Globally, there have been attempts towards improving the coverage of malaria preventive measures with the 2015 goal of the World Health Organization’s (WHO’s) Roll Back Malaria Partnership centered to reduce global malaria cases by 75% and to reduce malaria deaths to near zero through universal coverage by effective prevention and treatment interventions. Regrettably, malaria still constitutes a serious public health problem in Nigeria. The aim of this study was to assess long lasting insecticide treated net use among women of child bearing age in Nwangele LGA Imo State. A community based descriptive cross sectional study was used for the study. The study involved women of child bearing age aged 15-45yrs at Nwangele LGA as its Target Population. A Probability based multi stage sampling method was adopted for the study. A semi-structured questionnaire was used as the instrument of data collection for this study and Statistical Package for the Social Sciences (SPSS) was used in the analysis of the data gotten from the study. A total of 404 women participated in the study.
## I. INTRODUCTION
According to a publication by center for Disease Control (2014), malaria infection is caused by a protozoan (Plasmodiae). However the report posited that malaria infection occurs when favorable environmental conditions of temperature, rainfall, and humidity are created for the female Anopheles mosquitoes, carrying the Plasmodium, to bite a susceptible host (CDC, 2014). Malaria infection is endemic in Nigeria, with a prevalence of 919 per 10,000 of population; it remains one of the leading causes of morbidity and mortality (Ganihu & Jimo, 2013; Oche et al., 2011; Aribodor et al., 2017) It accounts for seven out of ten outpatient visits in Nigerian hospitals as well as being responsible for about $20\%$ and $30\%$ of infant and under-5 mortality rate, respectively (Oche et al., 2011).
Following the attempts towards improving the coverage of malaria preventive measures, the 2015 goal of the World Health Organization's (WHO's) Roll Back Malaria Partnership are to reduce global malaria cases by $75\%$ and to reduce malaria deaths to near zero through universal coverage by effective prevention and treatment interventions (RBM, 2010). Among other preventive interventions, WHO recommends the use of insecticide treated nets (ITNs), particularly Long-Lasting Insecticide Nets, which have been shown to be cost-effective, to reduce malaria episodes among children under 5 years of age by approximately $50\%$ and all-cause mortality by $17\%$. Universal coverage with ITNs is defined as use by $>80\%$ of individuals in populations at risk (WHO, 2019; RBM, 2010).
Aribodor et al. (2017) in a report posited that the usage of long lasting insecticide treated nets is largely affected by distribution patterns and also the knowledge of people and their perception about it. Behavioral patterns of people-utilization of the LLITNs are dependent on their socio demographic characteristics on the consequence of nonuse (Aina and Ayeni, 2011; Mbanugo and Okorudo, 2015; Aribodor et al., 2017). Researchers give varied indications on the coverage and use of the LLITNs in various parts of the World and peoples level of knowledge it (Runsewe-Abiodun et al., 2012; Aluko & Oluwatosin, 2012; Iwu et al., 2010: Aina and Ayeni, 2011: Ganihu & Jimo, 2013). Isah and Nwobodo (2009) reported that despite evidence that the use of LLITNs decreases malaria-related morbidity and mortality, the use of LLITNs in Africa remains relatively low. Estimates suggest that in 2005, only $3\%$ of children under five years of age slept under LLITNs, while up to ten times as many are thought to sleep under any bed net (Baley & Deressa, 2008). This shows that the fact that ITNs are very effective in malaria prevention does not necessarily mean that people will use them after they have received those (Baley & Deressa, 2008). While the evidence based on the effectiveness of LLITNs in reducing malaria transmission has grown rapidly in recent years, utilization rates of LLITNs in most African countries have been very low (Chukwuocha et al., 2010; Ganihu & Jimo, 2013). The renewed Abuja, Nigeria, target for roll back malaria (RBM), a control program for malaria, targeted $80.0\%$ of children $< 5$ years of age and pregnant women to use long lasting insecticide-treated mosquito nets (LLITN) between 2006 and 2010 (FMOH, 2015; (Deneye et al., 2011).
The millennium development goal 6 has a target of halting and beginning to reverse the incidence of malaria in 2015 (Baley & Deressa, 2008). These control programs are aimed at reducing the morbidity and mortality, resulting from malaria infections in at-risk groups particularly at Households. The past decades have witnessed an increase in international funding for malaria control. This increased funding has led to an increase in accessing LLITNs in Sub-Saharan Africa (Deneye et al., 2011). At the end of 2010, approximately 289 million LLITNs were delivered to the Several Households at Sub-Saharan African region; this is enough to take care of $76\%$ of the 765 million persons at risk (Deneyeet et al., 2011). Insecticide Treated Nets is currently one of the most cost-effective options for reducing malaria-related morbidity and mortality and has been reported to reduce malaria mortality by $17\%$ in children $< 5$ years of age (Runsewe-Abiodun et al., 2012).
Regrettably, malaria still constitutes a serious public health problem in Nigeria (Aina and Ayeni, 2011; Mbanugo and Okorado, 2015; Aribodor et al., 2017). Malaria is endemic in the poorest countries in the world, causing 400 to 900 million clinical cases and up to 2.7 million deaths each year (Guyatt & Ochola, 2014). More than $90\%$ of malaria deaths occur in Sub-Saharan
Africa, resulting in an estimated 3,000 deaths each day. Almost all the deaths are among high-risk groups including women of childbearing age, women during pregnancy, non immune travelers, refugees and other displaced persons, and people of all ages living in Household areas of unstable malaria transmission (Mbanugo & Okorado, 2015; Iwu et al., 2010: Aina & Ayeni, 2011: Ganihu & Jimo, 2013). In highly endemic countries, malaria poses a serious danger to women of child bearing age, women in pregnancy and their unborn children (Mbanugo & Okorado, 2015). Malaria in pregnancy causes maternal anaemia, miscarriage, and low birth weight. In endemic countries, it is the leading cause of maternal mortality and one of the primary causes of neonatal deaths (Mbanugo & Okorado, 2015).
According to some reports in Nigeria, malaria is the leading cause of Maternal Mobility contributing $33\%$ of deaths among women of child bearing age and $25\%$ infant mortality (Oche et al., 2011; Iwu et al., 2010). These Problems resulting due to minimal preventive measures especially in poor sub Saharan African regions like Nigeria which include low utility of LLITNs and poor sanitary conditions at Household and residential areas remain an issue of concern and a problem. Despite these interventions, women of child bearing age have reported gaps in uptake noting that LLITNs are effective in the prevention of malaria, ITN coverage and utilization still remain low in Nigeria with few studies have documented household net coverage and utilization in Nigeria (Aina and Ayeni, 2011; Mbanugo and Okorado, 2015; Aribodor et al., 2017). Most of the published studies available were conducted in other malaria endemic countries in Sub-Saharan Africa and the few published studies in Nigeria were from the urban centers of other states. With women of childbearing age being at significant risk, it is imperative to examine this coverage of long lasting Insecticide treated nets in Nwangele. However, it is due to the magnitude of the problem that the researcher aims to find out Long Lasting Insecticide Treated Nets use among women of child bearing age in Nwangele LGA, Imo state South Eastern Nigeria.
## II. METHODS
### a) Design
A community based descriptive cross sectional study was used for the study to determine Long Lasting Insecticide Treated Nets among women of child bearing age in Nwangele LGA.
