The results of studies of intraoperative x-ray radiation with the participation of two groups are presented: the main database using a neuronavigation group and a control group where standard 2D fluoroscopy was used. The radiation load on the operating surgery and operating supporting staff was estimated. Stryker iNtellect ENT Second Generation Navigation for the Injured of RFD Ziehm Vision Core and Optical Converters for the Injured of the Control Group. Variants of visualization using an electron-optical transducer are especially important for minimally invasive procedure where instrumentation is performed percutaneously without direct anatomical control in contrast to open procedures or work with misrepresented anatomical structures in case of injuries. Biplanar fluoroscopy was one of the first methods of intraoperative imaging in real time as well as one of the most advanced technologies in orthopedic and spinal surgery. However, radiation exposure from intraoperative fluoroscopy remains a serious problem for patients, surgeons and supporting staff.
## I. INTRODUCTION
Currently, much attention is being paid to the impact of ionizing radiation on patients and medical personnel. This is due to the fact that in almost all fields of medicine, diagnostic search and surgical imaging techniques are closely related to x-ray radiation.
One of the most important diagnostic methods of mankind appeared due to Professor of Physics at the University of Würzburg Wilhelm Conrad Roentgen (1845-1923), who discovered the "X-rays" on November 8, 1895, for which he was later awarded the Nobel prize. It was the time when the era of medical imaging begins, which allows us to objectively assess the quantitative and qualitative pathological processes occurring in the human body.
One of the urgent problems of minimally invasive surgery is the impact of ionizing radiation on the human body, particularly the effect on the structure of deoxyribonucleic acid (DNA), which leads to irreversible changes. Negative effects of ionizing radiation lead to cell damage through DNA induction and the release of reactive oxygen species. In this regard, cell death or genome instability occurs, which leads to various radiation-related pathologies. Children and people of reproductive age are primarily at high risk [1, 2]. This is due to the high intensity of replication processes which occur with damage to the DNA structure under the influence of ionizing radiation, thereby causing mutations in the daughter chain. The probability of transmitting a damaged DNA chain to offspring is currently not confirmed [3].
The most frequent and actively used type of imaging when fixing the spine with transpedicular metal structures is biplane radioscopy.
In the attempts to reduce the risks associated with ionizing radiation to the body, radiation safety has become an important topic in the medical industry. All practitioners regardless of the field of medicine can apply the radiation safety methods, including shielding and distancing to reduce radiation exposure. In addition, detailed adjustment of the parameters for bringing doses of fluoroscopic racks and new imaging techniques can be used as an effective way to reduce the radiation dose [9].
Neuronavigation systems have become a new visualization technique. The main purpose of these systems was to provide a reliable assistance for surgical interventions, to reduce intraoperative radiation load and surgical aggression [4]. While the number of new advanced radiation safety technologies in spinal surgery is not large, much needs to be done to overcome the difficulties and limitations associated with funding, material supply, and a fairly labor-intensive training process.
The use of fixation structures and other implants is particularly relevant in the field of spinal surgery, where instrumentation is often used for the treatment of degenerative, traumatic and neoplastic diseases.
Screws used for spinal fusion are the most widely used methods of stabilization in spinal surgery, but inaccurate implantation of such structures can lead to significant intraoperative and postoperative complications [6, 11, 13]. In particular, damage to nearby neurovascular structures can occur leading to severe complications or disability of patients.
To ensure high accuracy of placement of metal structures in spinal surgery intraoperative radiography is used as a navigator when placing implants [12, 16]. This imaging option is particularly important in minimally invasive interventions where instrumentation is performed percutaneously without direct anatomical imaging as opposed to open procedures or surgery of misrepresented anatomy in case of injuries.
2D fluoroscopy is the first and one of the most reliable methods of intraoperative navigation in real time and continues to be one of the leading techniques for controlling screw implantation [5, 8, 10].
However, radiation exposure from intraoperative fluoroscopy is a serious problem for patients, surgeons, and operating room support staff [14 - 15, 17 - 18]. Personal protective equipment and the latest imaging techniques such as neuronavigation have been developed in order to reduce the risk associated with intraoperative radiation. Organizations have also been established in our country and abroad that have developed documents and legal acts regulating work with ionizing radiation designed to protect staff and patients from the harmful effects of radiation. In our country the documents regulating work with x-ray radiation are the sanitary rules and regulations "Hygienic requirements for the device and operation of x-ray devices and x-ray research" SanPiN 2.6.1.1192-03, Federal law No. 3 of 09.01.1996 "About radiation safety of the population", Order of the Minister of Defense (MD) of the Russian Federation (RF) of 07.04.2003 No. 111 "Approval of instructions for the organization in military units and institutions using sources of ionizing radiation".
