Congenital Insensitivity to Pain with Anhidrosis (CIPA) is a rare hereditary condition that affects the nervous system, leading to an absence of pain sensation and impaired thermal regulation. This case report highlights the diagnostic process of a 9-year-old patient suspected to be suffering with CIPA in a dental setting where early recognition of the condition plays a critical role in preventing complications. The report discusses the implications of CIPA for pediatric dental care, emphasising the need for increased awareness and modified management approaches.
## I. INTRODUCTION
Congenital Insensitivity to Pain with Anhidrosis (CIPA) is classified under Hereditary Sensory and Autonomic Neuropathies (HSAN Type IV). Due to a mutation in the NTRK1 gene, affected individuals are unable to feel pain or temperature, leading to frequent self-injuries, delayed wound healing and other complications.
While CIPA has been widely studied in medical literature, its impact in pediatric dentistry is not well documented. In dentistry, the absence of pain can mask serious oral conditions, posing a significant challenge for diagnosis and management. CIPA is an exceedingly rare disorder, with a reported incidence of one in 125 million[1]. The disease shows geographic variability, which may be attributed to founder mutations and consanguineous marriages[2]. The condition exhibits an autosomal recessive inheritance pattern, necessitating the presence of two mutated alleles for phenotypic expression[3]. The majority of affected individuals originate from consanguineous unions, emphasizing the importance of genetic counseling in at-risk populations. There is no reported study about the gender predilection of this disease particularly.
CIPA is characterized mainly by 3 symptoms: pain, anhidrosis and temperature. Notably, lacrimation, salivation, and touch perception are unaffected. Due to their lack of pain perception, affected persons are more vulnerable to infections and self-inflicted injuries, such as intraoral injuries. The inability to sweat is a contributing factor to anhidrosis, which raises the risk of hyperthermia. A nerve biopsy, genetic testing, and clinical assessment all contribute to the diagnosis. To detect the precise mutation and validate the diagnosis,
NTRK1 gene genetic analysis is required.[4] This case report focuses on the identification of CIPA in a 9-year-old patient and its implications for pediatric dental practice.
## II. CASE REPORT
### a) Patient Information
A 9-year-old male was brought to the Department of Pediatric and Preventive Dentistry in Seema Dental college & Hospital, Rishikesh, for a routine dental check-up. The patient's medical history revealed no significant dental complaints, but the parents reported frequent self-injuries and an inability to perceive pain since birth. According to his mother the patient would inflict self-injuries using hot iron rods or would sit on top of the fire and get burns but won't feel any pain. Based on clinical history, the patient was suspected to be suffering from a very rare condition known as congenital insensitivity to pain with anhidrosis (Table 1). The patient belonged to low socio economic background therefore his parents never bothered to undergo any kind of investigation for his medical condition.
### b) Clinical Presentation
Upon extraoral examination, the patient displayed several healed scars on the extremities and head, likely resulting from repeated self-inflicted injuries as shown in Figure 1(a). Despite the presence of noticeable injuries, the patient exhibited no signs of discomfort.
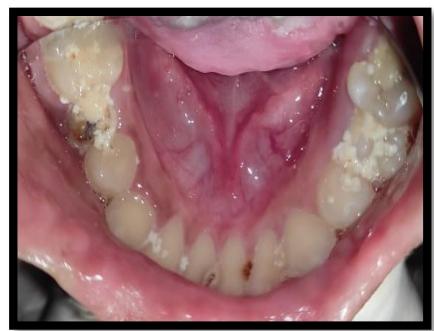
Intraoral examination revealed generalized attrition of teeth, early carious lesions in the posterior teeth with no complaints of sensitivity or pain, multiple areas of soft tissue scarring on the inner lips and buccal mucosa, no other visible pathologies or acute dental issues were noted as shown in Figure 2.