### b) Study Setting
Nwangele is a Local Government Area of Imo State, Nigeria. Its headquarters are in the town of Amaigbo. Nwangele Local Government is administered under the terms of the Constitution of the Federal Republic of Nigeria. Imo State it is located at the central part of Amaigbo and it is made up of 11 villages comprising of Amaigbo Community, Abba Community, Dimnanume community, Isu Ancient Kingdom Community, Umuozu Community, Isiala Umuozu Community, Umunakara Community, Umudurunna Community, Abajah Community, Ogwuaga/Ekitiafor Community and Umunna Community. The urban towns of Nwangele L.G.A. are Abajah, Isu, Amaigbo, Umuozu and Abah, the rest are more of rural towns. Going by the 2006 census, the population of Nwangele L.G.A. was 127,691 people divided as Male 65022, Female 62669 (National Population Commission, 2006). Nwangele Local Government Area Constitutes mainly of lgbo people situated in her Residential territories as well as other minor ethnicities. It has an area of $295\mathrm{km}^2$ and a population of 99,265 at the 2006 census The Coordinates of Nwangele Local Government Area is given as $5.4166^{\circ}\mathrm{N}$, $6.9853^{\circ}\mathrm{E}$.
### c) Study Population
This study on Long Lasting Insecticide Treated Nets among women of child bearing age in Nwangele LGA involved women of child bearing age aged 15-45yrs at Nwangele LGA as its Target Population
### d) Inclusion criteria
The study included the following i. Women of child bearing age at Nwangele LGA who gave in their consent for the study.
ii. Women of child bearing age at Nwangele LGA who are adults aged 18-45years present as at the time of data collection.
### e) Exclusion criteria
The study excluded the following;
i. Women of child bearing age who refused to give in their consent for the study ii. Women of child bearing age who were lunatic, sick or disabled during the time of data collection.
### f) Sampling
## i. Sample size Calculation
The sample size was determined using the Yamene formula (1967) for sample size determination.
$$
\mathrm {n =} \quad \frac {\mathrm {N _ {-}}}{1 + \mathrm {N e ^ {2}}}
$$
Where:
n is the desired sample size
N is the population size (12,389) = population of women of childbearing age at Nwangele LGA (NPC, 2010).
e is margin of error (0.05)
Therefore,
$$
n = 3 9 2. 3 0 3 6 2 2 1 0
$$
Furthermore, to adjust for a $10\%$ rate of non response and invalid response (i.e $90\%$ expected response rate $= 0.9$ ).
n = n/expected response rate
$$
n = 3 9 2 / 0. 9 0 = 4 3 5. 5
$$
$$
n = 4 3 6
$$
## ii. Sampling Methods
A Probability based multi stage sampling method was adopted for the study on the coverage of Long Lasting Insecticide Treated Nets among women of child bearing age in Nwangele LGA.
First stage-Selection of Communities: A total of Three (3) Out of the communities in Nwangele LGA was selected by the researcher using simple random sampling via balloting to give every community an equal chance of selection. Second stage- Selection of villages: Three (2) villages each out of the total number of villages in the selected community was selected via simple random sampling using balloting giving every village in the selected community an equal chance of being selected. Third stage- Selection of Streets: A total of Five (5) streets each in the selected Six (6) villages were selected via simple random sampling (balloting) to give every street an equal chance of being selected. Fourth stage: Selection of households: A systematic probability sampling method was used to select each household in the selected streets giving each household an equal chance of selection. Fifth stage: Selection of Respondents: the researcher selected women of child bearing age in each household or any one present at the time of study. Selection of respondents was done via simple random sampling.
### g) Instrument for data collection
A semi-structured questionnaire was used as the instrument of data collection for this study on the coverage of Long Lasting Insecticide Treated Nets among women of child bearing age in Nwangele LGA.
### h) Validity of the instrument
### i) Reliability of Instrument
The Reliability of the instrument of data collection was determined using test retest method. Copies of the questionnaire were given to some respondents outside the area of study by the researcher. This area shared similar characteristics with Nwangele LGA that was used for this study. Chrombach alpha test was used to test for the reliability of the questionnaire to determine the consistency of the results with a reliability coefficient of 0.8 obtained.
### j) Method of Data Collection
Data was obtained using an interviewer based semi structured questionnaire. This will be done with the aid of Two (2) field assistants who will be hired and trained to aid the researcher in the data collection process.
### k) Method of Data Analysis
The Statistical Package for the Social Sciences (SPSS) was used in the analysis of the data gotten from the study. Results will be expressed in percentages, frequencies, tables and charts (Descriptive Statistics). Chi square was used to test the hypothesis statement of the study $(p = 0.05)$.
Ethical Consideration
A letter of introduction and ethical clearance was obtained from the School of Postgraduate studies Ethical clearance committee in Federal University of Technology Owerri (FUTO) before the research was conducted. The purpose of the research was explained to each respondent and verbal informed consent obtained from them before inclusion into the study. Also, anonymity of the respondents was assured and ensured. The confidentiality of the information they gave was also maintained.
## III. RESULTS
A total of four hundred and thirty six (436) copies of questionnaires were distributed for the study. They were properly filled and crosschecked for correctness, and 404 questionnaires were retrieved and were used for the purpose of the analysis.
### a) Socio Demographic Factors of the Respondents
From the table 1 below, $41.5\%$ (169) of the respondents were aged between 26-30 years, $20.5\%$
(83) between ages 15-20, $9.9\%$ (40) were people in their early 20's (21-25), $14.3\%$ (58) were between 31-40 years of age and $13.3\%$ (54) were adults within 41-45 year age bracket. On ethnicity, $38.1\%$ (154) opted for ethnic groups not listed but label 'others', $93.7\%$ (379) were of the Igbo ethnic group, $1.9\%$ (8) Yoruba, and $0.4\%$ (2) of the respondents were Hausa/Fulani. On educational backgrounds, $30.9\%$ (125) of the respondents had Informal education, $12.8\%$ (52) had attained the Tertiary level of Education, and $22.2\%$ (90) had primary education and $37.1\%$ (150) of the respondents with secondary level of education. $50.7\%$ (205) of the respondents did occupations not listed but label 'others', $17.3\%$ (70) were civil servants, $18.8\%$ (76) of the respondents housewives while just $13.1\%$ (53) were self employed. On the marital status of the respondents, $26.2\%$ (106) were widowed, $24.7\%$ (100) were single, $24.5\%$ (99) married while $12.6\%$ (51) of the respondents were separated. $11.8\%$ (48) opted to choose 'others'. $27.2\%$ (110) of the respondents had an income level between 1-10,000, $21.7\%$ (88) had an income level between 31,000-50,000, $20.2\%$ (82) earned above 100,000, $17.0\%$ (69) had an income level between 11,000-30,000, and the least percentage $13.6\%$ (55) earned an income between 51,000-100,000.
