## I. INTRODUCTION
In the present era of exponential industrialization and global changes in lifestyle, infertility cases are on an increasing trend. Assisted reproductive technology has become a widespread choice for the treatment of infertility in recent decades. Simple assisted reproduction techniques include induction of ovulation, follicular scanning and intrauterine insemination. If multiple cycles fail or if there is a tubal factor, or a male factor etc., the patients are then recommended in vitro fertilization and embryo transfer popularly referred to as IVF-ET[^1].
The increased incidence of multifetal pregnancies has been attributed to two mainfactors: 1) Increased maternal a geat conception, when multifetal gestations are more likely to occur naturally and 2) increased use of assisted reproductive technology (ART), which is more likely to result in multifetal gestation[^2]. Multifetal pregnancies are associated with increased risk of maternal complications like preeclampsia, eclampsia, preterm delivery, cesarean delivery, and postpartum hemorrhage. Also, there is increased incidence of neonatal morbidity and mortality compared to singleton pregnancies[^3]. In spontaneously conceived (SC) pregnancies, the incidence of multifetal gestation is about $2\%$, while it is up to $40\% - 50\%$ in in vitro fertilization (IVF) conceived pregnancies[^4]. Studies have been done to compare the outcomes between spontaneously conceived twins and those conceived by assisted reproductive techniques (ART). However, many studies are inconclusive and contradictory in their findings. We planned our study to compare the maternal and fetal outcomes among dichorionic-diamniotic (DCDA) twin pregnancies. The primary objective was to examine whether DCDA twin pregnancies conceived after ART were at a higher risk of adverse outcomes as compared to their spontaneously conceived counterparts. The secondary objective was to assess the maternal and fetal complications in the twin pregnancies.
## II. METHODOLOGY
### a) Study Design
We conducted a prospective observational study at a South Indian tertiary care center from June 2022 to July 2023. The DCDA twin pregnancies that were booked at our center and consented to be a part of the study were recruited using convenient sampling technique. We limited our study to only DCDA twin pregnancies to eliminate the bias of higher morbidities associated with monochorionic twin pregnancies. They were divided into two groups- one that conceived spontaneously and the second that conceived after ART (OI (ovulation induction), ICSI (intracytoplasmic sperm injection) \*IVF (in vitro fertilization). We excluded women with higher order multiple pregnancies, twins reduced to singleton, triplets reduced to twins, twins with early vanishing twins, and those conceived after only IUI conception. The study was started after receiving the Institutional Review Board approval (EC Reference No. 11_2022).
### b) Sample Size
The sample size was calculated assuming the expected proportion of stillbirth in the non-exposure (Spontaneous) group as $20\%$ and the relative risk of stillbirth in ART (exposure) based on the previous hospital records. The required sample size was calculated using the formula proposed by Kirkwood BR et al. The required sample size as per the formula was 270 where 1:2 ratio applied for non-exposure it will be 90 babies and for exposure it will be 180 babies. To account for a non-participation rate/ loss to follow up rate of about $20\%$, another 18 and 36 twin babies will be added to the sample size. Hence the final required sample size would be 108 and 216 twin babies in non-exposure and exposure groups respectively. We converted the sample size for twin pregnant mothers, it was 54 and 108 mothers in spontaneous and ART groups respectively.
### c) Data Collection and Analysis
Data was collected from the electronic medical records and operative notes in a preset proforma. The same was compiled in excel sheet after completion of the sample size. The primary variable was the composite adverse outcome of any of the major maternal and fetal morbidities. For normally distributed quantitative parameters the mean values were compared between study groups using an independent sample t-test (2 groups).
For non-normally distributed quantitative parameters, medians and Interquartile range (IQR) were compared between study groups using Mann Whitney U test (2 groups). Categorical outcomes were compared between study groups using the Chi-square test. P value $< 0.05$ was considered statistically significant. Data was analyzed by using coGuide software version 1.0.
## III. RESULTS
Total of 162 dichorionic diamniotic twin pregnancies were included, among which the ART group consisted of 108 (66.67%) pregnancies and the spontaneous group encompassed 54 (33.33%) pregnancies.
### a) Demographic Comparison
In our study, 53 (98.15%) participants were aged \<35 years in spontaneous conception group and in ART conception group, 87 (80.56%) participants were aged \<35 years. 25 (46.3%) participants were primigravida and 29 (53.7%) were multigravida in spontaneous conception group whereas in ART conception group, 59 (54.63%) were primigravida and 49 (45.37%) were multigravida. In both the study groups, maximum number of mothers gained weight more than 15 kg. In our study most of them delivered by LSCS i.e., 52 (96.3%) participants in spontaneous conception group and in ART conception group, 104 (96.3%) delivered by LSCS. Table 1 shows the demographic details of the study population.