The criteria of these guidelines are designed to protect those who are exposed to excessive radiation exposure in professional practice as well as to reduce the radiation load on the patient. The main international organization developing these guidelines is the International Commission on Radiological Protection (ICRP).
In both national and foreign regulatory documents, the dosage limits are expressed in joules per kilogram (j/kg) otherwise known as Sievert (SV). The latter is a measure of stochastic exposure of ionizing radiation and an exposure of 1 SV is associated with a $5.5\%$ risk of cancer. According to the ICRP guidelines occupational exposure should be limited to a maximum average of $20\mathrm{mSv}$ per year for no more than a five-year period, with exposure not exceeding $50\mathrm{mSv}$ per year. Exposures should be strictly limited to a maximum average of $1\mathrm{mSv}$ per year over a 5-year period for patients [7]. These values can be used as benchmarks for evaluating the safety and effectiveness of new imaging technologies and anti-radiation protection methods. At the same time, when there is a question of saving the life of the injured the standards and doses of ionizing radiation affecting the injured are erased or expanded.
## II. PURPOSE OF RESEARCH
To prove experimentally that neuronavigation technologies in comparison with standard methods of fluoroscopy can significantly reduce the intraoperative radiation load on the injured, surgeons and auxiliary medical personnel of the operating room.
## III. MATERIALS AND METHODS
The results of 21 patients with combined vertebral-cerebrospinal injury (VCI) who made up the main hard data were analyzed prospectively as well as the results of treatment of 45 patients with severe combined injury (SCI) of spine and spinal cord who made up the control group.
The average age of the injured of the main hard data was 39 years, including 18 men and 3 women. The average value of the severity of combined trauma on the scale of military field surgery-injuries (MFS-I) = 5.8 points.
The injured of this group were operated on for spinal injuries in the clinic of Military Field Surgery (MFS) of the Military Medical Academy named after S. M. Kirov (MMA) in the period from 2017 to 2019. The injured were included in the main hard data according to the following criteria: all of them had combined injuries to the spine and spinal cord, indications for performing posterior spondylodesis based on data obtained by computed tomography (CT) and/or magnetic resonance imaging (MRI), performed when they were hospitalized in the clinic's reception and diagnostic Department (RDD). The use of CT-based intraoperative neuronavigation for spinal surgery has been studied to reduce the use of radioscopy and improve the accuracy of screw implantation.
The average age of the injured of the control group was 33 years, including 35 men and 10 women. The average value of the severity of combined injuries on a scale MFS-lwas 8.8 points. The injured were operated on at the MFS of MMA clinic between 2011 and 2016.
The injured of both groups had similar spinal injuries (compression-comminuted fractures, fractures-dislocations, spondylolistheses) accompanied by instability and neurological deficit. The spinal operations were performed using standard fluoroscopy.
In the control group, the screws were implanted using classical fluoroscopy using a Vision RFD device manufactured by Ziehm (Germany). Individual dosimeters (ID) were used to assess radiation exposure from intraoperative fluoroscopy. In the course of the study the radiation dose received by the injured, operating surgeons and other medical personnel of the operating room (anesthesiologists, anesthesiologist and operating nurses, aidmen) was evaluated.
Note that radiation exposure during spinal surgery is a serious risk factor for operating surgeons, staff and patients adversely affecting the body. However, the actual biological effect is determined by cumulative exposure over long periods of time. The cumulative effect of x-rays can be a serious risk to the health of surgeons and medical staff. The radiation dose that affects the body will be affected by the factors such as the distance from the source to the object, screening and the time of the x-ray. The main tasks facing medicine to reduce the impact of ionizing radiation on surgeons and medical personnel are to find ways to reduce radiation load.
