## I. INTRODUCTION
Hypernatremia consists of a serum sodium concentration exceeding $145\mathrm{mEq/L}$, constituting a relatively infrequent condition in newborns [1-7]. The exact incidence of hypernatremia in newborns remains uncertain but is estimated to range between $1\%$ to $5.6\%$ [1,6,8]. In neonates, hypernatremic dehydration (HD) is more commonly observed in those exclusively breastfed or with excessive weight loss, with early discharge from the hospital being a significant risk factor. In these cases, HD is associated with ineffective lactation due to insufficient milk production or inadequate support [1-7,9-11].
Initial symptoms of HD are nonspecific, which can lead to delayed diagnosis and subsequent treatment. Consequently, many newborns with HD experience prolonged and severe hypernatremia, increasing the risk of serious complications such as seizures, thrombosis, intracranial hemorrhage, metabolic acidosis, acute kidney injury (AKI) and disseminated intravascular coagulation [1-11]. These complications are directly associated with hypernatremia and its treatment, and the severity of the symptoms does not correlate with blood osmolarity [1,2].
The management of HD involves identifying and addressing the underlying cause, as well as administering intravenous fluids to correct sodium levels.
This correction should occur at a controlled rate of 0.5-0.6 mEq/L per hour, aiming to prevent complications from a rapid decrease in sodium levels, particularly cerebral edema [1-3].
Despite the potential for severe consequences, most newborns recover fully without any lasting effects [1-3,9].
The authors have presented a case report of a newborn with severe HD. This report was previously showcased as an abstract at the 2021 European Academy of Pediatrics Meeting on April 25, 2021.
## II. CASE PRESENTATION
A 12-day-old female newborn was referred by her family doctor to the Emergency Room due to significant weight loss and decreased urination. The infant was delivered at 39 weeks via cesarean section because of a pelvic presentation and the Apgar score was 9/10. Maternal serological tests showed negative results, and all prenatal ultrasounds reported normal findings.
At birth, the newborn weighed 2800 grams (15th percentile; $-2< z$ -score $< 0$ ) and measured 46 centimeters in length (3rd-15th percentile; $-2< z$ -score $< 0$ ). Since delivery, she had been exclusively breastfed every two hours, exhibiting satisfactory suction reflexes and tolerance (the newborn was discharged home at the age of two days).
During the ER assessment, the newborn's weight was measured at 1940 grams, indicating a $30\%$ weight loss compared to birth weight. She was emaciated, jaundiced and had sunken eyes (refer to Figure 1) and fontanelle. Capillary refill time was 3 seconds, heart rate was 123 bpm, blood pressure was immeasurable, and capillary blood glucose levels measured $96~\mathrm{mg / dL}$. A saline bolus $(10~\mathrm{mL / kg})$ was administered with a good response in blood pressure. The newborn also appeared less responsive, with weak crying and mild global hypotonia; the remainder of the neurological examination was ordinary.
Venous blood gas analysis displayed the following values: pH 7.39, lactate 4.3 mmol/L, HCO3-21.8 mmol/L, and Na+ 180 mEq/L. Following HD's approach guidelines, intravenous treatment for dehydration was initiated. Laboratory results indicated a normal blood count, with Na+ levels 178 mEq/L, K+ 4.5 mEq/L, Cl- 143 mEq/L, urea 191 mg/dL, creatinine 1.39 mg/dL, and C-reactive protein 1.45 mg/dL. The coagulation study yielded average results. Both blood and urine cultures returned negative results.
The protocol implemented to address the newborn's hypernatremia ensured a gradual reduction in sodium levels, aiming for a decrease of $0.5 - 0.6 \, \text{mEq/L}$ per hour. This process necessitated the adjustment of fluid infusion rates according to sodium levels, which were monitored every one to two hours during the initial phase of treatment. The infant remained stable, exhibiting a gradual normalization of analytical parameters, achieving complete sodium level normalization 60 hours after admission. Throughout the treatment period, formula milk was introduced and adjusted per newborn's tolerance.