Table 1: Demography
<table><tr><td rowspan="2"></td><td colspan="2">Study Group</td><td rowspan="2">Chi square value</td><td rowspan="2">P value</td></tr><tr><td>Spontaneous Conception (N=54)</td><td>ART Conception (N=108)</td></tr><tr><td colspan="5">Age (years)</td></tr><tr><td><=35</td><td>53 (98.15%)</td><td>87 (80.56%)</td><td rowspan="2">9.494</td><td rowspan="2">0.002*</td></tr><tr><td>>35</td><td>1 (1.85%)</td><td>21 (19.44%)</td></tr><tr><td colspan="5">Gravida</td></tr><tr><td>Primi</td><td>25 (46.3%)</td><td>59 (54.63%)</td><td rowspan="2">1.001</td><td rowspan="2">0.317*</td></tr><tr><td>Multi</td><td>29 (53.7%)</td><td>49 (45.37%)</td></tr><tr><td colspan="5">weight gain (Kg) (N=162)</td></tr><tr><td>Upto 5 Kg</td><td>2 (3.7%)</td><td>10 (9.26%)</td><td rowspan="4"></td><td rowspan="4">0.129*</td></tr><tr><td>5-10 Kg</td><td>15 (27.78%)</td><td>20 (18.52%)</td></tr><tr><td>10-15 Kg</td><td>12 (22.22%)</td><td>38 (35.19%)</td></tr><tr><td>>15 Kg</td><td>25 (46.3%)</td><td>40 (37.04%)</td></tr><tr><td colspan="5">Mode of delivery</td></tr><tr><td>LSCS</td><td>52 (96.3%)</td><td>104 (96.3%)</td><td rowspan="2">0.00</td><td rowspan="2">1.000*</td></tr><tr><td>Vaginal</td><td>2 (3.7%)</td><td>4 (3.7%)</td></tr></table>
### b) Maternal Outcome
In our study, maternal outcomes like hypertensive disorders (12.96%), gestational diabetes mellitus 47 (43.52%) and postpartum hemorrhage (12.96%) were higher in the ART group, whereas intrahepatic cholestasis of pregnancy cases were noted higher in the spontaneous group i.e., in $7.41\%$ cases. Among the four maternal outcomes, Hypertensive disorders (P value 0.001) and gestational diabetes mellitus (P value 0.016) were statistically significant. Figure 2 shows the comparison of the maternal outcomes in both the groups.
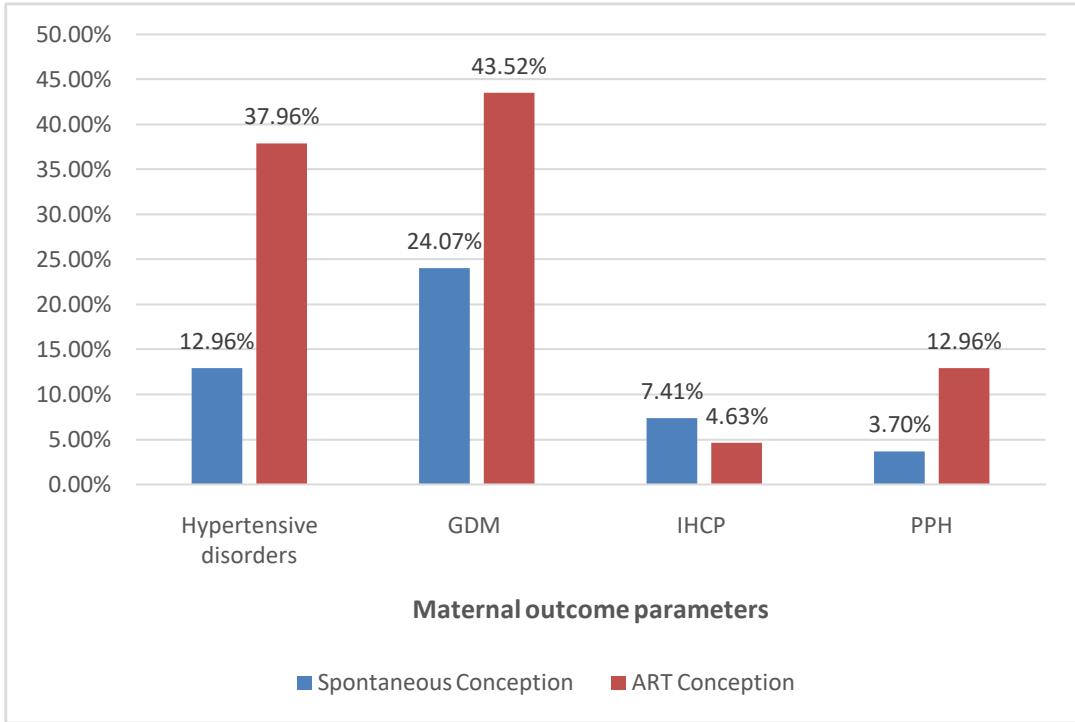 Figure 2: Comparison of Maternal Outcome Parameters with Study Group
### c) Neonatal Outcome
In spontaneous conception group no babies birthed between 28 to 32 weeks, 12 birthed (11.11%) between 32.1 to 34 weeks, $60(55.56\%)$ between 34.1 to 36.6 weeks and 36 $(33.33\%)$ are 37 weeks. In ART conception group, $18(8.33\%)$ babies are between 28 to
32 weeks, 34 (15.74%) between 32.1 to 34 weeks,110 (50.93%) between 34.1 to 36.6 weeks and 54 (25%) are
$\geq 37$ weeks. Figure 3 gives a graphical representation of these results.