The patient did not respond to any pain stimuli during the examination, confirming the clinical signs of CIPA. Radiographic imaging was performed, which showed deep carious lesions with periapical radiolucency as shown in Figure 3. The diagnosis made was deep carious lesion with periapical abscess w.r.t 46.
### c) Diagnostic Process
The diagnostic process is based on clinical evaluation, genetic testing, and a nerve biopsy. Genetic analysis of the NTRK1 gene is essential for confirming the diagnosis and identifying the specific mutation.[6] The mother used to work at AllMS Rishikesh as a cleaning staff and she mentioned that she had consulted a neurologist about the condition once and she was told that it might be due to neurological problems. No further investigation of any kind was done. Given the patient's unique presentation and the reported medical history and comparing it with other similar neuropathies, CIPA was suspected as the underlying condition. While the patient did not present with any immediate dental concerns, the absence of pain posed challenges in evaluating the true extent of oral damage. Routine dental tests, such as percussion or sensitivity testing, were not applicable, necessitating a more cautious approach in future monitoring.
### d) Management
No immediate treatment was provided during this visit. The focus remained on educating the parents regarding the long-term implications of CIPA on oral health. Preventive dental care, regular check-ups, and close monitoring were strongly recommended. Customized preventive strategies, including the use of mouthguards and improved oral hygiene practices, were discussed to minimize the risk of self-inflicted injuries in the future. Since the mother was a labor moving from place to place in search for work, the patient didn't turn up for further treatment.
## III. DISCUSSION
CIPA presents a unique diagnostic challenge in pediatric dentistry due to the patient's inability to experience pain. In a typical dental scenario, pain acts as a key indicator for diagnosing conditions such as caries, pulpitis, or infections.[6] However, in patients with CIPA, dental practitioners must rely on visual and radiographic cues rather than patient-reported symptoms, potentially delaying the diagnosis of critical conditions. Although this syndrome can be diagnosed by clinical and paraclinical tests together, but a confirmatory genetic test is better to fully understand the disease.[3] In this case the child was first suspected to be victim of child abuse and neglect as it can be easily confused for child abuse as described by Yagev et al.[8] After thorough conversation with the child and his mother as well his sister individually it was found out that the child has masochistic habits. Upon further conversation it was found out that the child doesn't feel any pain.
Pediatric dentists should be aware of the increased risk of oral trauma, caries progression, and periodontal disease in these patients, as they often go unnoticed without the protective mechanism of pain. In a case presented by Kouvelas N et al. parents gave a history of self-extraction of the teeth as the child did not feel any pain.[1] Additionally, these patients may develop severe infections or complications if oral conditions are left untreated. Caregivers should be informed about maintaining meticulous oral hygiene, frequent dental visits, and injury prevention techniques.
The case also highlights the need for a multidisciplinary approach, involving pediatricians, neurologists, and dentists, to ensure comprehensive care. We suggest psychological interventions for CIPA primarily focusing on patient education, coping mechanisms development and emotional support to help individuals understand their condition, learn strategies to prevent injuries and manage psychological impact of not experiencing pain, including anxiety related to potential harm and social challenges arising from their unique situation. In a similar case presented by Neves BG et al, they reported that it is important to include a dentist in the multidisciplinary team to reduce the frequency and severity of the self-inflicted lesions in these patients.[9] Early diagnosis of CIPA in a dental setting can prevent severe complications, contributing to better long-term outcomes for the patient. At an early age and with parent's cooperation, the use of a nightguard, grinding sharp edges of the teeth, or the addition of a composite are helpful; rather than the performance of a full mouth extraction which is an extremely radical treatment that causes bone loss.[10]
The management of these individuals is quite challenging, and there is little information in dentistry literature about this problem. Unrecognizing of the clinical pictures of CIPA and minimal literature references in the past, misleads to late diagnosis and management.[11]
### a) Significance in Pediatric Dentistry
CIPA significantly alters the approach to pediatric dental care. Key considerations include:
- Preventive Focus: Regular dental visits should be scheduled to monitor oral health since patients will not report symptoms of pain.