To evaluate the received doses of ionizing radiation of surgeons during surgery, the ID was placed on the surgeon:
1) in the orbits and under the surgical magnifying glass, in maximum proximity to the eye (fixed on the bracket), figure 1;
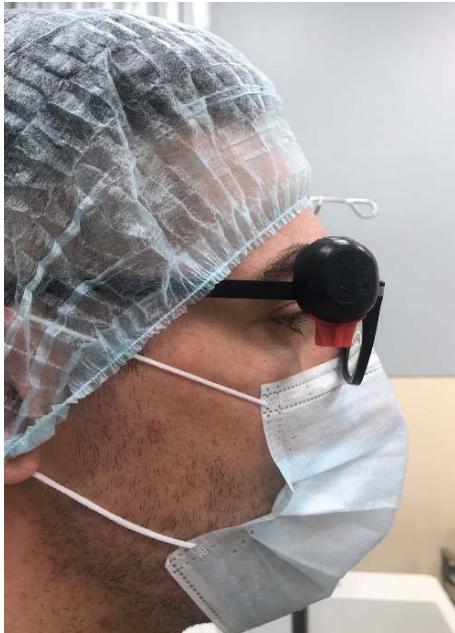 Figure 1: Individual dosimeter fixed in the orbit area
2) In the area of the neck that is not covered by the neck collar (the neck of surgical underwear is fixed) to assess the impact on the thyroid and upper breast (Fig. 2);
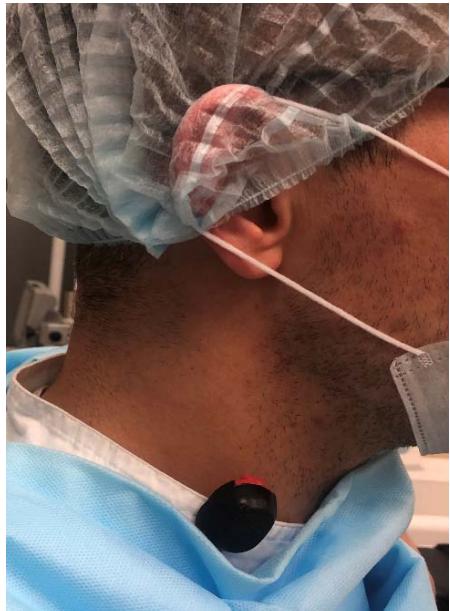 Figure 2: Individual dosimeter fixed in the neck area
3) On the right back surface of the operating surgeon's right hand, in the area of the wrist joint under the surgical glove (Fig. 3);
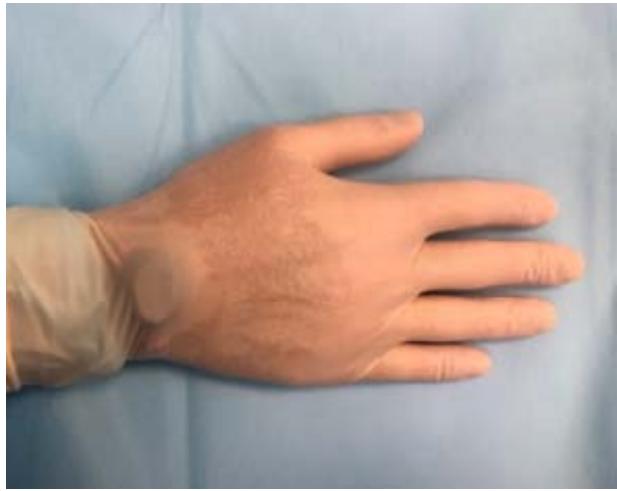 Figure 3: Individual dosimeter fixed in the area of the wrist joint
4) On the surface of the chest and in the groin area under the standard protective apron of the surgeon (Fig.4).
 Figure 4: Standard x-ray protection apron
All personal protective equipment is regulated by the interstate standard from 01.01.2015 "Protection Against X-ray Radiation in Medical Diagnostics. Part 3. Protective Clothing", individual dosimeters on the injured were located in the scanning zone (cervical, thoracic, lumbar spine). Tracking the doses of ionizing radiation on the injured for each zone was performed using two IDs to clarify the average value. In the operating room two sensors were placed which were located from the x-ray source at a distance of 1 and $2\mathrm{m}$. In addition, we used individual thermoluminescent dosimeters (thermoluminescent solid-state detector TSD-4 TU 50.477-85) of the company "DTU-1". After the surgery the dosimeters were removed from the work area and protected from further radiation.
All the IDs used in our study were identical and the results from all the sensors were recorded on the same device by the same specialist who was responsible for the measurement results. The dosimeters were processed and the measurements were tabulated.
The x-ray source of the electron-optical Converter (EOC) was located in 2 projections (straight and side) in relation to the operating field and on the side opposite to the surgeon (Fig. 5). The injured was not screened in the operating room.