An encephalic ultrasound was conducted to rule out any potential brain damage resulting from hypernatremia and its treatment, which revealed no abnormalities.
After a seven-day hospital stay, the newborn was discharged and continued follow-up care, showing positive weight gain and normal neurodevelopment.
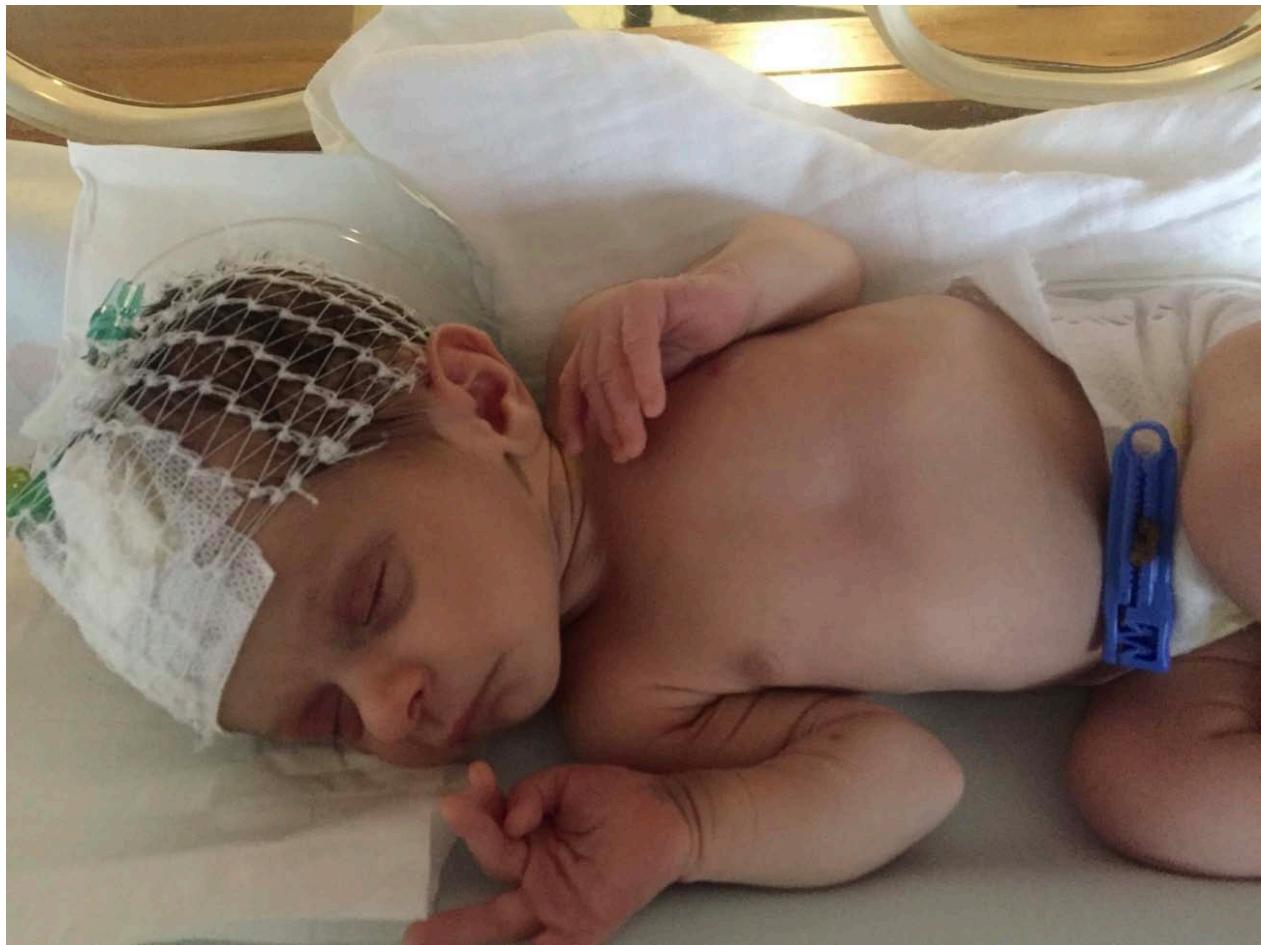 Figure 1: Newborn with hypernatremic dehydration. Physical examination shows an emaciated appearance, jaundice, sunken eyes and skin turgor.