Table 1: Socio Demographic Factors of the Respondents
<table><tr><td>Characteristics</td><td>Frequency (n=404)</td><td>Percentage (%)</td></tr><tr><td>Age</td><td></td><td></td></tr><tr><td>15-20</td><td>83</td><td>20.5%</td></tr><tr><td>21-25</td><td>40</td><td>9.9%</td></tr><tr><td>26-30</td><td>169</td><td>41.5%</td></tr><tr><td>31-40</td><td>58</td><td>14.3%</td></tr><tr><td>41-45</td><td>54</td><td>13.3%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Ethnicity</td><td></td><td></td></tr><tr><td>Igbo</td><td>379</td><td>93.8%</td></tr><tr><td>Hausa/Fulani</td><td>2</td><td>0.4%</td></tr><tr><td>Yoruba</td><td>8</td><td>1.9%</td></tr><tr><td>Others</td><td>15</td><td>3.7%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Educational level</td><td></td><td></td></tr><tr><td>Informal education</td><td>52</td><td>12.8%</td></tr><tr><td>Primary</td><td>90</td><td>22.2%</td></tr><tr><td>Secondary</td><td>150</td><td>37.1%</td></tr><tr><td>Tertiary</td><td>112</td><td>27.7%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Occupation</td><td></td><td></td></tr><tr><td>Self employed</td><td>53</td><td>13.1%</td></tr><tr><td>House wife</td><td>76</td><td>18.8%</td></tr><tr><td>Civil servant</td><td>70</td><td>17.3%</td></tr><tr><td>Others</td><td>205</td><td>50.7%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Parity</td><td></td><td></td></tr><tr><td>None</td><td>92</td><td>22.7%</td></tr><tr><td>1-2</td><td>169</td><td>41.8%</td></tr><tr><td>3-5</td><td>40</td><td>9.9%</td></tr><tr><td>Above 5</td><td>103</td><td>25.4%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Marital status</td><td></td><td></td></tr><tr><td>Married</td><td>99</td><td>24.5%</td></tr><tr><td>Single</td><td>100</td><td>24.7%</td></tr><tr><td>Separated</td><td>51</td><td>12.6%</td></tr><tr><td>Widowed</td><td>106</td><td>26.2%</td></tr><tr><td>Others</td><td>48</td><td>11.8%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Income Level</td><td></td><td></td></tr><tr><td>1-10,000</td><td>110</td><td>27.2%</td></tr><tr><td>11,000-30,000</td><td>69</td><td>17.0%</td></tr><tr><td>31,000-50,000</td><td>88</td><td>21.7%</td></tr><tr><td>51,000-100,000</td><td>55</td><td>13.6%</td></tr><tr><td>Above 100,000</td><td>82</td><td>20.2%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr></table>
### b) Level of Knowledge of Long Lasting Insecticide-Treated Nets
Table 2 considering the level of knowledge of long lasting insecticide treated nets, a majority of the respondents with $96.5\%$ (390) said "Yes" when they were asked if they had heard about malaria at any time prior to the questionnaires, while a small $3.4\%$ (14) denied. When asked if they had suffered from malaria, a majority if the respondents also with $95.2\%$ (385) replied "Yes" while just $4.7\%$ (19) said "No". $61.6\%$ (249) of the respondents believe mosquito bites causes malaria, $26.2\%$ (106) said malaria is caused by dirt/stagnant water, $9.6\%$ (39) chose plasmodium organisms and $4.7\%$ (19) said "germs". Upon question on how malaria is transmitted, $44.0\%$ (178) opted to choose 'Bites of any
Mosquito', $19.0\%$ (77) said "Bites of insect which has bitten a malaria Patient", and $36.8\%$ (149) opted for 'Stagnant water and unclean environment'. $74.0\%$ (299) of the participants replied "Yes" when asked if they had heard about LLITNs, while $25.9\%$ (105) said "No". $24.2\%$ (98) had heard about LLTINs from Health centers, $15.3\%$ (62) from the Media, $17.3\%$ (70) from publications/journals, $18.5\%$ (75) chose options not listed but label 'others', $13.6\%$ (55) heard about LLTINs from school, while $10.8\%$ (44) from Family/Friends. Based on LLITNs is Key in Prevention of Malaria due to its Durability, $75.2\%$ (304) said "Yes", while $24.7\%$ (100) said "No". On if LLITNs is effective in the Prevention of Malaria when it is air dried frequently $73.7\%$ (298) replied "Yes" and $26.2\%$ (106) of the respondents said "No".
Table 2: Level of Knowledge of Long Lasting Insecticide-Treated Nets
<table><tr><td>Variables</td><td>Frequency (n=404)</td><td>Percentage (%)</td></tr><tr><td>Heard about Malaria</td><td></td><td></td></tr><tr><td>Yes</td><td>390</td><td>96.5%</td></tr><tr><td>No</td><td>14</td><td>3.4%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Have you Suffered from Malaria before</td><td></td><td></td></tr><tr><td>Yes</td><td>385</td><td>95.2%</td></tr><tr><td>No</td><td>19</td><td>4.7%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>What causes malaria</td><td></td><td></td></tr><tr><td>Germs</td><td>19</td><td>4.7%</td></tr><tr><td>Dirts/Stagnant Water</td><td>106</td><td>26.2%</td></tr><tr><td>Mosquito Bites</td><td>249</td><td>61.6%</td></tr><tr><td>Plasmodium Organisms</td><td>39</td><td>9.6%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>How is malaria Transmitted</td><td></td><td></td></tr><tr><td>Bites of any Mosquito</td><td>178</td><td>44.0%</td></tr><tr><td>Bites of insect which has bitten a malaria Patient</td><td>77</td><td>19.0%</td></tr><tr><td>Stagnant water and unclean environment</td><td>149</td><td>36.8%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td colspan="3">Have your Heard about LLITN</td></tr><tr><td>Yes</td><td>299</td><td>74.0%</td></tr><tr><td>No</td><td>105</td><td>25.9%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td colspan="3">Source of Information</td></tr><tr><td>Health center</td><td>98</td><td>24.2%</td></tr><tr><td>Media</td><td>62</td><td>15.3%</td></tr><tr><td>Family/Friends</td><td>44</td><td>10.8%</td></tr><tr><td>Publications/Journals</td><td>70</td><td>17.3%</td></tr><tr><td>School</td><td>55</td><td>13.6%</td></tr><tr><td>Others</td><td>75</td><td>18.5%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td colspan="3">LLITNs is Key in Prevention of Malaria due to its Durability</td></tr><tr><td>Yes</td><td>304</td><td>75.2%</td></tr><tr><td>No</td><td>100</td><td>24.7%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td colspan="3">LLITNs is effective in the Prevention of Malaria when it is air dried frequently</td></tr><tr><td>Yes</td><td>298</td><td>73.7%</td></tr><tr><td>No</td><td>106</td><td>26.2%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr></table>
Overall respondents Knowledge of Long Lasting Insecticide Treated Nets among Respondents
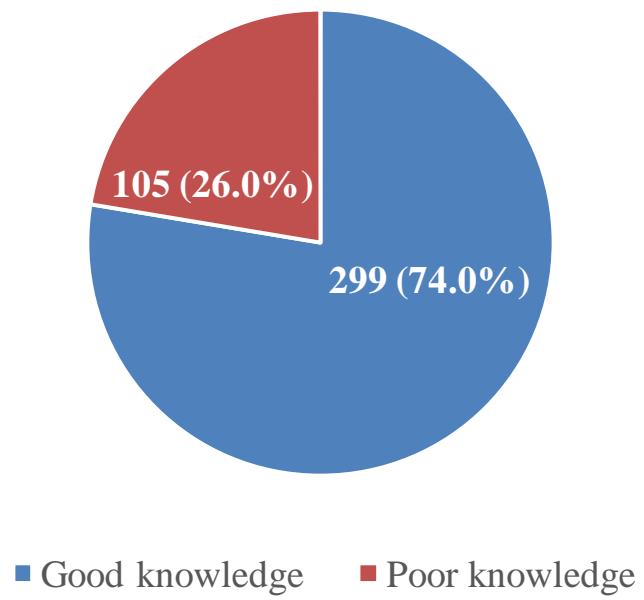 Figure 3: Overall respondents Knowledge of Long Lasting Insecticide Treated Nets among Respondents
Above figure 3 shows that $74.0\%$ (299) of the respondents had good knowledge of long lasting insecticide Treated Nets among respondents while 109 $(26.0\%)$ had poor knowledge.