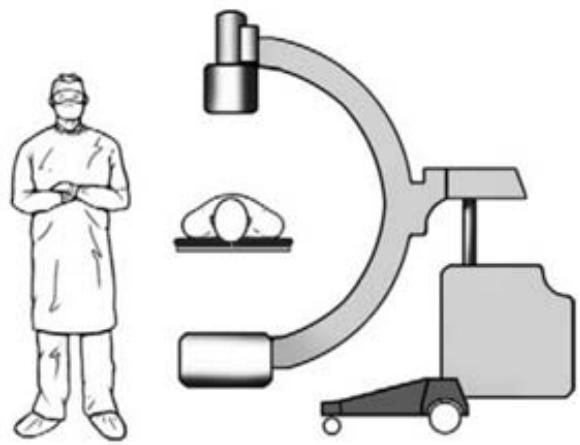 Figure 5: The position of the EOC x-ray source in relation to the patient's back
For the injured of the main hard data the 2nd-generation "iNtellect Navigation" of Stryker (USA) was used to install the transpedicular structure (Fig. 6).
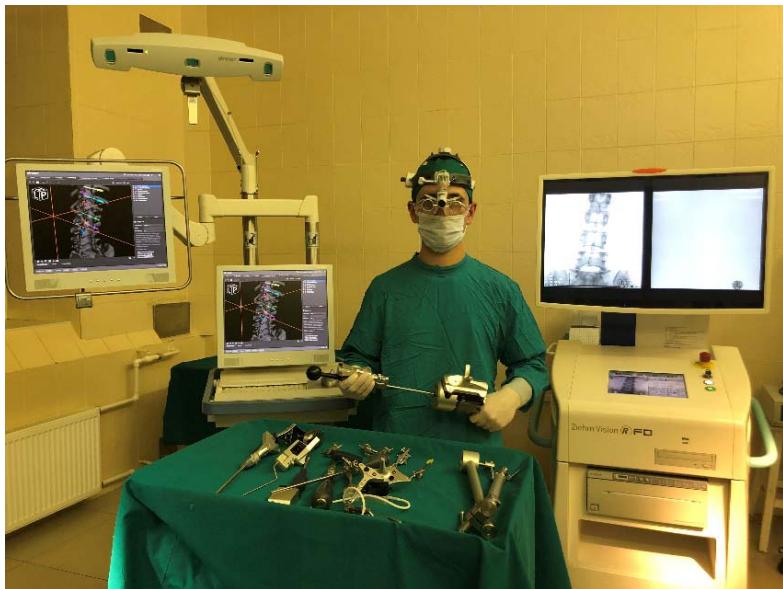 Figure 6: Neuro-navigation rack "iNtellect Navigation" of company "Stryker" (USA) with a set of basic tools
All the injured were operated on using 3D modeling of data obtained during preoperative CT scanning.
Single "forced radiation doses" for diagnostic and therapeutic purposes the so-called average effective doses per examination using medical sources of ionizing radiation were as follows:
- Radiography overview (chest) - 0.150-0.400 mSv;
- Radiography of the limb-0.02 mSv;
- Computed tomography on standard devices - 20 mSv, if the study was performed in the "Whole body" mode and is a native scan-40 mSv. In cases where contrast is introduced during the study - 50 mSv for one study in the "Whole body" mode (the figures may vary depending on body weight, injuries, etc.).
At the same time, the maximum allowable annual rate for personnel working with x - ray radiation is 20 mSv (the periods of receiving this dose should not exceed 5 years); the maximum annual rate for a healthy person is $1 \mathrm{mSv}$; natural annual radiation for a person is $3 \mathrm{mSv}$ per year; the first signs of radiation sickness are $250 - 300 \mathrm{mSv}$.
## IV. RESULTS AND DISCUSSION
It was found that the dose of x-ray radiation during the installation of transpedicular fixation using x-rays on the cervical, thoracic and lumbar spine with a total number for the entire structure was: for the injured in the lumbar spine and pelvic region - 1.22 mSv-1st detector; 1.05 mSv-2nd detector, average value-1.14 mSv (0.11 P), for the thoracic spine and chest cavity organs - 1st detector-2.17 mSv, 2nd detector - 2.0 mSv, average value-2.09 mSv (0.2 P), and the cervical spine - 1st detector - 0.264 mSv, 2nd detector - 0.212 mSv, average value-0.238 mSv (0.023 P).
