of endothelial dysfunctions and lymphadenopathies, since it is a fundamental mediator in sympathetic innervation in subcutaneous adipose tissue, in specific areas of the body besides being an important modulator of lipid metabolism, through alpha and beta estrogen receptors, which could explain the higher prevalence of this condition in women. It is also believed that the imbalance of estrogen-mediated weight control mechanisms in the central nervous system may also be related to the accumulation of fat that happens in this pathology. Research has shown that the addition of alpha estrogen receptors in female laboratory rats resulted in hyperphagia and hypermetabolism, suggesting that changes in the estrogen pathway may explain weight loss resistance in patients with lipedema. $^{1}$
Despite the interesting findings of previous research, it is important to emphasize that these are speculative results and without strong scientific evidence, which justifies the need for continuity of studies on the subject, to further elucidate the pathogenesis of lipedema.
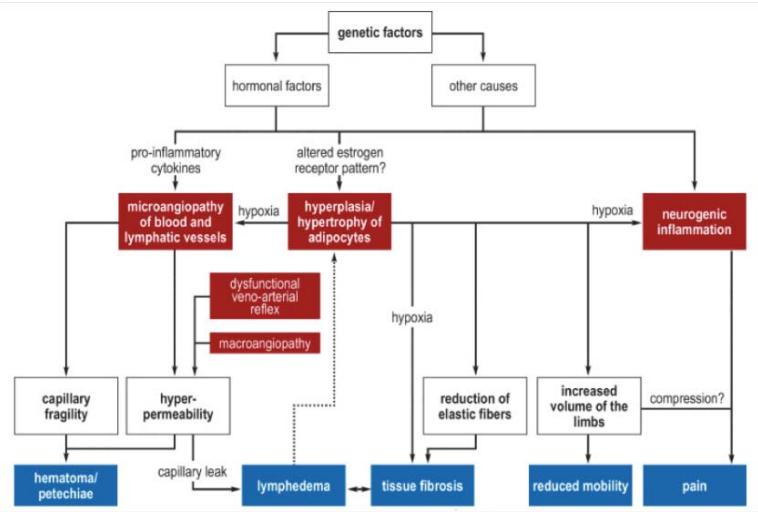 Figure 01: Flowchart illustrating the pathogenesis of lipedema
Source: KRUPPA, P.; et al., 2021
#### 2. Diagnosis
As previously discussed, lipedema's diagnosis, due to the lack of specific biochemical markers that can identify the disease, is based mainly on the patient's clinical status and on the exclusion of differential diagnoses, such as obesity, lymphedema, Dercum's disease and chronic venous disease, which are all wrongly diagnosed as lipedema. Besides, due to presenting heterogenic manifestations in different patients, a sound assessment of the patient's history, symptoms, and physical examination is absolutely necessary. The main findings during examination in patients diagnosed with lipedema consist of frail and stretched aspects of the skin, hematomas, disproportional accumulation of fat tissue on the limbs, except for the hand and feet, and also the intensification of symptoms like swelling and sensitivity during the day.[2] When it comes to the exclusion of differential diagnoses, such as obesity, it is important to emphasize that lipedema is normally influenced by moments of shifting hormonal concentration, such as puberty, menopause and pregnancy, which can help differentiate the pathologies. Furthermore, the preservation of hands and feet of the fat accumulation, less influence of the diet over the symptoms and the associated presence of psychiatric comorbidities are also favorable to it being, in fact, lipedema. However, there are cases of obese patients in which the concomitant presence of lipedema can be elucidated by symptoms such as pain, sensitivity and hematomas, as previously discussed. There are also cases where the diagnosis can only be certain after bariatric surgery because only after a considerable weight loss it is possible to notice the irregular distribution of fat tissue.