- Education: Educating caregivers about injury prevention and the importance of maintaining oral health is crucial in preventing self-inflicted damage and infections.
- Modified Treatment: Treatment approaches must be adjusted, focusing on visual diagnostics rather than patient-reported symptoms. Pain management strategies should be carefully considered due to the patient's lack of pain perception.
A rubber dam should always be used to avoid any serious iatrogenic injuries since the patient is unable to feel any pain and wouldnot be able to report about the same.
- Team Approach: A collaborative approach between dental and medical professionals is essential to ensure the patient's overall well-being.
## IV. CONCLUSION
CIPA is a rare condition with profound implications for pediatric dental care. Although no immediate dental treatment was required for the 9-year-old patient in this case, the diagnosis emphasizes the need for a specialized approach to oral care. Pediatric dentists must be vigilant and proactive in identifying and managing such cases to prevent complications and maintain oral health in the absence of pain as a diagnostic tool.
 (a)
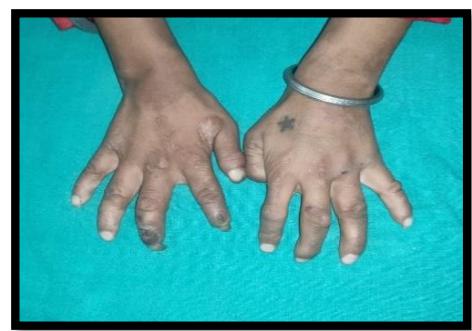 (b)
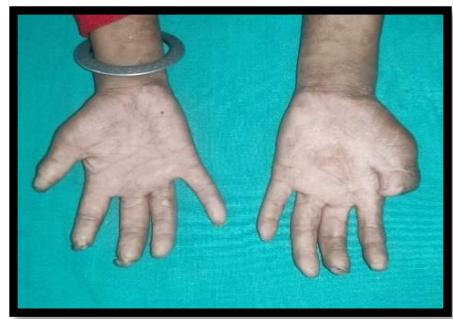
 (c)
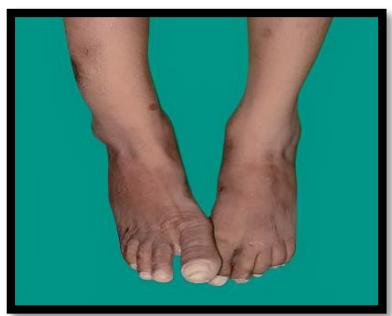
 (d)
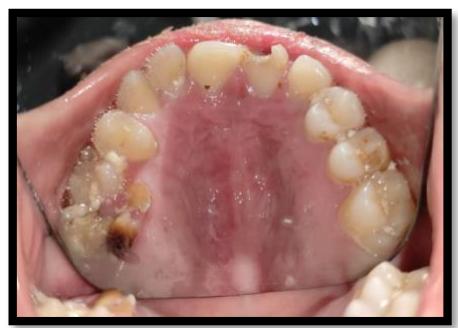 Figure 1: (a) Healing scars on face, (b&c) Foreshortening of distal phalanges of hand (d) Multiple burn scars on leg (a)
 (b)
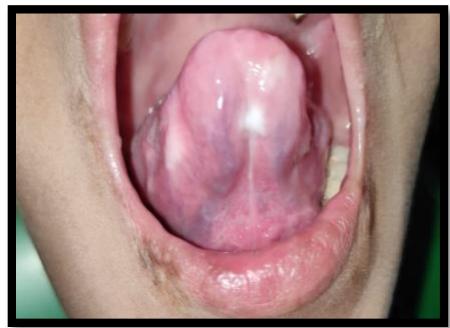
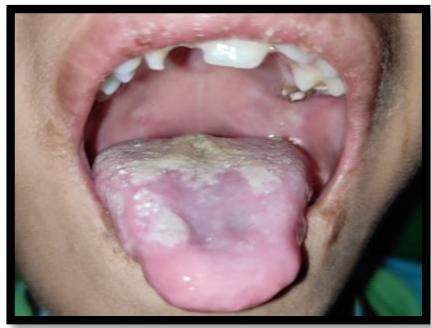 Figure 2: Intraoral examination (a&b) Multiple carious teeth, poor oral hygiene, (c&d) Diffused whitish mucosal lesions seen on the dorsal and ventral aspect of tongue, Labial soft tissue deformity of the patient due to biting
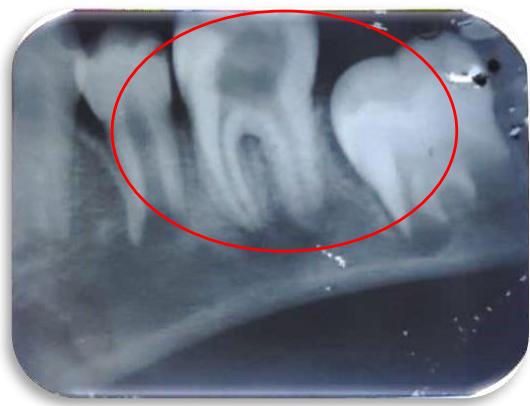 Figure 3: Radiolucency involving enamel, dentin and pulp, loss of lamina dura in mesial and distal root, diffused periapical radiolucency with mesial and distal root i.r.t 46
Generating HTML Viewer...
References
11 Cites in Article