For the operating surgeon the x - ray radiation dose when fixed on the right hand was- 1st Indicator detector - 1.87 mSv, 2nd detector-0.75 mSv, average value - 1.31 mSv (0.26 p), on the protected thyroid gland- 1st detector - 0.12 mSv, 2nd detector-0.095 mSv, average value - 0.11 mSv, on the head and eye area-1st detector - 0.09 mSv, 2nd detector - 0.07 mSv, average value - 0.08 mSv (0.009 p). In turn, personal protective equipment against x-ray radiation (individual aprons) demonstrated a reliable protection since the radiation dose on dosimeters when working with them was - 0 mSv.
X-ray irradiation doses when installing transpedicular fixations at different levels of the spine on a single screw were as follows: in the cervical spine - 0.034 mSv, in the thoracic spine - 0.075 mSv and in the lumbosacral spine-0.063 mSv.
Indicators of ID located in the operating room at a distance of 1 and $2\mathrm{m}$ from the x-ray source were 0.3 and $0\mathrm{mSv}$ (Fig. 7). This location of the ID was necessary to assess the spread of x-rays in the operating room.
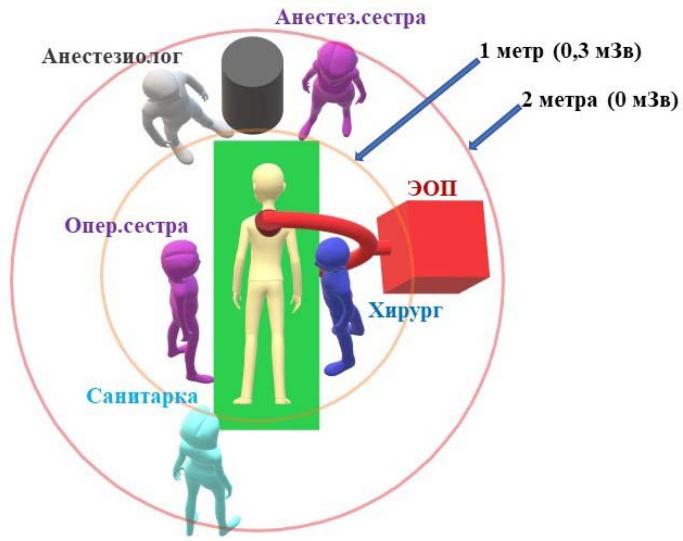 Figure 7: Scheme of x-ray radiation spreading in the operating room
This drawing shows the top view of the EOC in the position above the patient. Dosimeters were placed within a radius of 1 and $2\mathrm{m}$ from the center of the EOC x-ray source. In this case the radiation exposure varies not only with the distance (the lowest radiation dose beyond $2\mathrm{m}$ ), but also with the angle of the x-ray source position in the EOC. Thus, the spreading of rays in a vertical plane is practically absent, but when the source is changed to a horizontal position the rays spread over a distance of $1\mathrm{m}$. All radiation dose data obtained in our study are shown in table 2.
Table 2: Table of radiation doses received during the study, mSv
<table><tr><td>Indicator</td><td colspan="6">Spine Department</td></tr><tr><td>Methods of visualization</td><td colspan="2">cervical spine</td><td colspan="2">thoracic spine</td><td colspan="2">lumbar spine</td></tr><tr><td>Radiography (per screw)</td><td colspan="2">0,034</td><td colspan="2">0,075</td><td colspan="2">0,063</td></tr><tr><td>Total radiation dose (by parts for the entire operation)</td><td colspan="2">0,238</td><td colspan="2">2,09</td><td colspan="2">1,14</td></tr><tr><td colspan="7">The area of exposure of the surgeon</td></tr><tr><td>Methods</td><td>eye socket</td><td colspan="2">Neck</td><td>Right arm</td><td>Chest</td><td>Pelvis</td></tr><tr><td>Radiography</td><td>0,08</td><td colspan="2">0,11</td><td>1,31</td><td>0</td><td>0</td></tr><tr><td>Navigation</td><td>0</td><td colspan="2">0</td><td>0</td><td>0</td><td>0</td></tr><tr><td colspan="7">Operating room</td></tr><tr><td>Distance from the x-ray source (during the entire operation), m</td><td colspan="3">1</td><td colspan="3">2</td></tr><tr><td>Radiation dose</td><td colspan="3">0,3</td><td colspan="3">0</td></tr></table>
Thus, the average dose of ionizing radiation received by the injured of both groups in the course of treatment and performing forced x-ray diagnostics was from 40.3 to $74.6 \mathrm{mSv}$ (exceeded the annual radiation exposure for a healthy person by 40 times). Thanks to the use of neuronavigation technologies for spinal operations intraoperative radiation was reduced by 14 times since they performed only 2 control images to clarify the positioning of screws in the vertebral bodies which was $0.15\mathrm{mSv}$. Medical personnel in the operating room were not exposed to ionizing radiation at all. Patients of the control group depending on the damaged spine were intraoperatively subjected to additional x-ray irradiation at a dose of 1.15 to $2.1\mathrm{mSv}$ which is associated with the use of EOC for navigation.