On physical examination, it is possible that the doctor will notice the presence of nodules and edema, which increase in size as the disease progresses, in addition to discomfort and pain when performing the Pinch Test, used to assess skin flaccidity. In more advanced cases, lymphedema and a positive Stemmer sign can also be observed (where the examiner is no longer able to squeeze a skin fold in the basal joint of the feet or hands).[2]
According to the findings of the examination, lipedema can be characterized in three stages:[2,4]
- Stage I: Presence of small nodules, reversible edema, smooth skin with a soft homogenous increase of the subcutaneous tissue, cold skin in certain areas, due to functional vascular imbalance;
- Stage II: Almond sized nodules, reversible or irreversible edema, irregular skin surface, nodular alterations of the subcutaneous tissue;
- Stage III: Deforming fat deposits, macronodular changes, potentially Stemmer sign positive lymphedema, sensitive subcutaneous nodules, a relevant increase of loose skin/tissue circumference, protruding fat mainly on the inner thighs and knees.
Aside from this characterization, this disease can be classified into five different types depending on the location of the fat nodules:[2,5]
- Type I: Affects the buttocks;
- Type II: Affects the buttocks, hips and thighs;
- Type III: Affects buttocks, hips, thighs and calves;
- Type IV: Affects the arms;
- Type V: Affects the calves.
It is important to emphasize that type IV is often associated with types II or III.2
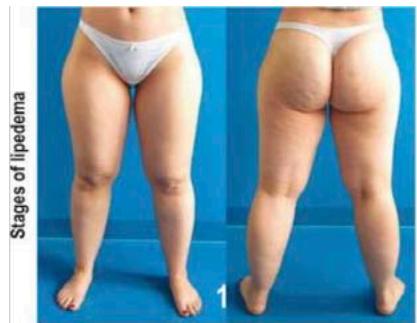
1. thickened subcutis, soft, with small, palpable nodules, skin surface still smooth
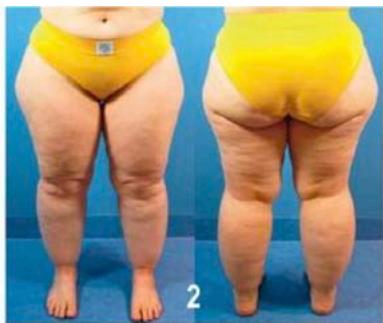 Classification by stage 2) thickened subcutis, soft, some larger nodules, skin surface uneven
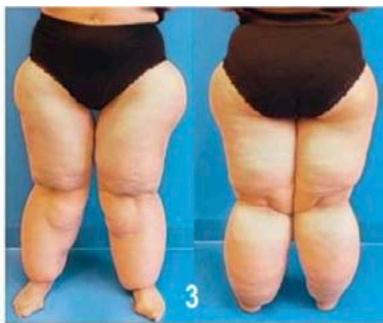 3) thickened subcutis, hardened, with large nodules, disfiguring fat deposition
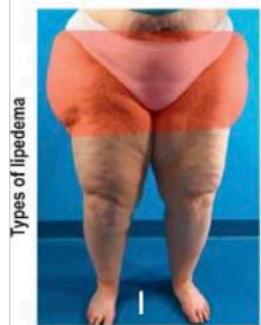
1. buttock
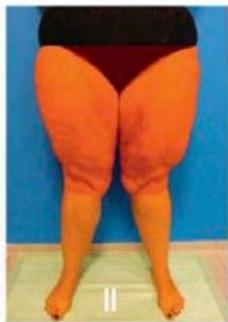 II) thigh
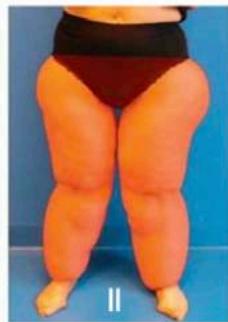 Classification by morphology III) entire lower limb
 IV) arm\*
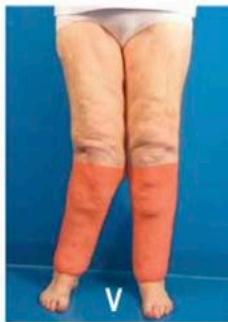 V) leg * Type IV is often associated with type II or III. Fonte: KRUPPA, P.; et al., 2021 Figure 02: Classification of lipedema according to stage and type On the other hand, laboratory analyzes are relevant for the investigation of possible differential diagnoses, being common the analysis of liver, kidney and thyroid function, in addition to lipid and glycemic profile. Regarding diagnostic imaging methods, such as X-ray, magnetic resonance imaging and computed tomography, although they allow qualitative and quantitative assessment of the subcutaneous tissue, there is little evidence that demonstrates a great impact on the diagnosis of lipedema, with its most common use in the investigation of differential diagnoses, such as lymphedema.[2]