## III. DISCUSSION
HD is a severe condition defined by elevated sodium levels above 145-150 mEq/L, often stemming from excessive fluid loss or inadequate fluid intake, with the latter being a prevalent cause in neonates. While it occurs more frequently in premature infants due to feeding immaturity, it can also affect full-term healthy newborns, mainly due to breastfeeding issues in the initial weeks of life [1-3,5-7,9-11]. In our case, the newborn exhibited unmistakable signs of dehydration linked to insufficient milk intake, notably a $30\%$ decrease in birth weight and a skeletal appearance. The likely cause for breastfeeding failure was inadequate support provided to the mother, compounded by limited guidance during the prevailing pandemic, where the mother did not receive adequate support from both family and healthcare providers. This situation allowed inadequate breastfeeding to persist until the first appointment for the newborn, which, within the Portuguese national healthcare system, can take place up to the fifteenth day of life.
Several risk factors for HD exist, including cesarean delivery, primiparity, breast anomalies, excessive pre-pregnancy maternal weight, delayed initiation of the first breastfeeding, and lack of prior breastfeeding experience [3,4,6]. In the case described, the mother was a primipara and had no previous experience or knowledge about breastfeeding. Additionally, the newborn was delivered via cesarean section.
Neonates with HD often present well, as classic signs of dehydration, such as sunken eyes and depressed fontanelles, may not be initially evident. Parents may misinterpret certain signs, like the lack of crying or prolonged sleep, as indicators of satiety, leading to a delayed diagnosis [2,4,8-9]. Initial signs of HD are subtle and nonspecific, like lethargy, agitation, and irritability, progressing to severe symptoms including seizures, coma, and potentially death [1-5,8-9]. In our case, the parents perceived prolonged sleep and rare crying as positive signs, assuming the child's well-being.
The diagnosis of HD is typically incidental during newborn weight checks, revealing a weight loss higher than $10\%$ compared to birth weight, prompting comprehensive evaluation, including medical history, physical examination, and blood tests [1,2,5,7,11]. In our case, the family doctor immediately referred the infant to the ER upon finding a $30\%$ weight loss for further investigation and treatment.
Treating HD involves identifying and addressing the underlying cause while administering intravenous fluids to restore sodium levels to normal values. The challenge lies in preventing rapid sodium level decreases, which can lead to severe problems such as intracranial hemorrhage, thrombosis, and cerebral edema, particularly within the first 24 hours of dehydration [1,2,5-7,10-11]. Sodium correction might take up to 48 hours or more, maintaining a decrease rate of $15\mathrm{mEq/L}$ in 24 hours or $0.5 - 0.6\mathrm{mEq/L}$ per hour [1-4,6-7]. In mild cases (sodium values below $160\mathrm{mEq/L}$ ), the infant may be given oral feeds at 1.5 times the maintenance with breast milk or formula milk [3,11]. For more severe cases, the fluid choice depends on the sodium level, aiming to prevent rapid changes. If the sodium levels are higher than $170\mathrm{mEq/L}$, a customized solution aligning with the patient's osmolarity is recommended to avoid complications [1,2,5-7,9]. Regular monitoring and adjusted infusion rates prevented complications, resulting in normalized sodium levels 60 hours after admission with no evidence of cerebral edema.