### c) Distribution and Ownership of Long Lasting Insecticide- Treated Nets among Respondents
The table 3 below revealed the choices of respondents relative to Distribution and Ownership of Long Lasting Insecticide- Treated Nets. When asked if Insecticide Treated Nets had been distributed in their environs, $48.0\%$ (194) replied "Yes" while $51.9\%$ (210) said "No". When the respondents were asked if they had any Insecticide Treated Net, $71.2\%$ (288) affirmed, while $28.7\%$ (116) said "No". The respondents were asked if they owned a Long Lasting Insecticide Treated Nets, $45.0\%$ of the respondents (182) said Yes, while $54.9\%$ (222) denied. On the question 'How did you get it', $38.3\%$ (155) chose Health Centers, $33.1\%$ (134) said "Market", $7.1\%$ (29) said "Friends", $15.0\%$ (61) of the respondents replied "School" while some respondents $6.1\%$ (25) chose options not listed but label 'Others'. When asked How Many ITNs their household Owned, $41.3\%$ (167) of the respondents said "None", $17.8\%$ (72) replied "1", $29.9\%$ (121) said between 2-4, $10.8\%$ (44) of the respondents said "Above 4".
Table 3: Distribution and Ownership of Long Lasting Insecticide- Treated Nets among Respondents
<table><tr><td>Variables</td><td>Frequency (n=404)</td><td>Percentage (%)</td></tr><tr><td>Insecticide Treated Nets distribution in your Area</td><td></td><td></td></tr><tr><td>Yes</td><td>194</td><td>48.0%</td></tr><tr><td>No</td><td>210</td><td>51.9%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Have any Insecticide Treated Net</td><td></td><td></td></tr><tr><td>Yes</td><td>288</td><td>71.2%</td></tr><tr><td>No</td><td>116</td><td>28.7%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Own Long Lasting Insecticide Treated Net</td><td></td><td></td></tr><tr><td>Yes</td><td>182</td><td>45.0%</td></tr><tr><td>No</td><td>222</td><td>54.9%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>How did you get it</td><td></td><td></td></tr><tr><td>Health Center</td><td>155</td><td>38.3%</td></tr><tr><td>Market</td><td>134</td><td>33.1%</td></tr><tr><td>Friend</td><td>29</td><td>7.1%</td></tr><tr><td>School</td><td>61</td><td>15.0%</td></tr><tr><td>Others</td><td>25</td><td>6.1%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>How Many ITNs do your household Own</td><td></td><td></td></tr><tr><td>None</td><td>167</td><td>41.3%</td></tr><tr><td>1</td><td>72</td><td>17.8%</td></tr><tr><td>2-4</td><td>121</td><td>29.9%</td></tr><tr><td>Above 4</td><td>44</td><td>10.8%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr></table>
### d) Level of Utilization of Long Lasting Insecticide-Treated Nets
Table 4 shows the Level of Utilization of Long Lasting Insecticide-Treated Nets among respondents. When asked if they had ever slept under an LLITN, $44.3\%$ (179) said "Yes", while $55.6\%$ (225) replied "No". The respondents were asked if they slept under an LLITN the previous night, $66.0\%$ (267) confirmed, while $33.9\%$ (137) denied. Respondents that denied were in turn asked when last they slept under an LLITN, $42.3\%$ (58) told less than 7 days ago, $33.5\%$ (46) said between
8-29 days, $24.0\%$ (33) more than 30 days. When asked if their children/family members sleep under LLITN, $66.0\%$ (267) confirmed "Yes", while $33.9\%$ (137) said "No". The respondents who replied "No" were then asked if their children/family members slept under an LLITN the previous night, $62.8\%$ (254) confirmed, while $37.1\%$ (150) denied. Respondents that denied were in turn asked when last they slept under an LLITN, $32.0\%$ (48) told less than 7 days ago, $21.3\%$ (32) said between 8-29 days, $46.6\%$ (70) more than 30 days.
Table 4: Level of Utilization of Long Lasting Insecticide-Treated Nets
<table><tr><td>Variable</td><td>Frequency</td><td>Percentage</td></tr><tr><td>Have you Ever Slept under an LLITN?</td><td></td><td></td></tr><tr><td>Yes</td><td>179</td><td>44.3%</td></tr><tr><td>No</td><td>225</td><td>55.6%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Did you sleep under an LLITN Last Night?</td><td></td><td></td></tr><tr><td>Yes</td><td>267</td><td>66.0%</td></tr><tr><td>No</td><td>137</td><td>33.9%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>If No, when was the last time you slept under an LLITN?</td><td></td><td></td></tr><tr><td><7 days ago</td><td>58</td><td>42.3%</td></tr><tr><td>8-29 days</td><td>46</td><td>33.5%</td></tr><tr><td>>30 days</td><td>33</td><td>24.0%</td></tr><tr><td>Total</td><td>137</td><td>100</td></tr><tr><td>Do your children/family Members sleep under LLITN</td><td></td><td></td></tr><tr><td>Yes</td><td>267</td><td>66.0%</td></tr><tr><td>No</td><td>137</td><td>33.9%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td colspan="3">Did they sleep under an LLITN last Night</td></tr><tr><td>Yes</td><td>254</td><td>62.8%</td></tr><tr><td>No</td><td>150</td><td>37.1%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td colspan="3">If No, when was the last time they slept under an LLITN</td></tr><tr><td><7 days ago</td><td>48</td><td>32.0%</td></tr><tr><td>8-29 days</td><td>32</td><td>21.3%</td></tr><tr><td>>30 days</td><td>70</td><td>46.6%</td></tr><tr><td>Total</td><td>150</td><td>100</td></tr></table>
### e) Factors Influencing the Coverage of Long Lasting Insecticide-Treated Nets
Shown in table 5 below are the Factors Influencing the Coverage of Long Lasting Insecticide-Treated Nets among respondents. When asked if Nets Inflicts Rashes, $74.0\%$ (299) of the respondents confirmed, while $25.9\%$ (105) said "No". Considering the Distance to Facility, $62.8\%$ (254) of the respondents said it was a factor, while $37.1\%$ (150) did not consider distance to facility being a factor influencing coverage of LLITNs. When asked about Cultural Acceptance, $44.3\%$ (179) said "Yes" while $55.6\%$ (225) denied. The respondents were questioned concerning Family
Factors; Study shows $71.2\%$ (288) replied "Yes" while $28.7\%$ (116) said "No". On whether Religious Acceptance influenced the use of LLITNs, $4.7\%$ (19) affirmed "Yes" while majority of the respondents with $95.2\%$ (385) said "No". $59.1\%$ (239) denied Difficulty to install a LLITN was a factor influencing the use of the Nets, while $40.8\%$ (165) confirmed. When asked if the respondents had door nets, $64.3\%$ (260) said "Yes", while $35.6\%$ (144) did not have door nets. On Information during Distribution being a factor influencing use of LLITNs was met with $44.0\%$ (178) confirming among the respondents, while $55.9\%$ (226) replied "No".