Exposing patients to excessive radiation the doctor of each specialty should understand that it is possible in the long term this radiation may affect the development of neoplastic processes in patients and medical personnel.
Specialists performing surgical interventions using x-ray navigation must use personal protective equipment (aprons and collars) approved by regulatory documents. But despite the measures taken for screening, the surgeon's body remains unprotected places that are exposed to x-ray radiation. For example, the total dose that a surgeon receives for the distal area of the upper limb on average for one operation on the spine or extremities is $1.31\mathrm{mSv}$, and for the eye area (depending on the position of the surgeon from the EOP) $-0.08\mathrm{mSv}$. Having performed about 15 similar operations, the surgeon already significantly exceeds the professional average annual radiation dose established by regulatory documents. At the same time performing surgical interventions using neuronavigation the surgeon receives a minimal x-ray radiation which in some cases is reduced to zero.
In general, in our opinion in terms of the effectiveness, intraoperative radiation safety and ease of use navigation technologies as a means of intraoperative visualization are the most preferable in comparison with standard methods of radioscopy. At the same time the entire medical staff of the operating room can continuously assist in the process of surgery without being exposed to radiation. The operating room increases the working space associated with bulky equipment and wires. One of the important aspects of its application of navigation technologies for intraoperative visualization is the absence of harmful ionizing effects on the operating surgeon.
## V. CONCLUSIONS
1. Neuronavigation technologies can significantly reduce the radiation load on the injured, reduce the ionizing effect on surgeons and operating room support staff to almost zero.
2. When using neuronavigation the surgeon has more opportunities to move around the operating table since there are no bulky devices in the form of an
ionizing radiation source and an EOC receiving panel that restrict these actions.
3. Due to the absence of constant ionizing radiation in the operating room, all its medical personnel (anesthesiologists, nurses, aidmen) can perform their professional duties during surgery without fear of radiation exposure.
Generating HTML Viewer...
References
9 Cites in Article
J Cho,; (2012). Announcements.
Oliver Gautschi,Bawarjan Schatlo,Karl Schaller,Enrico Tessitore (2011). Clinically relevant complications related to pedicle screw placement in thoracolumbar surgery and their management: a literature review of 35,630 pedicle screws.
K Perisinakis (2004). Estimation of patient dose and associated radiogenic risks from fluoroscopically guided pedicle screw insertion / K.
M Silvestre (2007). Complications of thoracic pedicle screws in scoliosis treatment.
Gordon Singer (2005). Occupational Radiation Exposure to the Surgeon.
Y Rampersaud,Kevin Foley,Alfred Shen,Scott Williams,Milo Solomito (2000). Radiation Exposure to the Spine Surgeon During Fluoroscopically Assisted Pedicle Screw Insertion.
N Theocharopoulos (2006). Fluoroscopically assisted surgical treatments of spinal disorders: conceptus radiation doses and risks / N.
N Theocharopoulos (2003). Occupational exposure from common fluoroscopic projections used in orthopaedic surgery / N. Theocharopoulos [et al.
M Ulhaque (2006). Radiation exposure during pedicle screw placement in adolescent idiopathic scoliosis: is fluoroscopy safe.
No ethics committee approval was required for this article type.
Data Availability
Not applicable for this article.
How to Cite This Article
R.V. Yarmoshuk. 2026. \u201cNeuronavigation Assistance. Decreased Radiation Exposure during Spinal Surgery in Patients with Severe Combined Trauma\u201d. Global Journal of Medical Research - D: Radiology, Diagnostic GJMR-D Volume 24 (GJMR Volume 24 Issue D1).
Explore published articles in an immersive Augmented Reality environment. Our platform converts research papers into interactive 3D books, allowing readers to view and interact with content using AR and VR compatible devices.
Your published article is automatically converted into a realistic 3D book. Flip through pages and read research papers in a more engaging and interactive format.
Our website is actively being updated, and changes may occur frequently. Please clear your browser cache if needed. For feedback or error reporting, please email [email protected]
Thank you for connecting with us. We will respond to you shortly.