While higher mortality rates are associated with sodium levels exceeding 160 mmol/L, newborns with HD typically make a full recovery without sequelae [2,3,8]. Indeed, in a cross-sectional study involving 46 infants diagnosed with HD, none exhibited central nervous system complications. Approximately half of the participants presented with AKI upon admission, which subsequently resolved entirely [3]. In a separate study encompassing 65 infants diagnosed with HD, over $12\%$ of the neonates developed intracranial hemorrhage, while $12.8\%$ experienced cerebral edema [8]. In our particular case, the newborn presented with AKI, which was resolved through appropriate correction of dehydration. Subsequently, the newborn showed complete recovery without cerebral complications, evidenced in follow-up appointments with normal encephalic ultrasounds and adequate psychomotor development.
It is crucial to maintain close follow-up in newborns who are exclusively breastfed to ensure adequate milk intake and to avoid serious conditions such as the one presented.
## IV. CONCLUSIONS
HD carries the potential for significant complications, such as intracranial hemorrhage and disseminated intravascular coagulation. The primary recognized risk factor for HD is inadequate milk intake, primarily stemming from ineffective lactation and insufficient knowledge about breastfeeding practices.
Therefore, this case report draws attention to the severe consequences resulting from breastfeeding failure, underscoring the critical need to educate and support mothers in breastfeeding. Providing ample guidance and information on breastfeeding techniques, healthy practices, and identifying signs of breastfeeding failure is imperative for successful breastfeeding. Additionally, emphasizing the necessity for close monitoring of newborns during the initial weeks of life through regular weight assessments and comprehensive physical examinations is essential to detect and manage conditions like HD promptly.
The benefits of breastfeeding are extensive and irreplaceable. Hence, breastfeeding promotion is crucial, requiring adequate support and guidance for mothers throughout this process.
Disclosures
Informed consent was obtained for the use of the newborn's photo.
The authors don't have any conflict of interest to declare.
Generating HTML Viewer...
References
11 Cites in Article
Naveed Durrani,Abubakr Imam,Naharmal Soni (2022). Hypernatremia in Newborns: A Practical Approach to Management.
V Sousa,C Carrusca,M Santos (2016). Desidratação hipernatrémica no recém-nascido.
Apoorv Saxena,Suprita Kalra,Subhash Shaw,K Venkatnarayan,Amit Sood,V Tewari,Rakesh Gupta (2020). Correction of hypernatremic dehydration in neonates with supervised breast-feeding: A cross-sectional observational study.
Christie Del Castillo-Hegyi,Jennifer Achilles,B Segrave-Daly,Lynnette Hafken (2022). Fatal Hypernatremic Dehydration in a Term Exclusively Breastfed Newborn.
Ashish Jain,Nidhi Jain (2019). OSCE: Management of hypernatremic dehydration in neonates.
Mohammed Zayed,Sarah Gadim,Omer Magzoub (2023). Common Clinical Presentation and Associated Laboratory Findings of Neonatal Hypernatremia.
Fatih Bolat,Mehmet Oflaz,Ahmet Güven,Göktuğ Özdemir,Demet Alaygut,Melih Doğan,Füsun İçağasoğlu,Ömer Cevit,Asm Gültekin (2013). What Is the Safe Approach for Neonatal Hypernatremic Dehydration?.
Hassan Boskabadi,Javad Akhondian,Maliheh Afarideh,Gholamali Maamouri,Sepideh Bagheri,Seyyed Parizadeh,Majid Mobarhan,Shabnam Mohammadi,Gordon Frens (2017). Long-Term Neurodevelopmental Outcome of Neonates with Hypernatremic Dehydration.
I Laing,C Wong (2002). Hypernatraemia in the first few days: is the incidence rising?.
B Butler,H Trotman (2021). Hypernatremic Dehydration in Breast Fed Infants: Lessons from a Baby-Friendly Hospital.
Nilofer Mujawar,Archana Jaiswal (2017). Hypernatremia in the neonate: Neonatal hypernatremia and hypernatremic dehydration in neonates receiving exclusive breastfeeding.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
Aida Azevedo. 2026. \u201cSevere Hypernatremic Dehydration in a Neonate\u201d. Global Journal of Medical Research - F: Diseases GJMR-F Volume 23 (GJMR Volume 23 Issue F10): .
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.