Table 5: Factors Influencing the Coverage of Long Lasting Insecticide-Treated Nets
<table><tr><td>Variable</td><td>Frequency (n=404)</td><td>Percentage (%)</td></tr><tr><td>Nets Inflicts Rashes</td><td></td><td></td></tr><tr><td>Yes</td><td>299</td><td>74.0%</td></tr><tr><td>No</td><td>105</td><td>25.9%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Distance to Facility</td><td></td><td></td></tr><tr><td>Yes</td><td>254</td><td>62.8%</td></tr><tr><td>No</td><td>150</td><td>37.1%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Cultural Acceptance</td><td></td><td></td></tr><tr><td>Yes</td><td>179</td><td>44.3%</td></tr><tr><td>No</td><td>225</td><td>55.6%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Family Factors</td><td></td><td></td></tr><tr><td>Yes</td><td>288</td><td>71.2%</td></tr><tr><td>No</td><td>116</td><td>28.7%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Religious Acceptance/Factors</td><td></td><td></td></tr><tr><td>Yes</td><td>19</td><td>4.7%</td></tr><tr><td>No</td><td>385</td><td>95.2%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Religious Acceptance</td><td></td><td></td></tr><tr><td>Yes</td><td>194</td><td>48.0%</td></tr><tr><td>No</td><td>210</td><td>51.9%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Difficulty to Hang</td><td></td><td></td></tr><tr><td>Yes</td><td>165</td><td>40.8%</td></tr><tr><td>No</td><td>239</td><td>59.1%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td>Have Door Nets</td><td></td><td></td></tr><tr><td>Yes</td><td>260</td><td>64.3%</td></tr><tr><td>No</td><td>120</td><td>35.6%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr><tr><td colspan="3">Information during Distribution</td></tr><tr><td>Yes</td><td>178</td><td>44.0%</td></tr><tr><td>No</td><td>226</td><td>55.9%</td></tr><tr><td>Total</td><td>404</td><td>100</td></tr></table>
### f) Relationship between Socio-demographic characteristics and level of utilization of long lasting Insecticide Treated Nets
Based on the Relationship between sociodemographic characteristics and level of utilization of long lasting insecticide treated nets, the table below shows that age not significantly associated with level of utilization insecticide treated nets $(P = 0.5301)$. Furthermore, the table 4.6 shows that religion is not significantly associated with utilization of LLITNs $(P = 0.115)$. Also, ethnicity doesn't show significant association with utilization of LLITNs $(P = 0.074)$. Marital status is significantly associated with utilization of LLITNs $(P = 0.0001)$. Moving further, the table reveals that parity is significantly associated with the level of utilization of LLITNs $(P = 0.0001)$. Also, level of education shows significant association with level of utilization of LLITNs $(P = 0.0001)$. Occupation is not significantly associated with level of utilization of LLITNs $(P = 0.942)$. The level of income of the respondents shows significant association with level of utilization of LLITNs $(P = 0.006)$ (Table 6 below).
Table 6: Association between Socio-demographic characteristics and level of utilization of long lasting Insecticide Treated Nets
<table><tr><td>Characteristics</td><td>X2</td><td>D.F</td><td>P value</td><td>Decision</td></tr><tr><td>Age</td><td>106.411</td><td>36</td><td>0.5301</td><td>NS</td></tr><tr><td>Religion</td><td>33.340</td><td>318</td><td>0.115</td><td>NS</td></tr><tr><td>Ethnicity</td><td>53.008</td><td>36</td><td>0.074</td><td>NS</td></tr><tr><td>Marital status</td><td>106.124</td><td>127</td><td>0.0001</td><td>S</td></tr><tr><td>Parity</td><td>81.645</td><td>36</td><td>0.0001</td><td>S</td></tr><tr><td>Education level</td><td>153.283</td><td>36</td><td>0.0001</td><td>S</td></tr><tr><td>Occupation</td><td>31.133</td><td>45</td><td>0.942</td><td>N.S</td></tr><tr><td>Level of income</td><td>71.977</td><td>45</td><td>0.006</td><td>S</td></tr></table>
## IV. DISCUSSION
Based on the finding of this study on Long Lasting Insecticide Treated Nets among women of child bearing age in Nwangele LGA, considering the socio demographic characteristics, it was revealed that majority $41.5\%$ (169) of the women were aged between 26-30 years. This finding goes in consistent with a study by Odoko et al., (2012), that women of child bearing age have a mean age of 32.4yrs. The study revealed that majority $93.8\%$ (379) of the respondents were lgbo region. This could be due to the fact that the study was conducted in Nwangele LGA which is the southeastern part of Nigeria dominated by people of lgbo origin. The findings of the study revealed that $27.2\%$ (110) of the respondents had an income level between 1-10,000 naira. A study by Kenneth and Amefume (2013) posited a significant improvement in income level among women in rural areas. However this goes in contrast with the study with women of child bearing age mostly involved in petty trading.
Considering the level of knowledge of long lasting insecticide treated nets, the study showed that a majority of the respondents with $96.5\%$ (390) are aware and have had heard about malaria prior to the study in consistence with a similar study conducted among groups of women of childbearing age (WOCBA) in Malawi by Owen et al (2018) on the awareness of Malaria among pregnant women. Information on Malaria is now widely open with several sources of information existing. The study posited that $74.0\%$ (299) of the participants had knowledge of long lasting insecticide treated nets. Studies by Kyi et al. (2020) and Adebayo et al. (2014) showed that respondents in an area had $69.6\%$, $81.5\%$ respectively knowledge of long lasting insecticide treated nets which corroborates with the finding of this study. Women of child bearing age at Nwangele are more likely to get information on the utilization and adequate knowledge following community meetings, hospital visits and at educational institutions. The study further revealed that majority $24.2\%$ (98) had heard about LLTINs from Health centers. This goes against a finding by Atenchong et al. (2014) that revealed that majority of women had good knowledge of LLITNs and ITNs from a community follow up program. However from this study it implies that health workers proffer information to women on antenatal and other related periodic health visit by women of child bearing age in the community.
From the study it was revealed that the women when asked if Insecticide Treated Nets had been distributed in their environs, $48.0\%$ (194) agreed. However this shows a poor reach of LLITNs in the community. The findings of this study on distribution of LLITNs reveal that women of child bearing age might experience shortfall of these LLITNs. A study by Kenneth and Amefume (2013) demonstrated that distribution of LLITNs was hugely affected in areas where concerned organizations seek for coverage. From the study $45.0\%$ of the respondents (182) owned long lasting Insecticide treated nets in corroboration with a previous study by Owen et al (2018) on converge and ownership of LLITNs by women in rural areas of Nigeria. Decreased ownership has been stated by the World Health Organization in a recent publication (WHO, 2021). These could be due to a lot of factors which this study sought further to find $38.3\%$ (155) of the women of child bearing age opined that they got LLITNs from Health Centers and $33.1\%$ (134) said Market. A finding by Nankinga et al (2012) posited that majority of resident's uptake ITNs from the Markets which goes against the finding of this study among women of childbearing age.