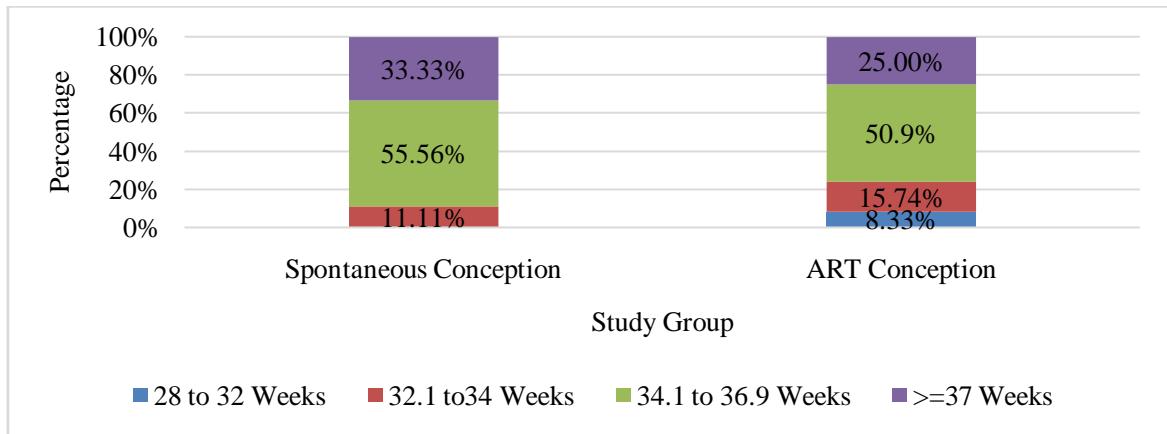 Figure 3: Stacked Bar Chart of Comparison of Preterm with Study Group
In spontaneous conception, APGAR $<=7$ at 5 minutes of birth seen in 2 (1.85%) babies and in 15 (6.94%) babies in ART conception. These are represented in figure 4.