Lipedema has, in general, a heterogeneous and variable progression, as some individuals may have a stabilization of the disease over time, while others may have a gradual progression. Considering the evolution of lipedema, the most common complaints are orthostatic edema, pain with digital pressure on the affected limbs, hematomas, fatigue and discomfort in the legs. In addition, excess fat in the buttocks, hips, thighs and legs interfere with gait and the misalignment of the mechanical axis of the leg, promoting joint stress that can progress to valgus osteoarthritis of the knee, antalgic gait and/or excessive pronation of the knees. feet. Considering that obesity is a risk factor for lipedema and that women with this disease are at increased risk of developing morbid obesity, it is thought that these patients would have a severe cardiovascular profile. However, according to BUSO et al, fat with gynoid distribution of lipedema correlated negatively with insulin resistance after adjustment for total fat and, consequently, with a less severe cardiovascular profile. This conclusion of cardiovascular risk for patients with lipedema has not been well elucidated. $^{1}$ Thus, more concrete studies are needed to clarify more clearly the pathophysiology and complications generated by lipedema.
Lipedema has two treatments recognized by studies and research: conservative treatment and surgery. Lipedema therapy has as its main objectives the relief of symptoms, slowing down the progression of the disease and preventing complications.[6] It is important to emphasize that, currently, there is no known treatment that leads to the cure of this pathology.[2]
Conservative treatment consists of manual lymphatic drainage, compression therapy, physical exercises and diet with weight control, which can be combined with pneumatic compressions, if available.[2,6,7]
Manual lymphatic drainage, compression therapy and physical exercise, together comprise the pillars of therapy to decongest the lymphatic vessels of the affected limbs, stimulating flow and reducing edema. Drainage should be performed regularly and has been proven to reduce pain and inflammation. $^{2}$ Compression therapy should be recommended by the physician and varies according to the degree of presentation of each patient's disease.
Physical exercise should be performed by all those diagnosed with the disease, regardless of the degree of involvement, and the degree of resistance of each individual should be respected. It is important to note that exercises performed in water, such as swimming and water aerobics, are highly recommended, since the hydrostatic pressure of the water aids in the drainage of the limbs.
The anti-inflammatory diet, despite being a pillar of the conservative treatment of lipedema, does not have published scientific evidence proving the help in controlling the symptoms and the evolution of the disease. However, the nutritional component, seeking to inhibit ongoing systemic inflammation, it is empirically indicated by several professionals who study this pathology. Furthermore, diet as a component of weight control and reduction of total body fat has been shown to be effective in reducing the symptoms caused by lipedema.