Based on the Level of Utilization of Long Lasting Insecticide-Treated Nets among the women, the study revealed that $44.3\%$ (179) of the women said yes when asked if they had ever slept under an LLITN which goes against the finding by Adebayo et al (2014) on utilization of insecticide treated nets. Several factors could be responsible for the low uptake of insecticide treated nets among the women which was investigated by the study. According to Bennett et al. (2012) usage of LLITNs can be harnessed by several factors which could include, itches, reactions etc.
Furthermore, based on the factors influencing the Coverage of Long Lasting Insecticide-Treated Nets among respondents, when asked if Nets Inflicts Rashes, $74.0\%$ (299) of the respondents opined it does. This finding goes in consistent with previous studies on the factors influencing uptake of LLITNs among women (Iwu et al., 2010: Aina & Ayeni, 2011: Ganihu & Jimo, 2013). However in this study, participants posited that Considering the Distance to Facility, $62.8\%$ (254) of the respondents said it was a factor towards their utilization. This implies that the health center is situated far away from them. When asked about Cultural Acceptance, $55.6\%$ (225) denied it could influence their utilization and the coverage of LLITNS in the area. This goes against a study conducted at rural Dars es Salaam that showed majority of respondents agreeing cultural acceptance as a modifier to Malaria preventive behavior. The study revealed also that information during Distribution being a factor influencing use of LLITNs was met with $44.0\%$ (178) confirming among the women of child bearing age (Charles et al., 2019). A publication by Kyi et al. (2020) revealed that source of information on malaria preventive approaches was imperative in determining its uptake. The finding of this study shows that for women of child bearing age, information on utilization is essential for them to utilize LLITNs.
demonstrated that parity is significantly associated with the level of utilization of LLITNs $(P = 0.0001)$. This could be due to the fact that increasing number of children can lead to uptake as well as less number of children. This goes in contrast with a report published by Nankinga et al (2012) on Parity and Usage of Nets. Also, from the study among women of child bearing age in Nwangele, it was posited that level of education shows significant association with level of utilization of LLITNs $(P = 0.0001)$. Women of child of bearing age with educational level and information on ITNs would likely utilize LLITNs. The study revealed that the level of income of the women shows significant association with level of utilization of LLITNs $(P = 0.006)$. A study by Owen et al (2018) opined that women with higher income status could afford malaria preventive. This implies that from the findings of this study among women of child bearing age at Nwangele it is more likely for them to purchase LLITNs if they have the money.
## V. CONCLUSION
However, from the study, the coverage and distribution of long lasting insecticide treated nets in Nwangele LGA forms part of the component of the 2011 RBM integration which is effective in rapidly increasing household possession and use of bed nets, achieving national bed net coverage goals set by National Health Development Plan (NHDP) 2012-2015. Low Ownership of LLITNs was reported in the study and malaria is a very serious public health problem; prompt treatment alone cannot guarantee the achievement of the goal. All strategies must be strengthened and employed in fight against malaria, if the desired goal is to be achieved. Findings from this study showed that majority of the residents had a considerable good knowledge of the use of insecticide treated nets but low ownership.
## VI. RECOMMENDATIONS
The recommendations for this study include the following;
1. Health education on the effective use of long lasting insecticide treated nets among residents and practices to improve ownership and function.
2. Health facilities at Nwangele LGA should liaise with relevant stakeholders and authorities to improvise the distribution of safe insecticide treated nets to residents and patients affected.
3. The federal government should train and empower a skilled manpower in surveillance and frequent check up of distribution gaps in LLITNs in the rural communities through the help of agencies and concerned nongovernmental organizations.
4. Public Health Officers and Environmental health personnel's should develop policies that would mandate the government and legislative bodies to
enact them to help protect the wider community at large.
### SECTION A: SOCIO DEMOGRAPHIC CHARACTERISTICS
INSTRUCTION: Please tick (√) the correct options besides each question and also fill in the spaces provided where appropriate with the correct options.
1. What is your Age: (a) 15-20 [](b) 21-25 (c) 26-30 [](d) 31-40 [](d) 41-45 []
2. Religion: (a) Christianity [](b) Muslim [](c) Traditional [](d) Others (Please Specify)
3. Ethnicity (a) Igbo [](b) Hausa [](c) Yoruba [](d) Fulani [](e) Others (please specify).
4. Marital status (a) Married [](b.) Single [](c.) Separated [](d) Widowed []
5. Number of children (Parity) (a) None [](b) 1-2 [](c) 3-5 [](d) above 5 []
6. Education level (a.) No formal education [](b.) Primary [](c.) Secondary [](d.) Tertiary [](e) others (specify).
7. Your occupation: (a) Artisan e.g Carpenter, Hairdresser, Tailor, Driver [](b) Civil servant e.g Teacher [](c) Self-employed e.g Trader, Photographer [](d) Unemployed [](e) Professionals e.g. Doctor, Nurse, Lawyer, Accountant [](f) Others (please specify)
8. What is your Level of Income (a.) 1-10,000 [](b.) 11,000-30,000 [](c.) 31,000-50,000 [](d.) 51,000-100,000 [](e) above 100,000 []
#### SECTION B: KNOWLEDGE OF LONG LASTING INSECTICIDE-TREATED NETS
Please tick (√) the correct options besides each question and also fill in the spaces provided where appropriate with the correct options.
9. Have you heard about Malaria (a) Yes [](b) No []
10. Have you suffered from Malaria before? (a) Yes [](b) No []
11. What causes malaria (a) Germs [](b) Dirts/stagnant water [](c) Mosquito bites [](d) plasmodium organisms [](d) others............
12. How is malaria Transmitted? (a) Bites of any Mosquito [](b) Bites of insect which has bitten a malaria Patient [](c) Stagnant water and unclean environment []
13. Have you heard about Long Lasting Insecticide treated Nets (LLITNs)? (a) Yes [](b) No[]
14. How did you hear about it? (a) Health center [](b) Media [](c) Friends/Family [](d) Publications/Journals [](e) School [](f) others............
15. Long Lasting Insecticide treated Nets (LLITNs) is Key in Prevention of Malaria due to its Durability (a) Yes [](b) No []
16. Long Lasting Insecticide treated Nets (LLITNs) is effective in the Prevention of Malaria when it is air dried frequently (a) Yes [](b) No []
## SECTION C: DISTRIBUTION AND OWNERSHIP OF LONG LASTING INSECTICIDE- TREATED NETS AMONG RESPONDENTS
17. Has Insecticide Treated Nets been distributed in your Area? (a) Yes [](b) No []
18. Do you have any Insecticide Treated Net? (a) Yes [](b) No []
19. Do you Own any Long Lasting Insecticide treated net(a) Yes [](b) No []
20. How did you get it?
a) Health center [](b) Market [](c) A Friend [](d) others............
21. How Many ITNs do your household Own? (a) None [](b) 1 [](c) 2-3 [](d) 4 [](e) above 4 []
### SECTION D: LEVEL OF UTILIZATION OF LONG LASTING INSECTICIDE-TREATED NETS
Please tick (√) the correct options besides each question and also fill in the spaces provided where appropriate with the correct options.