K Daneshjou,H Jafarieh,S Raaeskarami,B Khaled,M Alzahayqa,A Jaffal (2023). 2. Identification of founder and novel mutations that cause congenital insensitivity to pain (CIP) in palestinian patients.
(2007). Hereditary sensory and autonomic neuropathies: types II, III, and IV. Axelrod FB, Gold-von Simson G.
N Kouvelas,C Terzoglou (1989). Congenital insensitivity to pain with anhidrosis: case report.
Seung‐tae Lee,Jeehun Lee,Munhyang Lee,Jong‐won Kim,Chang‐seok Ki (2009). Clinical and genetic analysis of Korean patients with congenital insensitivity to pain with anhidrosis.
Seung‐tae Lee,Jeehun Lee,Munhyang Lee,Jong‐won Kim,Chang‐seok Ki (2009). Clinical and genetic analysis of Korean patients with congenital insensitivity to pain with anhidrosis.
T Erdem,I Ozcan,D Ilguy,S Sirin (2000). Case report hereditary sensory and autonomic neuropathy: review and a case report with dental implications.
K Daneshjou,H Jafarieh,S Raaeskarami (2012). Congenital insensitivity to pain and anhydrosis (CIPA) syndrome; a report of 4 cases.
R Yagev,J Levy,Z Shorer,T Lifshitz (1999). Congenital insensitivity to pain with anhidrosis: ocular and systemic manifestations.
B Neves,R Roza,G Castro (2009). Traumatic lesions from congenital insensitivity to pain with anhidrosis in a pediatric patient: dental management.
A Safari,A Khaledi,M Vojdani (2011). Congenital Insensitivity to Pain with Anhidrosis (CIPA) Manifested with Chronic Osteomyelitis; A Case Report.
F Hartono,C Tanjung,K Besinga,D Marpaung,T Ananditya,A Budisantoso (2020). Catastrophic results due to unrecognizing of congenital insensitivity to pain with anhidrosis in children with multiple long bones fractures: A case report of 27 years follow-up of two siblings.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
Dr Kalpna Chaudhry. 2026. \u201cThe Silent Sufferers: Congenital Insensitivity to Pain with Anhidrosis (CIPA): A Case Report\u201d. Global Journal of Medical Research - J: Dentistry & Otolaryngology GJMR-J Volume 25 (GJMR Volume 25 Issue J1).
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.