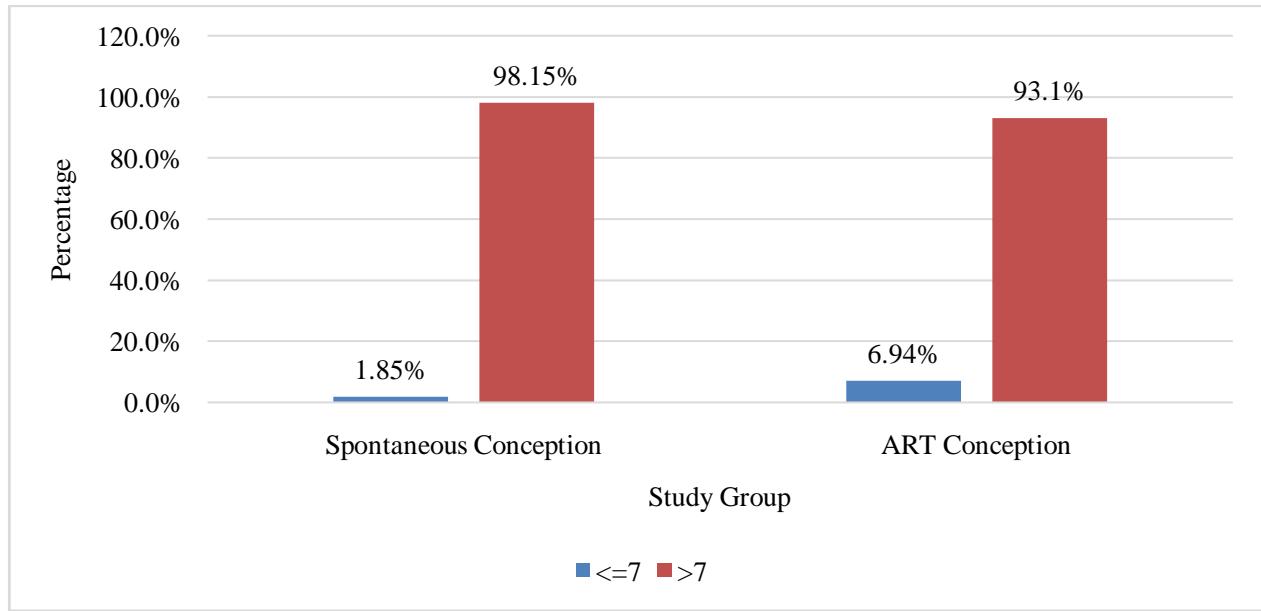 Figure 4: Cluster Bar Chart of Comparison of APGAR at 5 min Between Study Group (N=324)
In the spontaneous conception group, 76 (70.37%) babies were admitted in NICU for more than 48 hours and in ART conception 166 (76.85%) babies admitted.FGR babies were 54 (50%) in spontaneous conception group and 72 (33.33%) in ART conception group.
3 (2.78%) babies in spontaneous conception group and 19 (8.8%) in ART conception group had anomalies.
There was no fetal demise in spontaneous conception group, and 4 (1.85%) fetal demise babies were seen in ART conception group. In spontaneous conception group, no babies had intraventricular hemorrhage (IVH) and retinopathy of prematurity (ROP). In ART conception group 2 (0.93%) babies had IVH and
7 (3.24%) babies had ROP that required treatment. Figure 5 gives the graphical details of the neonatal outcomes. Of all the neonatal outcomes, Prematurity(P value 0.005), APGAR at 5 mins (P value 0.053),fetal anomalies(P value 0.042),FGR(P value 0.004) were statistically significant.
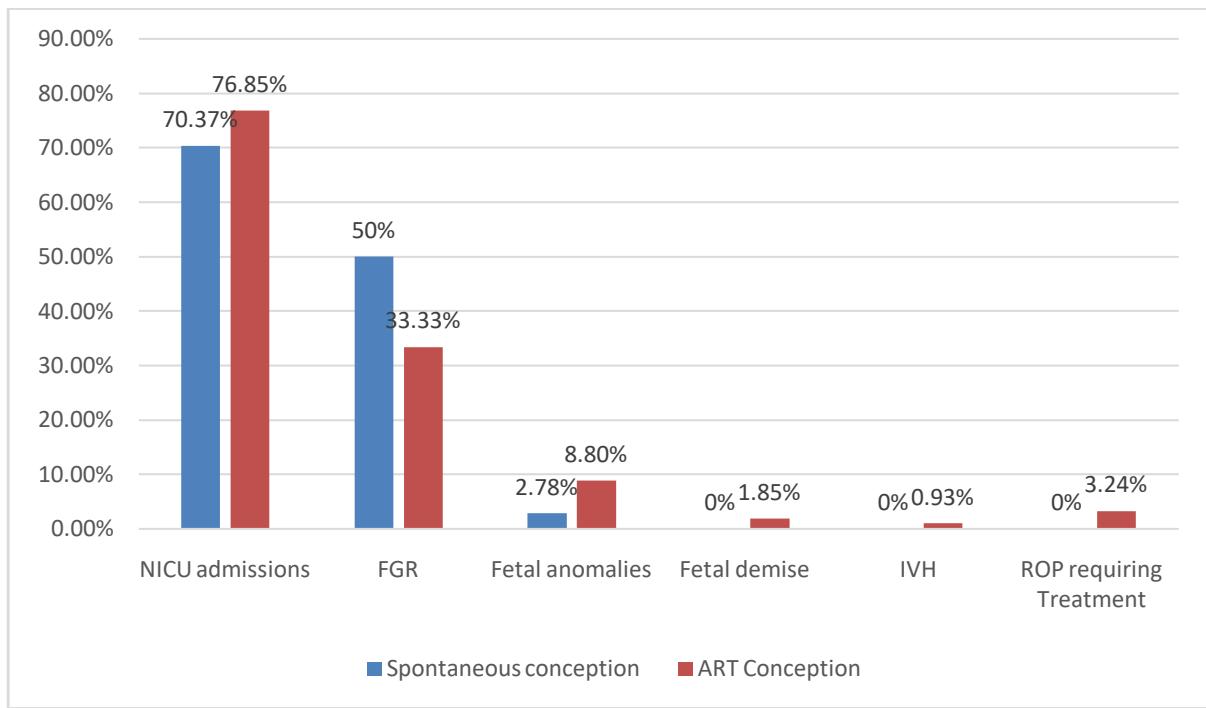 Figure 5: Comparison of Neonatal Outcome Parameters with Study Group
## IV. DISCUSSION
The current prospective study included a total of 162 dichorionic diamniotic (DCDA) twin pregnancies, i.e., spontaneous conception group with 54 DCDA twin pregnancies conceived spontaneously and the other group is ART conception group, that included 108 DCDA twin pregnancies conceived by assisted reproductive techniques like ovulation induction, in vitro fertilization, intracytoplasmic sperm injection based on the inclusion criteria and both the groups were compared for the maternal and perinatal outcomes.