22. Have you Ever Slept under an LLITN? (a) Yes [](b) No []
23. Did you sleep under an LLITN Last Night? (a) Yes [](b) No []
24. If No, when was the last time you slept under an LLITN? (a) $< 7$ days ago [](b) 8-29 days [](c) $> 30$ days []
25. Do your children/family Members sleep under LLITN? (a) Yes [](b) No []
26. Did they sleep under an LLITN last Night?
27. If No, when was the last time they slept under an LLITN? (a) $< 7$ days ago [](b) 8-29 days [](c) $> 30$ days []
#### SECTION E: FACTORS INFLUENCING THE COVERAGE OF LONG LASTING INSECTICIDE- TREATED NETS
Please tick (√) the correct options that influence Utility and coverage of Long lasting Ins ecticide treated Nets in the spaces provided in the Table below.
<table><tr><td>S/N</td><td>Factors Influencing Coverage</td><td>Yes</td><td>No</td></tr><tr><td>1.</td><td>Nets Inflicts Rashes</td><td></td><td></td></tr><tr><td>2.</td><td>Distance to Facility</td><td></td><td></td></tr><tr><td>3.</td><td>Cultural Acceptance</td><td></td><td></td></tr><tr><td>4.</td><td>Family Factors</td><td></td><td></td></tr><tr><td>5.</td><td>Religious Acceptance/Factors</td><td></td><td></td></tr><tr><td>6.</td><td>Difficulty to Hang</td><td></td><td></td></tr><tr><td>7.</td><td>Have Door Nets</td><td></td><td></td></tr><tr><td>8.</td><td>Information during Distribution</td><td></td><td></td></tr></table>
Generating HTML Viewer...
References
97 Cites in Article
Ayodeji Adebayo,Oluwaseun Akinyemi,Eniola Cadmus (2014). Knowledge of malaria prevention among pregnant women and female caregivers of under-five children in rural southwest Nigeria.
A Adeyemi,D Adekanle,S Akinola (2007). Use Prevalence of Insecticide-Treated Mosquito Bed Nets among Pregnant Population in Osogbo, Nigeria.
B Aina,F Ayeni (2011). Knowledge and use of Insecticide treated net as a malaria preventive tool among pregnant women in a local Government area of Lagos State.
J Aluko,A Oluwatosin (2012). Randomized Control Trail and Utilization of Insecticide treated nets during pregnancy among postpartum women in Ibadan Kenya: a cross sectional study.
E Amedo (2016). Utilisation of insecticide treated mosquito nets among caregivers of children under five years in Hohoe township in Ghana.
D Aribodor,O Nwaorgu,C Eneanya,O Aribodor (2017). Malaria among primigravid women attending antenatal clinics in Awka, Anambra State, south-east Nigeria.
Alicia Arnott,Alyssa Barry,John Reeder (2012). Understanding the population genetics of Plasmodium vivax is essential for malaria control and elimination.
M Atenchong,U Ngwibete,I Ozims,N James (2014). A Survey of Ownership and Utilization of Insecticide Treated Nets (ITNs) among Pregnant Women Attending Anc Clinic.
N Attanayake,J Fox-Rushby,A Mills (2018). Household costs of malaria morbidity: a study in Matale district, Sri Lanka.
B Azabre,K Teye,J Yaro (2013). Malaria control strategies in the Kasena-Nankana east and west districts of Ghana.
M Baley,W Deressa (2008). Use of insecticide treated nets by pregnant women and associated factors in a predominantly rural population in Northern Ethiopia.
A Bennett,S Smith,S Yambasu,A Jambai,W Alemu,A Kabano (2012). Household Possession and Use of Insecticide-Treated Mosquito Nets in Sierra Leone 6 Months after a National Mass-Distribution Campaign.
Jubilate Bernard,George Mtove,Renata Mandike,Frank Mtei,Caroline Maxwell,Hugh Reyburn (2009). Equity and coverage of insecticide-treated bed nets in an area of intense transmission of Plasmodium falciparum in Tanzania.
N Charles,Y Njumkeng,O Tobias (2019). Coverage and usage of insecticide treated nets (ITNs) within households: associated factors and effect on the prevalance of malaria parasitemia in the Mount Cameroon area.
Reginald Chima,Catherine Goodman,Anne Mills (2013). The economic impact of malaria in Africa: a critical review of the evidence.
U Chukwuocha,Ins Dozie,Beb Nwoke,C Ukaga,Coe Onwuliri,A Osuagwu (2010). The Clinical Pattern and Complications of Severe Malaria in Parts of the Imo River Basin of Nigeria.
William Collins,John Barnwell (2009). <i>Plasmodium knowlesi:</i>Finally Being Recognized.
A Adeneye,A Jegede,M Mafe,E Nwokocha (2011). A Pilot Study to Evaluate Malaria Control Strategies in Ogun State, Nigeria.
Konlan Diema,Konlan Dodam,Millicent Aarah-Bapuah,Abdulai Asibi (2015). Barriers to sustained use of the insecticide treated bed net in the upper east region of Ghana.
U Dupas,I Cohen (2009). Decreased motivation in the use of insecticide-treated nets in a malaria endemic area in Burkina Faso.
F Espino (1997). Perceptions of malaria in a low endemic area in Nigeria: transmission and prevention of disease.
Fmoh (2015). Emergency department management of mosquitoborne illness: Malaria, dengue, and west Nile virus.
Fmoh (2015). Emergency department management of mosquitoborne illness: Malaria, dengue, and west Nile virus.
A Ganihu,R Jimo (2013). Awareness and Use of Insecticide treated nets among women attending antenatal clinic in a Northern state of Nigeria.
Helen Guyatt,Sam Ochola (2014). Use of bednets given free to pregnant women in Kenya.
T Hartman,S Rogerson,P Fischer (2019). The impact of maternal malaria on newborns.
Ay Isah,E Nwobodo (2009). Awareness and utilization of insecticides treated mosquito nets among pregnant mothers at tertiary health institution in North-Western Nigeria.
R Iwu,B Ijioma,A Egeruoh,I Awurum,C Ohalete (2010). Awareness and use of Insecticide treated among pregnant women attending antenatal clinic at Federal Medical centre and General Hospital Owerri, Imo State.
A Johnson,U Inyang,U Etuknwa,U Ekanem,M Udo,H Ubom (2018). Cost Analysis of insecticide treated nets among households in teh rural community of sourthern Nigeria.
W Kenneth,N Amefume (2013). Postnatal Care Utilization and Its Determinants in Loma District, Southwest Ethiopia: A Community Based Cross Sectional Study.
M Kiwuwa,A Stergachis (2012). Determination of use of Insecticide treated nets for the prevention of malaria in pregnancy: Jinga Uganda.
A Kweku,G Sodofia,E Kye-Duedo,I Agboli,U Agbemafle (2016). Ownership and utilization of long lasting insecticide treated nets (LLIN) and factors associated to non-utilization among pregnant women in Ho municipality of Ghana.
V Kyi,C Thar-Min,H Thae,A Maung (2015). Utilization of insecticide-treated bed nets and care-seeking for fever and its associated sociodemographic and geographical factors among under-five children in different regions: evidence from the Myanmar Demographic and Health Survey.
J Mbanugo,O Okorudo (2015). Prevalence of Plasmodium infections in Pregnant women in Aguata, Anambra state, South Eastern Nigeria.
I Mueller,P Zimmerman,J Reeder (2017). Plasmodium malariae and Plasmodium ovale-the "bashful" malaria parasites.