Pneumatic compressions can be used to aid conservative treatment to reduce edema and pain in affected limbs.[2,7]
The surgical treatment for this pathology consists of liposuction. Normally, patients undergoing liposuction must have followed conservative treatment for at least 6 months without improvement in their quality of life, that is, with unsatisfactory results.[2] Liposuction in the affected limb would have as main objectives to reduce the evolution of the disease and symptoms of the patient, improving the individual's mobility, reducing the need for compression therapy and lymphatic drainage.[2,7] Currently, the hydroliposuction technique is the most recommended for patients with lipedema, as it reduces damage to the lymphatic tissues.[6]
Liposuction performed for the treatment of lipedema should be performed by a professional with experience in this type of treatment, since the volumes of fat removed will possibly exceed those traditionally recommended. Furthermore, multiple surgical interventions may be required to obtain the desired outcome.[2]
## IV. CONCLUSION
Lipedema is unknown to part of the medical community and commonly confused with some diseases such as lymphedema and obesity and is therefore often underdiagnosed. Its diagnosis is divided into three stages and five types, depending on the area of the affected body. Lipedema can significantly impact the patient's quality of life if not diagnosed early. Several studies prove the importance of treatment, especially conservative treatment, for the evolution of the disease since there is no known cure.
Treatment may involve manual lymphatic drainages, weight control, an anti-inflammatory diet, compressive stockings and even liposuction of affected areas, depending on the patient's clinical picture. While there are scientific shreds of evidence that corroborate the efficacy of treatment in improving the symptoms of this pathology, its pathogenesis is not yet fully clarified. Further and more extensive studies and research on the subject are still needed to elucidate the pathophysiology better.
Generating HTML Viewer...
References
7 Cites in Article
Giacomo Buso,Colab (2019). Unknown Title.
Philipp Kruppa,Iakovos Georgiou,Niklas Biermann,Lukas Prantl,Peter Klein-Weigel,Mojtaba Ghods (2020). Lipedema—Pathogenesis, Diagnosis, and Treatment Options.
Alexandre Amato,Fernando Amato,Daniel Benitti,Ricardo Santos (2020). Tradução, adaptação cultural e validação do questionário de avaliação sintomática do lipedema (QuASiL).
Monika Czerwińska,Paulina Ostrowska,Rita Hansdorfer-Korzon (2021). Lipoedema as a Social Problem. A Scoping Review.
Eran Shavit,Uwe Wollina,Afsaneh Alavi (2018). Lipoedema is not lymphoedema: A review of current literature.
Isabel Forner-Cordero,Angeles Forner-Cordero,Győző Szolnoky (2021). Update in the management of lipedema.
Karen Herbst,Linda Kahn,Emily Iker,Chuck Ehrlich,Thomas Wright,Lindy Mchutchison,Jaime Schwartz,Molly Sleigh,Paula Donahue,Kathleen Lisson,Tami Faris,Janis Miller,Erik Lontok,Michael Schwartz,Steven Dean,John Bartholomew,Polly Armour,Margarita Correa-Perez,Nicholas Pennings,Edely Wallace,Ethan Larson (2021). Standard of care for lipedema in the United States.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
Thaís Amorim Clemente. 2026. \u201cLipedema and its Main Characteristics: A Literary Review\u201d. Global Journal of Medical Research - F: Diseases GJMR-F Volume 23 (GJMR Volume 23 Issue F3): .
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Lipedema is defined as a genetic disorder that affects the mass of adipose tissue and its distribution, due to abnormal deposition of fat in the buttocks and legs, bilaterally. The characteristic symptoms are pain, tightness, and a tendency to hematomas. The onset of lipedema is typically triggered by hormonal changes (puberty, pregnancy, menopause, stress). This condition affects almost exclusively women, leading to considerable disability, impaired daily functioning, and psychosocial distress. A survey carried out in 2022 by the Department of Vascular Surgery of the Amato Institute revealed that the prevalence of lipedema in the population of Brazilian women is 12.3%. Research on this disease is still scarce, considering that it has a difficult diagnosis, heterogeneous picture, and lack of objective measurement instruments to characterize the conditions. The cause of this chronic progressive condition is still unexplained, but there are some hypotheses about its pathophysiology. As it usually manifests itself in periods of hormonal change and is characterized by a disproportionate distribution of body fat, this condition is believed to be mediated by estrogen. Thus, through this study, we seek to clarify the general aspects, pathogenesis, diagnosis, treatment, and complications of lipedema.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.