Overall, most of the mothers in our study were less than 35 years of age. Older women more than 35 years were more in ART group which is statistically significant (P value $<0.002$ ). The studies done by Ching Hong Ho and Preeti Patil et al also noted the same findings in relation to maternal age. The other demographic outcomes like parity, weight gain and mode of delivery were statistically insignificant. Maternal outcomes like Hypertensive disorders and Gestational diabetes were more in the ART group with statistical significance which are in line with the studies done by Diana Rashid et al and Hua Chen et al. The other maternal outcomes like IHCP and PPH were statistically insignificant in our analysis.
Our study showed that premature twins were more in the ART group than the spontaneous group and the results were statistically significant (P value 0.005). Similar findings were noted in studies done by Geisler et al[^7] and Caserta D et al[^8].
The 5 minute APGAR score of less than 7 was found to be more in the ART group which was statistically significant. Study by Ching Hong HO et al $^{5}$ showed the prevalence of twins with APGAR less than 7 at 5 minutes was more in spontaneous group (7.4%) compared to ART group (1.4%). But other studies such as those done by Leila Pourali et al $^{9}$ showed no difference between the two groups in the prevalence of twins with APGAR less than 7 at 5 minutes.
When other neonatal outcomes like NICU admissions for more than 48 hours, fetal demise, intraventricular hemorrhage, retinopathy of prematurity requiring treatment were compared between the 2 groups, they were found to be statistically insignificant. The prevalence of fetal anomalies in our study was overall more in the ART group which was statistically significant. This showed that the twins conceived by ART had a higher risk of structural abnormalities as compared to those that conceived spontaneously.
Diana Rashid et al[^6], also concluded the same in their study. In our study the prevalence of fetal growth restriction was more in the spontaneous group (50%) than ART group (33.33%), which was statistically significant. This was the only fetal morbidity that was found higher among the spontaneously conceived group as compared to the ART group in our study. Studies done by Da Silva et al[^10] and Leila Pourali et al[^9] have showed the prevalence of fetal growth restriction to be more in the ART group but, there was no statistical difference between the two groups. There were no cases of neonatal and perinatal mortality in our study.
## V. CONCLUSION
The present study concluded that mothers in ART group were older and mostly primigravida. Maternal complications like hypertension, gestational diabetes mellitus and neonatal complications like premature birth before 34 weeks, APGAR less than 7 at 5 minutes and fetal anomalies were significantly higher in ART group. Our study also concluded that fetal growth restriction was significantly higher in the spontaneously conceived group.
The findings of this study, strengthen the evidence of higher overall adverse maternal and neonatal outcomes among twin pregnancies conceived after ART versus those that are conceived spontaneously.
Author Contributions
-Data collection, conduct, analysis.
- Second author -Dr. Maimoona Ahmed -Planning, analysis, writing.
Third author -Dr.Prathiba Reddy
-Planning, design.
Generating HTML Viewer...
Funding
No external funding was declared for this work.
Conflict of Interest
The authors declare no conflict of interest.
Ethical Approval
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
Dr. P. Siva Ranjani Priya. 2026. \u201cMaternal and Perinatal Outcomes in Twins Conceived Spontaneously Versus by ART – A Prospective Observational Study\u201d. Global Journal of Medical Research - E: Gynecology & Obstetrics GJMR-E Volume 24 (GJMR Volume 24 Issue E1): .
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
×
This Page is Under Development
We are currently updating this article page for a better experience.
Thank you for connecting with us. We will respond to you shortly.