O Musa,G Salaudeen,R Jimo (2017). Awareness and use of Insecticide treated nets among women attending antenatal clinic in a Northern state of Nigeria.
Ziadah Nankinga,Joshua Muliira,Joan Kalyango,Joaniter Nankabirwa,Steven Kiwuwa,Denise Njama-Meya,Charles Karamagi (2012). Factors Associated with Utilization of Insecticide-Treated Nets in Children Seeking Health Care at a Ugandan Hospital: Perspective of Child Caregivers.
(2006). Nigerian Census and population committee.
M Oche,I Ameh,A Umar,G Gana,C Njoku (2011). Awareness and the use of Insecticide Treated Net (ITN) among pregnant women attending ante-natal at Usmanu Danfodiyo University Teaching Hospital, Sokoto.
Joseph Odoko,Ezekiel Nwose,Samuel Nwajei,Emmanuel Agege,John Moyegbone,Eunice Igumbor (2012). Epidemiology of malaria as it relates to utilization of insecticide treated nets among pregnant women and under five years children in South-South Nigeria.
L Odumegwu (2013). Undernutrition as an underlying cause of malaria morbidity and mortality in children less than five years old in Nigeria.
C Okoye,A Isara (2011). Awareness on the use of Insecticide treated nets among women attending antenatal clinic in a tertiary heath facility in South-South Nigeria.
O Okwa (2004). Preliminary investigations on malaria in sickle cell patients among pregnant women and infants in Lagos, Nigeria.
Jso Osero,M Otieno,Ass Orago (2015). Maternal use of insecticide-treated nets in the prevention of Malaria among children under five years in Nyamira District, Kenya.
B Owen,I Nkoka,V Ting-Wu,H Chuang (2018). Factors associated with insecticide-treated net usage among women of childbearing age in Malawi: a multilevel analysis.
W Richard,L Bernard,L Nah,E Mornica,U Parise,M Clara (2008). The burden of malaria in pregnancy in malaria endemic areas.
Marcus Rijken,Rose Mcgready,Machteld Boel,Rini Poespoprodjo,Neeru Singh,Din Syafruddin,Stephen Rogerson,François Nosten (2012). Malaria in pregnancy in the Asia-Pacific region.
L Ruben-Diaz (2011). Level of awareness, Ownership and Use of Insecticide Treated Bed Nets (ITNs) by Pregnant Women Attending Antenatal Clinics in Anambra state, South Eastern Nigeria.
T Runsewe-Abiodun,A Inyanwura,S Sotimehin (2012). Awareness and knowledge about Insecticide treated nets amongst pregnant mothers in Ogun state, Western Nigeria: A descriptive cross sectional study.
G Salaudeen,K Jimoh (2009). Awareness and use of insecticide treated nets among women attending antenatal clinics in a Northern state of Nigeria.
Pralay Sarkar,Gautam Ahluwalia,Vannan Vijayan,Arunabh Talwar (2009). Critical Care Aspects of Malaria.
U Ukibe,E Tailor,D Nku,S Duvail,M Tabala,S Meshnick,E Bechets (2017). Free distribution of insecticide treated bed nets to pregnant women in Kinshasa: an effective way to achieve 80% use by women and their newborns.
V Wagbasoma,E Aigbe (2010). A Survey of Ownership and Utilization of Insecticide Treated Nets (ITNs) among Pregnant Women Attending Anc Clinic.
(2016). World report on social determinants of health equity.
(2019). WHO guidelines for malaria, 13 August 2025.
E Worrall,S Basu,K Hanson (2012). The relationship between socioeconomic status and malaria: a review of the literature.
(2020). What your brand’s purpose is not.
(null). Christianity as a World Religion.
(2006). 5 Making a Larger Community: Igbo Ethnicity.
Marital status (a) Married.
(2014). Single-Arm, Single-Leg Deadlift.
Ronit Pinchas Mizrachi,Dan Bouhnik (2025). The parity paradox: does number of children (parity) influence breast cancer mortality across the life course?.
(2013). The Primary School.
Unknown Title.
Your occupation.
(null). Figure 5.4. More unemployed people become self-employed than those seeking it.
Section B KNOWLEDGE OF LONG LASTING INSECTICIDE-TREATED NETS Please tick (√) the correct options besides each quest ion and also fill in the spaces provided where appropriate with the correct options.
Daniel Hammett,Laura Martin,Izuu Nwankwọ (2023). Preamble.
Anthony Ajayi,Elita Chamdimba (2024). Have you ever suffered intimate partner abuse? We asked girls in Malawi and 40% said yes.
A Enayati,P Garner,J Hemingway (2005). Electronic mosquito repellents for preventing mosquito bites and malaria infection.
(2007). Mosquito Bites Boost Resistance to Malaria.
Y Shirayama,S Phompida,C Kuroiwa,M Miyoshi,J Okumura,J Kobayashi (2007). Maintenance behaviour and long-lasting insecticide-treated nets (LLITNs) previously introduced into Bourapar district, Khammouane province, Lao PDR.
(1400). Did You Hear the One About the Irishman …?.
(1995). Biographical Directory.
(null). How others see us.
(2025). Cost Effectiveness of Long-Lasting Insecticide Treated Bed Nets Distribution in Prevention of Malaria Deaths and Morbidity in Guyana.
(2025). Cost Effectiveness of Long-Lasting Insecticide Treated Bed Nets Distribution in Prevention of Malaria Deaths and Morbidity in Guyana.
C: Distribution And Ownership Of Section,Long LASTING INSECTICIDE-TREATED NETS AMONG RESPONDENTS.
Leslie Choi,Joseph Pryce,Paul Garner (2017). The combination of indoor residual spraying with insecticide-treated nets versus insecticide-treated nets alone for preventing malaria.
Tejas Sathe (2023). Do you have any questions for me?.
Mengistie Tariku (2021). Utilization of Long-lasting Insecticide Treated Net and Associated Factors Among Pregnant Women in Awabel District,North-West Ethiopia, 2017.
(1998). 4. Escape 'How Did You Get Out of It?'.
(2002). Chapter Two. Charles Dickens: The Other's Other in Our Mutual Friend.
Steve Ellen (2014). How well do you know your own feelings?.
Section D (2025). Utilization of Long-lasting Insecticide treated Mosquito Nets amongst Households in Upper River Region, The Gambia.
(2007). Are You Now or Have You Ever Been?.
Did you sleep under an LLITN Last Night?.
(1998). WHEN WAS THE LAST TIME YOU SLEPT THIS SOUNDLY?.
(2024). Yes, your pet might eat your corpse. That’s a problem for investigators.
Did they sleep under an LLITN last Night?.
(1998). WHEN WAS THE LAST TIME YOU SLEPT THIS SOUNDLY?.
Section E FACTORS INFLUENCING THE COVERAGE OF LONG LASTING INSECTICIDE-TREATED NETS Please tick.
N Factors Influencing Coverage Yes No 1. Nets Inflicts Rashes 2.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
David Chinaecherem Innocent. 2026. \u201cAssessment of Long Lasting Insecticide Treated Net among Women of Child Bearing Age in a Community in South Eastern Nigeria\u201d. Global Journal of Medical Research - F: Diseases GJMR-F Volume 23 (GJMR Volume 23 Issue F1).
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.